Dear Editor,
Cholesterol crystal embolism (CCE) is characterized by multi-system organ dysfunction resulting from occlusion of arteries by atheromatous plaque. Most CCE occur following vascular surgery or radiological procedures, and the CCE which occur without history of interventional operation or surgery is often called “spontaneous CCE”.1 However, CCE is commonly accompanied by eosinophilia which is an important characteristic of allergy. Although eosinophilia is generally considered as the secondary reaction after CCE occurring, allergic disease has been proved to be the risk factor of atherosclerotic disease.2-4 So the relationship between CCE and allergy is still deserved to discuss. Here we describe a case of CCE which occurred after the attack of allergic disease. The patient had a long history of allergic disease (allergic asthma and eczema) over 20 years and an acute attack of eczema and asthma before kidney function decreasing. Satisfactory treatment was obtained with only corticosteroid. This case is a direct proof that allergy is not only the secondary reaction, but also be one of the important precipitating factors of CCE.
One month before admission, a 71-year-old male presented with asthma and eczema. Then he had lower limb edema, anorexia, and toe pain. He had a long history of eczema and asthma over 20 years, with no history of chest pain, anticoagulant therapy, cardiac catheterization, or angiography. Urinary sediment showed BLD±, PRO±. Blood chemistry showed renal function insufficiency (BUN: 118.8mg/dL, Cr: 4.28mg/dL). Blood routine showed anemia (90g/L), thrombocytopenia (81x109/L; normal range, 100 to 300×109/L) and eosinophilia (absolute eosinophil count, 1.6×109/L; normal range, 0 to 0.5×109/L). Immunological examination showed increased IgE level (3080IU/mL; normal range, 0 to 165IU/mL). The symptoms got worse gradually and the serum Cr had increased to 6.72mg/dL before admission. On admission, the patient presented with marked lower-extremity pitting edema with bilateral pre-tibial skin eczema. Feet pulses were preserved. The skin temperature of the first one-third of the dorsal feet decreased. Cyanosis was present in the toes with overt tenderness.
On admission, serum creatinine had increased to 7.88mg/dL. Urinalysis showed slight proteinuria (272mg/24h) and increased N-acetylglucosaminidase (29.9U/gCr; normal range, 2-21.6U/gCr). IgE level was very high (3650IU/mL). Doppler ultrasonic imaging study of arteries revealed atherosclerosis and small mural plaques of bifurcations for the common carotid artery, the internal carotid artery and the proximal and middle vertebral artery.
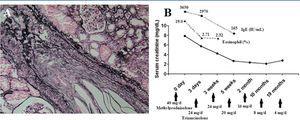
Percutaneous kidney biopsy was performed. The results revealed as follows (Figure 1 A). Among all 12 glomerulus, 5 glomerulus showed ischemic global sclerosis and 2 glomerulus showed ischemic atrophy. Others showed diffuse slight to mild proliferation of glomerular mesangial cells. Multifocal tubular atrophy and interstitial fibrosis were present and accompanied by focal infiltration of mononuclear cells, neutrophils and eosinophils in the interstitium. The most noticeable changes were found within the small arteries, arterioles and vascular pole of the glomeruli presenting with cholesterol crystal gaps. On immunofluorescence, mesangial deposits of FRA (+) were present while IgA, IgG, IgM, C3, and C1q were weak or negative.
Although the creatinine clearance rate (Ccr) was as low as 7.3ml/min/1.73m2, hemodialysis was not administered immediately because of no oliguria. Intravenous methylprednisolone was administered at a dose of 40mg/day. Three days later, the patient’s general condition improved dramatically. Pain of toes was obviously relieved and no further cutaneous lesions appeared. One week after treatment, the skin temperature of feet increased and the cyanosis turned shallower than before. Blood routine showed eosinophil count decreased to 0.18×109/L. Serum creatinine and IgE decreased to 5.57mg/dL and 2970IU/mL, respectively. Oral triamcinolone was given at a dose of 24mg/day. Three weeks after treatment, serum creatinine decreased to 4.26mg/dL. Pre-tibial skin eczema and pain of toes diminished. The temperature of feet skin recovered. Five weeks after treatment, serum creatinine decreased to 2.69mg/dL. Eosinophil count turned normal. Steroids were tapered 10% every 2-4 weeks. Triamcinolone has been tapered to 4 mg/day for maintenance treatment without CCE relapse so far. The serum creatinine of the patient was 2.81mg/dL during last visit (Figure 1 B).
The relationship between CCE and autoimmunity is an interesting issue. Details of the inflammatory response have been documented in animal models that cholesterol emboli could not only mechanically occlude the vessel but also trigger an inflammatory reaction.5 Although the role of immune system in the pathogenesis of CCE was only considered to be an inflammatory response after embolism, opposite proofs have also existed. Recently, there were two important studies which showed a significant correlation between allergic disease and atherosclerosis. In the Bruneck study of 826 middle aged and elderly Italian subjects, the risk for atherosclerosis development and progression increased significantly for 32 subjects with allergic disorders. Furthermore, serum IgE levels were significantly raised in subjects in whom atherosclerosis had developed or progressed.2 In the ARMY study which took 141 male Austrian subjects aged 17 and 18 years, the vascular intima-media thickness (IMT) measured by ultrasonography of the 34 subjects diagnosed as having allergic disease was higher than the healthy subjects.2,3 Although the exact mechanism is still not fully understood, components of the allergic process such as leukotrienes and mast cells may be involved in atherogenesis.2 Furthermore, IgE has been proved to be able to promote atherogenesis in Apoe-/- mice.4
There has not been a definite consensus of the treatment of CCE by now.6,7 Although the use of corticosteroid is still controversial, our patient received only corticosteroid treatment without other above drugs and satisfactory results were obtained. Previous reports indicated that Anticoagulant therapy, which is generally essential in hemodialysis, was harmful to patients with CCE because it was a potent risk factor for plaque rupture and cholesterol embolism.8 Since the present patient was cured successfully with corticosteroid, hemodialysis was avoided and the renal function kept stable to date. So we think treatment with corticosteroid should be a recommended alternative for patients with CCE, especially for patients who had obvious allergic conditions.
Conflict of interest
The authors declare that there is no conflict of interest associated with this manuscript.
Figure 1. The kidney biopsy and clinical course of the patient