Objetivo: Analizar las concordancias en el filtrado glomerular (FG) estimado con las ecuaciones de CKD-EPI y MDRD-IDMS en una cohorte de pacientes hipertensos. Métodos: Se incluyeron 478 hipertensos consecutivamente, edad media 57,58 años (DE = 12,34), el 68,3% hombres. La estimación del FG se realizó con las ecuaciones de MDRD-IDMS y CKD-EPI, valorando las concordancias entre ellas. Resultados: La estimación de FG con CKD-EPI fue 4,37 ml/min/1,73 m2 (IC 95%, 3,73-4,19) superior al MDRD-IDMS en global y por sexos (hombres 3,99; mujeres 5,04). En menores de 65 años la diferencia fue mayor, 6,55 ml/min/1,73 m2 (IC 95%, 5,95-7,15), tanto en hombres (6,07) como en mujeres (6,48). Sin embargo, en mayores de 65 años no se encontró diferencia significativa. El coeficiente de correlación intraclase fue 0,904 (IC 95%, 0,886-0,919), en hombres 0,897 y en mujeres 0,917, y el índice kappa fue 0,848 (IC 95%, 0,795-0,889), en hombres 0,845 y en mujeres 0,852. Conclusión: La ecuación de CKD-EPI estima un FG más alto en mayores de 65 años y reclasifica hacia estadio 1 a hipertensos catalogados en estadío 2 por MDRD-IDMS.
Objective: To analyze the agreement in glomerular filtration rate (GFR) estimated with CKD-EPI and MDRD-IDMS equations in a cohort of hypertensive patients. Methods: We included consecutively 478 hypertensive patients, mean age 57.58 yr (SD: 12.34), 68.3% males. The estimation of GFR was performed with MDRD-IDMS and CKD-EPI equations and we analyzed the agreement between them. Results: The estimation of GFR with CKD-EPI was 4.37 (95%:3.73-4.19) mL/min/1,73 m2 higher than MDRD-IDMS, overall and by gender (males 3.99; females 5.04). In patients under 65 years the difference was greater, 6.55 (95%:5.95-7.15) mL/min/1.73 m2 in both men 6.07 and women 6.48. However, we found no significant difference over 65 years. Intraclass correlation coefficient was 0.904 (95%CI:0.886-0.919), 0.897 men and 0.917 women and Kappa index 0.848 (95% CI :0.795-0.889), 0.845 men and 0.852 women. Conclusion: CKD-EPI equation estimated a higher GFR in hypertensive patients under 65 years and reclassified in stage 1 patients classified in stage 2 by MDRD-IDMS.
INTRODUCTION
Chronic kidney disease (CKD) is a health issue that affects 10% of the adult population1-5 and more than 30% of the patients diagnosed with essential hypertension (HTN).6
The glomerular filtration rate (GFR) is the best indicator to assess renal function in hypertensive patients, but it is not easy to measure in clinical practice. Therefore, several equations have been developed to estimate the GFR. The most widely used equations include: the Cockroft-Gault equation,7 which overestimates the GFR at low values and presents a large dispersion of data, and the MDRD study equation8 (Modification of Diet in Renal Disease), which is currently recommended by the Spanish Society of Nephrology (SEN)9 as it is more accurate when estimating the GFR, both in its traditional version (MDRD) and the MDRD-IDMS version (Modification of Diet in Renal Disease-Isotope Dilution Mass Spectrometry), according to the analytical method used in creatinine determination. However, the MDRD equation has a number of limitations arising from the fact that the study was developed in patients with chronic kidney disease,10 and as such, its main limitations are imprecision and systematic underestimation, especially for GFR values greater than 90 mL/min 1.73 m2.
At present, the CKD-EPI group (Chronic Kidney Disease Epidemiology Collaboration) has published a new equation for estimating the GFR, developed from a population of 8,254 individuals, which includes serum creatinine, age, gender and race as variables, with different versions depending on ethnicity, gender and creatinine value. According to the authors, the results of this equation are more accurate and precise than those of the current by-choice equation, i.e. the MDRD-IDMS equation, especially for GFR values above 60 mL/min/1.73 m2 in a group of 3,896 individuals.11
The aim of this study is to compare the GFR values estimated using the new CKD-EPI equation in relation to the MDRD-IDMS equation in a cohort of hypertensive patients and to analyse the correlation between the two equations.
MATERIALS AND METHODS
Design and population
Cross-sectional descriptive study carried out in the field of primary healthcare at the La Alamedilla Research Unit. All Caucasian patients between 30 and 80 years old with a clinical diagnosis of HTN over the past five years who signed the informed consent form were included consecutively from December 2005 to June 2009. The excluded patients were those who met one of the criteria for which the use of equations to estimate the GFR is not appropriate: extreme body weight (BMI below 19 kg/m² or above 35 kg/m²), major alterations in the muscle mass (amputations, loss of muscle mass, muscle disorders or paralysis), acute renal failure, pregnancy, severe liver disease, generalised oedema and ascites.1,12
Variables analysed
We analysed age, gender, family history of premature vascular disease, smoking habit, diabetes mellitus, cerebrovascular disease and ischaemic heart disease. The determinations of creatinine and glucose in the blood and the albumin-creatinine index were carried out blindly at the reference laboratory after at least eight hours of fasting.
The examinations carried out included: weight, height, waist circumference and blood pressure measured with an OMRON M7 sphygmomanometer (Omron Healthcare, Kyoto, Japan), which was certified according to the recommendations of the European Society of Hypertension.13
The estimation of the GFR11 was performed with the MDRD-IDMS equation, where GFR = 175 x (serum creatinine)-1.154 x age-0.203 x (0.742 if female),8 and the CKD-EPI equation, with the following equations for Caucasian patients:
For women with creatinine <0.7 mg/dL (62 mmol): GFR = 144 x (cr/0.7)-0.329 x (0.993)age.
For women with creatinine >0.7 mg/dL (62 mmol): GFR = 144 × (cr/0.7)-1.209 x (0.993)age.
For men with creatinine <0.9 mg/dL (80 mmol): GFR = 141 x (cr/0.9)-0.411 x (0.993)age.
For men with creatinine >0.9 mg/dL (80 mmol): GFR = 141 × (cr/0.9)-1.209 x (0.993)age.
Statistical analysis
The characteristics of the patients studied were described using central tendency and dispersion measures for the quantitative variables and percentages for the qualitative variables. The Student’s t-test was used for independent data in order to compare quantitative and qualitative variables of two categories, while the chi-square test was used for the qualitative variables.
In the end, we used the intraclass correlation rate to assess the correlation between the two equations. The population was subsequently divided into the five stages of chronic kidney disease of the National Kidney Foundation,14 using the kappa index to evaluate the correlation in the classification of patients among the different categories. We used the Bland-Altman plot for the graphic representation of the correlation between the CKD-EPI and MDRD variables. All the tests were carried out using the statistical software SPSS/PC+, version 15.0 (SPSS Inc., Chicago, Illinois, USA).
RESULTS
Table 1 shows the characteristics of the hypertensive patients studied, as well as the cardiovascular risk factors, the serum creatinine values, the albumin-creatinine index and the GFR estimated using both equations for the total group and according to gender. The average progression of the disease was 3.41 years, while the percentage of patients on medication for hypertension was 55.6%. The range of creatinine ranged between 0.5 and 2.4 mg/dL.
The GFR mean in the whole sample estimated using the CKD-EPI equation was 4.37 mL/min/1.73m2 (95% CI, 3.73 to 4.19), higher than that of the MDRD-IDMS equation. It was also higher in women (5.04 mL/min/1.73 m2 [95% CI, 4.07 to 6.01]) and in men (3.99 mL/min/1.73 m2 [95% CI, 3.13 to 4.79]). In addition, these differences were also similar in those younger than 65 years, with the GFR being higher in the total sample when measured with the CKD-EPI equation: 6.55 mL/min/1.73 m2 (95% CI, 5.95 to 7.15). Finally, in the same age group, the GFR in women was 6.48 mL/min/1.73 m2 (95% CI, 6.50 to 8.44) and 6.07 mL/min/11.73 m2 (95% CI, 5.32 to 6.81) in men.
However, although the MDRD-IDMS equation estimated the GFR in men slightly higher (1.84 mL/min/1.73 m2 [95% CI, -0.002 to 3.67]) and in women slightly lower (0.70 mL/min/1.73 m2 [95% CI, -2.31 to 0.90]), the CKD-EPI equation found no significant differences between the two methods among those over 65 years of age. The percentage of occult renal disease estimated by the two equations was 5% higher in women than in men, while age was higher in both men and women (Table 1). The correlation coefficient between the two equations was 0.904 (95% CI, 0.886 to 0.919), with 0.897 in men (95% CI, 0.873 to 0.917) and 0.917 in women (95% CI, 0.890 to 0.937).
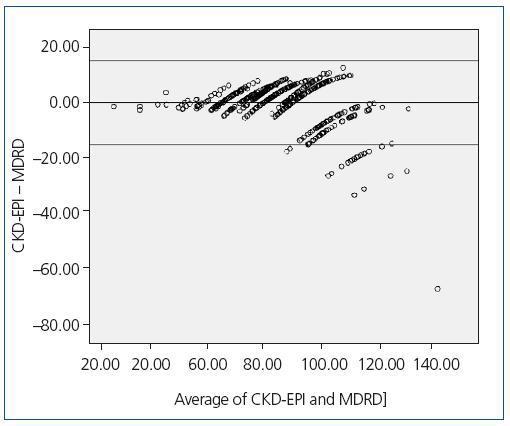
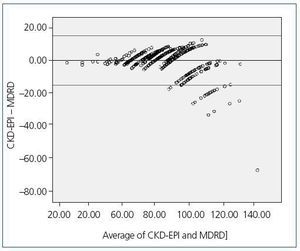
The correlation in the classification of the CKD stages was lower in stage 1 (82.04%), where the CKD-EPI equation classified a greater percentage of hypertensive patients, whereas the MDRD-IDMS equation classified a higher percentage of patients (86.35%) in stage 2. In stages 3 and 4, the correlation was 92.09% and 100%, respectively. Finally, in stage 5, no patient was classified by any of the two equations. The kappa index was 0.848 (95% CI, 0.795 to 0.889). This index was higher in women (0.852 [95% CI, 0.778 to 0.926]) than in men (0.845 [95% CI, 0.786 to 0.904]). Figure 1 shows the correlation for the CKD-EPI and MDRD variables, with a -0.86 mean value of differences, and the limits of agreement.
DISCUSSION
The results of this study indicate that if the GFR is estimated with the new equation, the rate in hypertensive patients is 4.37 mL/min/1.73 m2 higher than the rate obtained with the MDRD-IDMS equation.8 These differences increase in those under 65 years of age to 6.55 mL/min/1.73m2, in both men (6.07) and women (7.47). However, there were no differences between the two equations in the total group or according to gender in patients over 65 years of age. This increase in the GFR value results in a reclassification of the patients to higher stages, especially concerning the CKD-EPI equation,11 which classified a higher number of hypertensive patients in stage 1, whereas the MDRD-IDMS equation8 classified them in stage 2.
The intraclass correlation coefficient between the GFR rates estimated by both equations was 0.904 (95% CI, 0.886 to 0.919), while the kappa index concerning the classification of the different stages of renal failure was 0.848.
This 4.37 mL/min/1.73 m2 difference in the GFR of hypertensive patients between the two equations is smaller than the data presented from the application of the CKD-EPI equation11 on the study population (the National Health and Nutrition Examination Survey – NHANES, 1999-2006).1 In the latter, the value of the GFR from the new equation was 9.5 mL/min/1.73 m2 higher than those obtained with the MDRD-IDMS equation,8 showing a prevalence rate of chronic kidney disease (CKD) of 11.5% compared to 13.1%. This prevalence rate is lower than that in this study, which was 14.4% and 15.9% in the CKD-EPI and the MDRD-IDMS equations,8 respectively. This datum is logical if we consider that we are analysing hypertensive patients and not the general population.
In a recently published study by Bermudez Montanes R. et al.15 where the GFR values were estimated using the new CKD-EPI equation11 compared with the MDRD-IDMS equation8 in a cohort of 14,427 patients, the average GFR value was 0.6 mL/min/1.73 m2 higher in the CKD-EPI equation11 than in the MDRD-IDMS equation8 in the total group. The value was 1.9 mL/min/1.73 m2 higher for women and 0.2 mL/min/1.73 m2 lower for men. These results are consistent with those obtained in hypertensive patients. Nevertheless, only the CKD-EPI equation11 estimated a lower GFR value in men over 65 years of age. Unlike in our study, the correlation was higher in men.
The use of the ERC-EPI equation11 reduces the prevalence of women diagnosed with CKD, which is one of the problems with the MDRD-IDMS equation,8 which underestimates the GFR in elderly people and in women, thus increasing the diagnosis of CKD in these groups.16 However, there seems to be no improvement of the prevalence in elderly people.
The main contribution of this study is that it constitutes the first publication that analyses the new CKD-EPI equation in hypertensive patients within the Spanish primary healthcare system. The major limitation is the lack of knowledge of the true GFR value, since we do not have a direct measurement from a standard method. Another limitation that we cannot overlook is whether the performance in the upper stages is the same, since only one patient reported a GFR value lower than 30 mL/min/1.73 m2.
To conclude, we believe that until we have results of longitudinal studies to confirm the data this equation can be used in the clinical practice to estimate the GFR in hypertensive patients. We base our conclusion on the fact that the results obtained in hypertensive patients are consistent with those published by other authors.11,15 In addition, the new CKD-EPI equation11 for the estimation of GFR reclassifies a considerable number of hypertensive patients, mainly younger ones, to stages with a higher GFR value. It therefore yields more accurate and precise results than the MDRD-IDMS equation.8
Figure 1. Bland-Atmann graph
10321_108_7347_en_w477710395410321_18107_2043_es_10321_15491_2043_es_tabla_1_copy1_en.doc
Table 1. General characteristics and gender of the hypertensive patients studied
10321_108_7348_en_w477710395510321_18107_2044_es_10321_15491_2044_es_tabla_2_en.doc
Table 2. Correlation in the classification of the stages of chronic kidney disease between the estimated glomerular filtration rates of the MDRD-IDMS and CKD-EPI equations