To look at transplant coordinators’ professional narratives and explore their emotional experiences, coping strategies, needs and demands in relation to the donation interview.
MethodsExploratory, transversal, multicenter design, using grounded theory qualitative approach and content analysis of open-ended questionnaire and semistructured interviews with 22 transplant coordinators from the Andalusian Public Health System. Categories of analysis: Transplant coordination: perceptions, functions, impact and consequences; Positive/gratifying aspects and negative/difficult aspects; Donation interview; Coping strategies; Needs, demands and suggestions.
ResultsTransplant coordinators maintain a polarised perspective on their work, which they describe as a challenge and an opportunity. They highlight both their satisfaction and professional commitment as work difficulties and requirements, representing stress factors with an impact on professionals’ perceptions, life styles, identity or physical and psychical life. Most gratifying work aspects refer to professional excellence, successful transplants and relationship with patients and their families. The donation interview is considered to be the most stressful moment, in response to which coordinators develop different emotional paths, conditioned by their experience, families’ response to donation and its interpretation by the health team and professional (self) evaluation. Main professional demands are training strategies, group therapies and institutional support.
ConclusionsThe complexity and emotional intensiveness of transplant coordination require special interventions aiming to enable professionals towards an improvement of their emotional heath and management.
Conocer las experiencias en la práctica profesional de equipos de coordinación de trasplantes, y explorar sus vivencias emocionales, estrategias de afrontamiento, necesidades y demandas en relación a la entrevista de donación.
Materiales y métodosDiseño exploratorio, transversal, multicéntrico, con metodología cualitativa, basado en la Teoría Fundamentada y análisis de contenido de cuestionarios con preguntas abiertas y entrevistas semi-estructuradas, realizado con 22 profesionales pertenecientes a equipos de coordinación de trasplantes del Sistema Sanitario Público de Andalucía. Las categorías empleadas en el análisis fueron: Trabajo de coordinación: percepciones, funciones, impacto y consecuencias; Aspectos positivos/ gratificantes y negativos/difíciles de la coordinación de trasplantes; La entrevista de donación; Estrategias de afrontamiento; Necesidades, demandas y propuestas.
ResultadosLos equipos de coordinación de trasplantes tienen una visión polarizada sobre su trabajo, que describen como reto y oportunidad, evidenciando su satisfacción y compromiso profesional y, por otra parte, las dificultades y exigencias que representan factores de estrés con impacto en sus percepciones, estilos de vida, identidad profesional o salud física y psíquica. Los aspectos más gratificantes se relacionan con la excelencia profesional, trasplantes exitosos y la relación con pacientes y familiares. La entrevista de donación es el momento de mayor estrés, ante el cual se generan diferentes rutas emocionales, condicionadas por la experiencia en la coordinación, la respuesta familiar y su interpretación y la autoevaluación profesional. Las principales demandas profesionales se orientan hacia estrategias formativas, terapia grupal y apoyo institucional.
ConclusionesAnte la complejidad e intensidad emocional del trabajo de coordinación, se requieren intervenciones de capacitación para mejorar la salud y gestión emocional de sus profesionales.
Since the Transplant Act (1979) and the founding of the National Transplant Organisation (1989), Spain has become and remained one of the countries with the highest rates of organ donation and transplantation worldwide.1 The transplant model, exported internationally, works via a complex, consolidated system based on solid intra- and interhospital organizational and technological coordination, the efforts of an "excellent coordinator network"2 (p. 459), and a wide social acceptance.3
The commitment, experience, and preparation of the transplant coordination teams are key for ensuring clinical and organisational operations, relationships and communication with society, and high donation rates.4 However, the impact of the physical, mental, and emotional requirements of this activity on stress levels, burnout, health, and professional satisfaction has been documented.5–7
The emotional experiences of the health care personnel involved in donations and transplants is built around a series of contradictions and tensions between roles and duties8–10 primarily related to the interaction with patients and family members during the donation interview.11,12
The few available studies in the international literature indicate satisfaction, happiness,8 empathy, and respect10,13 or understanding11 as positive emotions, in contrast with difficult emotional situations, when the professionals experience from surprise, astonishment, or shock11 to sadness and sorrow,8 doubt and discomfort,13 anger,11 and fear of increasing the suffering of the families or seeming insensitive.9
The lack of skills and training resources to adjust strategies for coping, denial, or controlling how emotions are expressed also make it difficult to identify and manage emotions, with an implicit risk for the professionals' mental and emotional health.14
At present, no conclusive studies on the emotional experiences of the coordination teams are available at the national level, and this is particularly relevant for giving voice to those transplant coordination teams and collecting their opinions and proposals.
In this sense, the study objective is to learn about the experiences in the professional practice of the transplant coordination teams, as well as explore their emotional experiences, coping strategies, needs, and demands related to the donation interview.
Participants and methodsAn exploratory, cross-sectional, multi-centre design, with qualitative methodology, conducted in 2018 in Andalusia using a grounded theory approach based on analysing the contents of questionnaires with open-ended questions and semi-structured interviews with 22 transplant coordination team professionals.
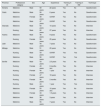
The study population included a total of 51 professionals belonging to sector and inter-hospital teams from Andalusian Regional Transplant Coordination. With prior authorisation from the responsible organisation, the study population was contacted by e-mail, through the Regional Coordination, which provided information about the objectives and methodology, and requested voluntary participation in the study, proposing a 2-week period to complete the online questionnaire with open-ended questions. The response rate was 22%, with 11 professionals having participated (Table 1).
Study participants.
| Province | Professional category | Sex | Age | Experience | Training in DI | Training in EM | Technique |
|---|---|---|---|---|---|---|---|
| Almería | Medicine | Male | 59 years | 22 years | Yes | No | Questionnaire |
| Cádiz | Medicine | Male | 56 years | 6 years | Yes | No | Questionnaire |
| Medicine | Female | 49 years | UK/NR | Yes | No | Questionnaire | |
| Medicine | Male | 47 years | UK/NR | Yes | No | Questionnaire | |
| Granada | Medicine | Male | 50 years | 10 years | Yes | No | Interview |
| Nursing | Male | 62 years | 27 years | Yes | No | Interview | |
| Huelva | Medicine | Male | 46 years | 9 years | Yes | No | Questionnaire |
| Nursing | Female | 56 years | 25 years | Yes | No | Questionnaire | |
| Jaén | Medicine | Male | 44 years | 7 years | Yes | No | Questionnaire |
| Málaga | Medicine | Male | 51 years | 20 years | Yes | No | Questionnaire |
| Nursing | Male | 43 years | UK/NR | Yes | Yes | Questionnaire | |
| Medicine | Male | 56 years | UK/NR | Yes | Yes | Questionnaire | |
| Seville | Medicine | Male | 43 years | 2.5 years | Yes | No | Questionnaire |
| Nursing | Female | 43 years | 6 months (ex) | Yes | No | Interview | |
| Nursing | Female | 40 years | 1 year | Yes | No | Interview | |
| Nursing | Female | 47 years | 18 years | Yes | No | Interview | |
| Nursing | Female | 46 years | 2 months | Yes | No | Interview | |
| Nursing | Male | 44 years | 1 year | Yes | Yes | Interview | |
| Medicine | Female | 50 years | 10 years (ex) | Yes | No | Interview | |
| Medicine | Female | 34 years | 1.5 years | Yes | No | Interview | |
| Medicine | Male | 38 years | 3 years | Yes | No | Interview | |
| Medicine | Male | 55 years | 7 years | Yes | No | Interview |
| Mean age | Mean experience | ||||||
|---|---|---|---|---|---|---|---|
| Total | 14 medicine professionals | 11 male | 49 years | 10 years | – | – | – |
| 3 female | 45 years | 6 years | – | – | – | ||
| 8 nursing professionals | 3 male | 50 years | 14 years | – | – | – | |
| 5 female | 46 years | 9 years | – | – | – |
For the semi-structured interviews, intentional sampling was used with collaboration from 2 key informants, regional transplant coordinators, who facilitated selecting and contacting 9 professionals, chosen according to criteria so as to have heterogeneous profiles by sex, age, professional category, age, years of experience, hospital and province level, specific training in emotional management, and religious/spiritual beliefs. This population was completed using the snowball technique, with 2 ex-coordinators who belonged to the transplant teams in the last 2 years and who voluntarily left this position (Table 1). The participants were contacted by telephone and all agreed to participate in the study. The interviews took place at the hospitals where they worked, and had a mean duration of 45−60 min, they were recorded in audio format and transcribed literally.
All participants signed an informed consent form, including information about the objectives and methodology and ensuring confidentiality.
The questionnaire with open-ended questions and the interview guide were designed based on pre-established, self-created categories, coming from a literature review, which demonstrated the most relevant dimensions of emotional experiences and management among donation and transplant professionals (Table 2).
Dimensions of the interview script/questionnaire with open-ended questions.
| Theme/dimension | Aspects and questions |
|---|---|
| Transplant coordination work | How is/how would you describe the transplant coordination work? |
| Duties, roles, requirements, description | |
| Organisational structure, pressures, relationship with the rest of the team and professionals, work rhythms | |
| How can the transplant coordination work change you or influence how you think, act, or see the world? | |
| Influence on personal, family, professional, social life, etc. | |
| Motivation for becoming part of the coordination team | Why did you become part of the coordination team? |
| Expectations, image of the job, motivation | |
| Positive/gratifying aspects | What are the most gratifying moments, experiences, or circumstances? |
| Description, thoughts, and own and others' feelings | |
| Negative/difficult aspects | What are the hardest moments, experiences, or circumstances that you usually confront in your transplant coordination work, or those with the greatest emotional burden? |
| Description, thoughts, and own and others' feelings | |
| What was the most disagreeable situation, or the one with the greatest psychological impact, that you have had to face in your transplant coordination work? | |
| Describe a specific case, its implications and emotional consequences, thoughts, actions, and perceived emotions | |
| The donation interview | How do you do feel when you have to do a donation interview? |
| What emotions usually come to the fore in you? | |
| When do these emotions appear? Before, during or after the interview? | |
| What are you thinking in that moment? How do you usually act? What happens after, that is, what are the consequences of your action? | |
| Do you believe that some people who work in transplant coordination can come to consider leaving behind the emotional burden they carry? Do you know any personal cases? | |
| Coping strategies | What thoughts, activities, actions do you carry out to reduce the emotional burden of your work? |
| Needs, demands, and proposals for emotional management and training | What do you believe that you would need or could help you to manage the emotions resulting form your work and lighten your psychological burden? |
| How do those emotions influence your personal and family life? | |
| What strategies/tools/emotional management skills would be most relevant for you? | |
| Socio-demographic data | Age, sex, city, professional category, specialised training related to the donation interview, training in self-managing emotions or psychological health, years on the transplant coordination team, religious/spiritual beliefs |
The interview contents and open-ended questionnaire questions were analysed using the Nudist Vivo software, based on pre-established and emerging categories (identified in the discussions with professionals), on the basis of the theoretic precepts of grounded theory (focused on social interaction as a basis for understanding social phenomena) and the constant comparative method, as applied to health care.15–17 The analysis phases were: reading and systematically organising the information, coding it into the tree of pre-established and emerging categories, recording, reorganising, and defining definitive categories in a theoretical framework, and triangulating results between members of the team and based on the individuals interviewed.
The quality and validity criteria were checked according to the recommendations for qualitative research shown in Sandin18 and Morse.19
Results"Challenge and opportunity in equal parts". Transplant coordination: perceptions, duties, and impact
Transplant coordination work is described from a polarised viewpoint which makes clear its complexity and exposes the satisfaction and commitment of its professionals, on the one hand, and its difficulties and requirements, on the other. Table 3 presents the main duties of the coordination teams, as well as their consequences and impacts on perceptions, lifestyles, identity, and occupational health. "The wheel keeps turning". Most gratifying and difficult aspects of transplant coordination
Transplant coordination: perceptions, duties, and impact/consequences.
| Topic | Results | Verbatim quotes |
|---|---|---|
| [15,0]Transplant coordination work | [15,0]Dual perception. Satisfaction, pride, complexity, importance, recognition-versus-Stress, responsibility, tiredness, pressure, difficulties, requirements | "Complex, systematised, and broad. Essential work" (Q/physician/56 years/6 years) |
| "Very satisfactory and at the same time intense and stressful regarding the organisational logistics" (Q/physician/43 years/UK/NR) | ||
| "Very satisfactory and gratifying in human and professional terms" (Q/physician/43 years/UK/NR) | ||
| "Very satisfactory when everything goes well, perhaps too high a workload" (Q/physician/59 years/22 years) | ||
| "Very stressing, sometimes it overwhelms you" (Q/nurse/56 years/25 years) | ||
| "It involves dedication to humans and management and it takes away much of your life, dealing with the family is very hard at first, you leave a donation and you are exhausted. (…) If you are not very hopeful, and the negative burden is not cancelled out by that hope for me, I have to leave, it is something that needs a lot of hope, if not, it is impossible" (I/nurse/47 years/18 years) | ||
| "The first is a professional and personal challenge, also an opportunity, a challenge and an opportunity in equal parts" (I/nurse/44 years/ 1 years) | ||
| "For me it's been a pleasure, from the professional and much more the personal perspective (…) by realizing that I am capable of helping people (..) but it is physically, emotionally exhausting (…) that there, on balance, that truly, today… I don't know what to do…"(I/nurse/40 years/1 year) | ||
| "I really like it at the professional level, it is an opportunity, I like the stress, the participation, and difference between the days, there are no established rules, it's very dynamic…"(I/nurse/47 years/18 years) | ||
| "Being a link in the chain, I like it… I see a documentary on transplantation and I start to cry and I like being part of this family" (I/nurse/46 years/0.2 years) | ||
| "For me it is a very stressful thing, very exhausting, physically and mentally, but at the same time very comforting. And very complex" (Q/physician/34 years/1.5 years) | ||
| "It requires unyielding ethics (…), that within the hospital you have all the support of your management team and you gain the support of your team and gain the respect of others, it is a very demanding job" (I/ex-coordinator/physician/50 years/10 years) | ||
| "You are the only people in the hospitals who has contact with the family that donated, you are the one who represents everything that they are saying and you are the one who gives the bad news. A person who gives them bad news like the death of a patient, they will never forget your face, that is a large responsibility" (ex-coordinator/physician/50 years/10 years) | ||
| "…I remember it being very stressful. Then I loved it, a double-edged sword, recognition and a rush for me, it was a lot of stress, but at the same time it comforted me. There were the most stressful times that I remember (…) it caused me anxiety that meant I couldn't continue, even though loved the experience" (I/ex-coordinator/nurse/43 years/0.5 years) | ||
| "It is a pride (…), how one more step in the scale in the complexity that it has, in the repercussion and importance that it has (…) That is what motivates you and makes it so that it does not take as much personal and professional effort" (I/physician/38 years/3 years) | ||
| "There is a lot of pressure to continue being the best, it is difficult to balance because the treatment pressure to get people off the waiting list is very big…" (I/nurse/62 years/27 years) | ||
| [15,0]Transplant coordination roles | [7,0]Donation interview. Detecting donors. Procuring organs. Informing and accompanying families | "The essential role is to detect possible donors (…) then what we do is evaluate what organs could be donated" (I/physician/50 years/10 years) |
| "The mission is to get donors, that is the mission of a coordinator, we won't fool ourselves" (I/ex-coordinator/physician/50 years/10 years) | ||
| "Our ultimate goal is to get organs so they can be transplanted" (I/nurse/62 years/27 years) | ||
| "In the donation interview, well you do it, you ask for the organs and you give support to the family informing them about the process" (I/nurse/44 years/1 year) | ||
| "You are going to help them, support them, but your objective is to ask the question and to know how to fit in at any time" (I/nurse/40 years/1 year) | ||
| "They feel accompanied, they have the possibility of saying goodbye to their family member, we help them with the funeral (…), we give them our telephone number…" (I/nurse/40 years/1 year) | ||
| "When you see a person suffering that way, you can't go running out, you have to stay with them and keep them company, sometimes that company is by hugging them, not hugging them, letting them cry, or turn their back (…) and you focus yourself on being able to answer all the questions that they have (…), helping them understand that the situation is irreversible (…), that everything possible has been done and that the person suffered as little as possible (…) I try to dispel all doubts" (I/physician/38 years/3 years) | ||
| "I want them to be well informed about everything and all their fears resolved, (…) I try to calm them down (…) let them say what they want, I do not have to give them solutions, I let them talk and help them for that time to be together" (I/nurse/47 years/18 years) | ||
| [1,0]Internal and external social impact: Social campaigns. Raising awareness among professionals, generating and consolidating a pro-donation professional culture | "We participate in donation promotion activities, in the media, in institutes, in different types of associations" (I/physician/50 years/10 years) | |
| "My basic job was to detect potential donors and to create a culture, when there wasn't one, that we can all be donors. That cultural change that was very clear outside the hospital, Spanish society was very clear about it, within the hospital, no. Since physicians and nurses, very good professionals, did not take it into account when a patient reached the end of their life…, the possibility wasn't offered. That was my first mission as an intra-hospital medical coordinator" (I/ex-coordinator/physician/50 years/10 years) | ||
| [1,0]Bringing together and motivating the team | "You have to build the team. (…) I'm an optimist by nature and I let myself be overwhelmed for an hour or two, no more, I don't like to carry a burden for very long, I have everyone in my kit and I know it…" (I/ex-coordinator/physician/50 years/10 years) | |
| "You help your colleagues, resolve their doubts…" (I/nurse/44 years/1 year) | ||
| [3,0]Organisation, quality, safety, follow-up | "All the logistics…" (I/nurse/44 years/1 year) | |
| "We have to review, manage time, continue with the protocol…" (I/physician/38 years/3 years) | ||
| "We organise all the logistics of the operating theatre… Since one team comes in to operate at this time, another one comes in at that time, if there is an absolute emergency then you have to call the airport that will receive a plane of surgeons form Coruña… We make sure that everything goes well for the surgeon, that nothing happens, that the organs and tissues are removed and stored correctly for transfer, we do a quality control on the subsequent outcome of those organs, we send the family a letter after 3–6 months asking how things are going…" (I/physician/50 years/10 years) | ||
| "…managing mobile teams, managing and fighting because you need to get the operating theatre opened up, set up parallel operating theatres, the staff doesn't answer, time is running out" (I/ex-coordinator/nurse/43 years/0.5 years) | ||
| [24,0]Impact and consequences of coordination work | [11,0]Change of perspective on life and death: Awareness of the unpredictability of death. Objectiveness and rationality. Ability to downplay. Appreciate and enjoy life | "You undoubtedly see things differently, in the sense that you are fully aware that you are here today and not tomorrow (Q/nurse/43 years/UK/NR) |
| "I leave here thinking that I could die at any time" (I/physician/34 years/1.5 years) | ||
| "Seeing death that comes so suddenly, like a life cut short and how their loved ones experience it, it is very hard and you cannot stay indifferent" (Q/physician/56 years/6 years) | ||
| "The sadness, sometimes how heavy it feels to see how life ends in such an absurd way, it discourages me and there is no lack of desire to leave it all" (Q/physician/56 years/6 years) | ||
| "In life we are only prepared to live and we barely talk about death because of fear. And the fact of seeing it so close makes you be more objective. I believe that you become more rational in the face of adversity" (Q/nurse/56 years/25 years) | ||
| "I came to feel defenceless, you are exposed to things that can happen to you that you cannot control… you have to think that these are the rules of the game and that we are all playing, it is absurd to protect yourself, impossible to control everything" (I/nurse/44 years/1 year) | ||
| "It has changed me, everything is more relative. How I deal with the families has changed and my vision of day-to-day life is more relative, more idealistic" (Q/physician/56 years/UK/NR) | ||
| "Over time it changes your concept of life, but I believe that it has influenced it in a positive way" (Q/physician/43 years/2.5 years) | ||
| "It has changed how I enjoy life, seeing young people die makes you say that here are two days and you have to enjoy them and it's good" (I/nurse/46 years/0.2 years) | ||
| "You become aware of how little value everything else has, you value the things as they should be and you enjoy the happiness from the small things and not absolute happiness" (I/nurse/44 years/1 year) | ||
| "When you get home, see your family, you see your wife, you see your kids, you see your parents, and you say "wow, how lucky we are"…" (I/physician/38 years/3 years) | ||
| "Each time I am more positive and I see more… that nothing is transcendental, everything is much more relative, my life, I have three or four clear things that I want and those are my objectives, but three days or five, the times are short, yes, it has changed me in that respect" (I/nurse/47 years/18 years) | ||
| [5,0]Impact on social and family life | "In the end everything that we live leaves a trace that alters us in all facets of our life. From the start, all my small children know what donation is, what a donor is, and they declared themselves organ donors. Sometimes frustration, or simple tiredness, accompanies you home and those changes in how you see life materialize in changes in your day-to-day life. Sometimes it makes me want to appreciate my own loved ones and enjoy being with them" (Q/physician/46 years/9 years) | |
| "I think that I enjoy the little time I have left more than before being on the coordination [team]" (I/physician/34 years/1.5 years) | ||
| "If I've had a bad day, I'm not capable of going to the cinema, or going to eat with my family… Or I don't want to and I end up fighting with everyone…" (I/physician/34 years/1.5 years) | ||
| "When you are on-call, you always have the mind set of "if they call me now"…, you feel that pressure from the start, and it progressively dissipates… that hyperresponsibility blocks you from leading a normal life" (I/physician/38 years/3 years) | ||
| "Everything around you and your family life and leisure revolves around this… I remember my ex, he had nightmares that the day of my wedding they would call me for a transplant… we never ended up marrying" (I/nurse/44 years/1 year) | ||
| "At home I talk about donation in a positive and pleasant way, but my family has no reason to live my work or my fears. And we talk about death as something natural, my children ask me "are you going today?" and I tell them "yes, I'm going because I have death", I tell them that" (I/nurse/47 years/18 years) | ||
| [2,0]Image and professional identity and conflict of professional roles | "We're sort of freaks because we have a weird job, you know? It's the unknown and it's difficult to understand what we dedicate ourselves to, some might even think that we are vultures, scavengers…" (I/physician/50 years/10 years) | |
| "The type of work as an Emergency physician, where you "save" lives and as a coordinator, it was not easy at the beginning to look after "deceased" people" (Q/physician/49 years/UK/NR) | ||
| "It's the dichotomy of leaving here (from the interview) with the pain of having shared something as bad as it has to be to lose a child in hours… but I leave here saying "hey, 36-year-old donor, heart, pancreas, liver…"" (I/nurse/40 years/1 year) | ||
| [3,0]Physical and mental health | "Sometimes I have had low blood sugar, the blues in general" (Q/nurse/56 years/25 years) | |
| "(…it affected me a lot) Because of the hours and I left because it did not let me rest, I wasn't able to detach myself, I was very stressed out, it wore me out thinking a lot about "tomorrow I'm on-call for 24 hours, I don't know what will happen at any time day or night". (…) as feelings I am experiencing it now with a pit in my stomach, shortness of breath, distress, anxiety (…), being without sleep, with this feeling all day (…). What I felt was that, sensations of distress, of not being able to sleep, nervousness and restlessness, from the day before I couldn't sleep, I wasn't calm, I didn't leave my house, I didn't go to the supermarket in case they called me…" (I/ex-coordinator/nurse/43 years/0.5 years) | ||
| "At first I couldn't sleep at two in the morning, I came in early and reviewed notes (I/nurse/46 years/0.2 years) | ||
| "Eventually some time ago, I was noting a feeling of being overwhelmed, tachycardia, palpitations, insomnia. (…) I told my doctor "Could this be because of anxiety?" And it surely was, surely" (I/nurse/40 years/1 year) |
The identification of the verbatim quotes is given in parentheses in the format: technique (Q: questionnaire; I: interview/professional category/age/experience in coordination).
Table 4 summarises the most gratifying and difficult aspects of the work. The positive aspects include: professional development and access to an excellent specialisation and high social recognition; inclusive, collaborative, multidisciplinary work environment for all professional categories; outcomes and successes in donations and transplants; the quality and emotional intensity and gratification regarding the relationship with patients and family members. The difficult aspects include: communicating deaths, the relationship and emotional impacts of the donation interview, and organisational and professional difficulties. "Asking the question". Emotional experiences around the donation interview
Positive/gratifying aspects and negative/difficult aspects of coordination.
| Topic | Results | Verbatim quotes |
|---|---|---|
| [23,0]Positive/gratifying aspects | [7,0]Professional aspects: Quality, professionalism, training, excellence, compensation. Motivation. Coordination and quality of interprofessional relationships on the coordination team. Collaboration and recognition of medicine and nursing knowledge | "It is an elite team at the hospital which has access to resources for training, executive power (…) a spearhead of medicine, one of the last frontiers of medicine is always the world of transplants, with which they have first-line training, they also have access to first-line technology… They will work a lot and they will be paid more than their colleagues" (I/physician/50 years/10 years) |
| "The possibility of working with teams of people with high levels of motivation and professionalism" (Q/physician/51 years/20 years) | ||
| "Coordinating so many professionals in such a short time" (Q/physician/56 years/UK/NR) | ||
| "Collaboration with all the hospital personnel" (Q/physician/49 years/UK/NR) | ||
| "The people are super motivated, I would almost say that they self-select themselves… those who do not feel capable of living with this predisposition, with this availability is the word, to the hospital… then they end up leaving. But the people who stay are super motivated, very prepared people (…). So being able to work with a human group of this value… when there is a problem, the people don't just look at the group, the people raise their hand and say "I’ll do it" (…), whatever happens, whatever time it is, which makes you say "hey, I'm not alone here, I'm not a crazy person trying to do one thing while everyone is against me" (…), but rather you have people, see, who are voluntarily (…), no one is making them follow…" (I/physician/38 years/3 years) | ||
| "Good dynamics with colleagues have an influence" (I/nurse/62 years/27 years) | ||
| "There is no map of skills between transplant coordination by nurses and doctors, you do this and you do that, we dedicate ourselves to transplant coordination as a whole" (I/nurse/44 year/1 years) | ||
| "(The interview is done by) the transplant coordinator, regardless of whether they are a doctor or nurse. Normally there are two of us, a doctor and a nurse come in…" (I/physician/50 years/10 years) | ||
| [6,0]Transplant outcomes and successes | "Guaranteeing the outcomes from such valuable organs and tissues, it is a big achievement" (Q/physician/56 years/6 years) | |
| "Also when I call the transplant centre and they confirm that the organs were implanted, it is the best after so much stress" (Q/nurse/56 years/25 years) | ||
| "After a donation knowing that the organs have been transplanted, that your efforts were worth it" (Q/physician/49 years/UK/NR) | ||
| "When they tell us that the organ was valid and it was correctly implanted without a problem" (Q/physician/46 years/9 years) | ||
| "The expectation and hope because after such a hard task many people are saved" (I/nurse/47 years/18 years) | ||
| "The most gratifying final outcome of the entire procedure, is that people are transplanted" (I/nurse/40 years/1 year) | ||
| "You feel happy, you see the success of the system (…), you see that the wheel turns in society" (I/physician/38 years/3 years) | ||
| [8,0]Relationship with donor and recipient families comforting donor families getting the donation acknowledgements | "The experiences lived with dozens of families, which in each of the donation processes teaches you about first-rate human values, along with the second chances of the transplant recipients who in their own words "are re-born"" (Q/physician/51 years/20 years) | |
| "Basically at the time when the families accept and agree to the donation. Mainly when the family after the donation thanks you for the work and are satisfied despite the grief" (Q/physician/43 years/2.5 years) | ||
| "When a family, despite the death of a loved one, is capable of saying goodbye and thanking you" (Q/physician/59 years/22 years) | ||
| "Meeting with the donors' families again and seeing the transplanted patients" (Q/nurse/43 years/UK/NR) | ||
| "After a family agrees to the donation in the interview and the initial care of the transplant patients" (Q/physician/47 years/UK/NR) | ||
| "Sometimes I have a relationship with some transplant patients and they spread their excitement to me for the new chance at life" (Q/nurse/56 years/25 years) | ||
| "…that the donor's family ends up thanking you, that after they are the one who are generous and the heroes, they go giving thanks" (I/nurse/40 years/1 year) | ||
| "It leaves the best taste in my mouth, being able to accompany the family, being with them (…). I'm still perplexed, after the entire process, they thank you (…). I think that it may be like a little stick to cling to, giving meaning (to their loss)" (I/nurse/62 years/27 years) | ||
| "(The donor's mother) came close to me and hugged me and said: thank you very much, that, for the rest of my life (…), something that can't be described, something that you'll carry with you for all your life (…) she made me feel like I had never felt in my life" (I/ex-coordinator/physician/50 years/10 years) | ||
| [30,0]Most difficult aspects | [4,0]Communicating the death | "Communicating the fatal outcome of the potential donor and the logical emotional reaction to the bad news received" (Q/physician/56 years/6 years) |
| "Sharing the times of crisis and grief of the families who just received the worst news" (Q/physician/51 years/20 years) | ||
| "When the family is informed about the death of their family member, if it was sudden and they do not understand…" (Q/nurse/56 years/25 years) | ||
| "The time when the brain death is definitively reported and preparing the ground for a subsequent organ donation petition" (Q/physician/56 years/UK/NR) | ||
| "The most emotional burden is, without a doubt, communicating the death and the interview to request the donation. In some cases it is communicating the death that is the hardest moment, in others requesting the organs is more emotional because it is when the family expresses their fears, doubts, and pain. You see the delivery or you suffer the frustration from a no that you have to try to reverse" (Q/physician/46 years/9 years) | ||
| [17,0]Donation interview. Paediatric, young, or unknown donors. Projection of similar experiences or personal situations. Grief | "Informing and interviewing the family the day of the death and thus requesting the donation" (Q/physician/47 years/UK/NR) | |
| "The telephone call when they alert you about the possibility of a donor and the time of the interview with the family, before talking about the possibility of donation" (Q/physician/49 years/UK/NR) | ||
| "At the exact moment that the family says yes to the donation and begins to cry" (Q/physician/43 years/2.5 years) | ||
| "(after communicating the death to them)… after I have to go and ask for their organs and sometimes it's hard because I feel their pain" (Q/nurse/56 years/25 years) | ||
| "The family interviews that we do with parents when a child dies" (Q/nurse/43 years/UK/NR) | ||
| "A child with syncope who died with no apparent reason…" (I/nurse/44 years/1 year) | ||
| "When it involves children, even babies, you see such a small child, so defenceless, such a defenceless family (…), then I do a comparison with my personal life, I identify myself when I see that child, that family…" (I/physician/38 years/3 years) | ||
| "The donation interview with a mother, whose 4-year-old child drowned in the pool" (Q/physician/56 years/6 years) | ||
| "One case that impacted me was a young donor, the interview with his widow who had two small daughters" (Q/physician/49 years/UK/NR) | ||
| "A young girl who after a discussion with her husband had a subarachnoid haemorrhage (SAH) and died a few hours later, with two small children, with a complicated family situation" (Q/physician/46 years/9 years) | ||
| "The interview that I did with the parents of my daughter's friend" (Q/nurse/43 years/UK/NR) | ||
| "The death of a 14-year-old boy in the hospital facility, who came from playing football like my son" (Q/nurse/56 years/25 years) | ||
| "Each donation involves an emotional impact, perhaps more in young donors in type 3 asystole" (Q/physician/43 years/2.5 years) | ||
| "Requesting an organ donation from young donors and explaining to their parents, on one occasion spending more than 4 hours trying to get the mother to accept that her 19-year-old son had died" (Q/physician/59 years/22 years) | ||
| "Child donors are a psychological hell and young people. (…) And another very stressful situation was when I entered the room and, with the family, I saw a friend of mine, who knew the deceased… and I broke down" (I/physician/34 years/1.5 years) | ||
| "Perhaps talking with the mother of the boy who died, since I'm a mother, you put yourself in her place…" (I/nurse/46 years/0.2 years) | ||
| "The girl who had died was the age of my daughter…" (I/physician/50 years/10 years) | ||
| "I have had the complicated grief of a father who came every Wednesday, sat there, and asked me: "Where are my son's organs?"…" (I/nurse/62 years/27 years) | ||
| [7,0]Organisational difficulties and professional relationships | "I believe the most difficult involves having to confront certain obstacles and problems that my work colleagues always bring up, at the time of arranging the donation" (Q/physician/46 years/9 years) | |
| "The incomprehension of certain colleagues" (Q/physician/59 years/22 years) | ||
| "The personnel tend to be very egocentric, it is "me, me, me" and they try to manipulate you with lots of scientific criteria and "no, don't sweet-talk me, no"… how distasteful most people are, and me too, I don't say I'm not, we are motivated by our interests" (I/nurse/47 years/18 years) | ||
| "…(I left coordination) because there was no agreement with my management team at any given time, it was clear" (I/ex-coordinator/physician/50 years/10 years) | ||
| "Those who have left up to now, because they do not get along with their more-or-less immediate supervisors, do not share the same criteria, and because we are a group that has to coordinate with sometimes 300 people (…), you have to know how to get along with 3 or 4 department heads, who may come to have different interests" (I/nurse/47 years/18 years) | ||
| "That we should be a team, I do not believe we have that, the members have be completely together, be accomplices, row on the same boat, however, I don't see that" (I/nurse/40 years/1 year) | ||
| "The hospital is how it is, thousands of people work there, each one from their father and their mother… difficulties, millions… that you have to solve alone at 2 or 3 in the morning…" (I/nurse/40 years/1 year) | ||
| "The work of a coordinator, especially at small hospitals, sometimes makes you feel very alone, fighting against all the annoyances that arise in the health system, which are a lot… It causes more stress than dealing with the donor's family" (Q/physician/46 years/9 years) |
The identification of the verbatim quotes is given in parentheses in the format: technique (Q: questionnaire; I: interview/professional category/age/experience in coordination).
Circumstances of high emotional intensity have been reported given the variability in the reactions of family members, against which the professionals develop adaptive, judgement-free, and often, improvised, styles of approaching them.
For me, it is always novel and each interview is an outpouring of emotions (Q/physician/56 years/UK/NR).
You open the door and you don't know what you will find, you don't know how you can introduce it, or how to ask it. There are those who will tell you how you have to do it (I/nurse/40 years, 1 year of experience).
…I understand any reaction from any family, I understand everything, I don't judge anything. I will treat you the same if you were King Felipe VI or someone from the district of Los Pajaritos (…), it doesn't have anything to do with your social, cultural, or economic status. That is what coordination taught me… (ex-coordinator/physician/50 year/10 years).
One strategy widely used, applied consciously and maturely among the people with more experience and nearly spontaneously among those with less experience, is to listen, giving the families time to express their emotions, request the needed information, and have all their questions answered. The focus on listening and active communication corresponds to one of the basic objectives of the donation interview, which is to accompany, help, and support families in grief, beyond the purpose of procuring organs.
I have reached the point of doing interviews almost without speaking… you only have to say that you are the transplant coordinator and listen to them and help them, and you will be surprised, when did I ask for the donation? I didn't ask for it, but they tell me yes (Ex-coordinator, physician/50 years/10 years).
Many times I have stayed silent and it was the family who directed me to what has to be done, many times… (I/physician/34 years/1.5 years).
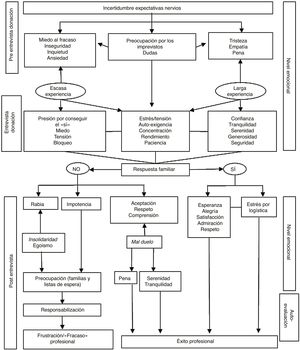
Fig. 1 presents the reported emotional experiences, observing how the clearly differentiated moments of before, during, and after the interview imprint shared emotional experiences, but also different ones, depending on the years of experience and family response to the donation.
Before the interview, feelings of apprehension, uncertainty, and nervousness are common, which results in doubts and concerns about the family response and possible unexpected events.
(I feel) a little bit of anxiety, including a feeling of uncertainty, apprehension about what will happen, what to say to the family, how they will reaction (…) Sorrow for the family, because of their loss, anticipation of getting close to them and the outcome, of trying to help the family and get the donation, not putting my foot in my mouth… (Q/physician/46 years/9 years).
I feel respect to see what I will encounter and lots of uncertainty; each interview is different and there is always something that you have not confronted and don't know how to resolve, uncertainty always 100 percent (I/physician/34 years/1.5 years).
There are times of tension, uncertainty, anxiety, worry, sometimes doubts. Waiting for the reactions of the families and how they will take our interventions makes me very nervous, sometimes somewhat afraid (Q/physician/56 years/6 years).
Those who have less experience report anxiety and worry related to fear of failure, while in those with long experience empathy with the families, sadness, and sorry for their loss predominate.
I'm afraid, afraid of not doing it well, making the family feel good, afraid, afraid (I/nurse/46 years/0.2 years).
Fear… fear of not knowing how to manage the situation, not having the right tools, of failing at something, expressing yourself poorly, not presenting the request in the right way (I/nurse/44 years/1 year).
I never stop "having butterflies in my stomach". (I feel) nervousness, sadness, empathy (Q/nurse/56 years/25 years).
With time I feel calmer, but many years have passed and it still ends up affecting me emotionally. (I feel) sadness, especially before the interview (Q/physician/59 years/22 years).
During the interview, all the health care personnel experiences situations of intense stress, tension, and concentration.
It is a feeling of alertness, open to all circumstances, operating at full power, peak capacity, with all five senses at 100%, a stressful situation… (I/nurse/40 years/1 year).
The stress is focused from different perspectives: recently hired individuals report sensations of fear and a mental block and high pressure to obtain agreement for the donation.
(When I started) to confront the family I was very afraid, I was very pressured to get a yes to the donation (…). I was very overwhelmed that they would say no, so I was very tense and very nervous and the situation overcame me, and I sometimes blanked when the family asked questions that I didn't know how to answer… (I/nurse/47 years/18 years).
My whole body trembled, I became nervous, very worried… (I/nurse/40 years/1 year).
Once they gain experience, the tension experienced during the interview is experienced as confidence and professional calm, with a central element being the usefulness of the interview, not just for obtaining organs, but also for accompanying the family and relieving the family's grief.
I feel good, since I approach the interview as an opportunity to help and accompany a family who is going through a very bad time (Q/physician/51 years/20 years).
In general, rather calm and tranquil, because I provide them with the opportunity to help other people and I help them to fulfil their desire to donate (Q/nurse/56 years/25 years).
Once the interview is over, there are two determining factors for the emotional experiences of the coordination personnel: first, the "yes" or "no" from the families and how this response is interpreted by the health care personnel; and second, the self-evaluation process that culminates with the sensation of professional success or failure.
Sensation of success or failure…, that is, evaluating your work, do you explain things clearly enough… whether it is a clear "no" or a "yes", but you evaluate it (I/nurse/44 years/1 year).
When they say "no" to the donation, it is considered a sign of a lack of solidarity and egotism, the health care professionals report feelings or anger and helplessness and intensely feel concern for the patients who are waiting for a transplant, as well as for the families themselves and their grief. Attributing responsibility to themselves is very high in this professional group, and often, the emotional outcome is frustration and a feeling of professional failure.
When you are inexperienced (…) you take the negative response as a loss (…) I felt angry (I/ex-coordinator/physician/50 years/10 years).
(I feel) helpless for not being able to help the families with an act which is only sustained by positive values (Q/physician/51 years/20 years).
Most (negative responses) are due to a lack of solidarity. When a family (…), which surely if their child needed a transplant (…), if they would receive it, but now they won't give? … that is egotism. (…) You know that a "no" means that people on the waiting list will die (…), so that weighs on us regarding possible negative responses. I suppose the term "professional failure" also weighs on you (…) partly you always think "I did it poorly and that's why they told me no"… sometimes partly because of the worry for those who are on the waiting list, partly because of worry that "I did it poorly", but especially, psychologically, "how does the family feel?" (I/physician/50 years/10 years).
On the other hand, when the professionals accept the donation rejection as a consequence of "bad grief", they experience this situation from a position of acceptance, respect, and understanding, and even though they feel sorry, they remain calm and tranquil. In addition, they make the experience a positive one based on the usefulness of the interview for accompanying and supporting the family, and they therefore experience a sensation of professional success.
Denying consent for donation will always exist and the people who refuse to donate are not bad (…) accepting them is the first step, respecting them is the best that a transplant coordinator can do and take into account that the family who refuses the donation does not have mechanisms to start a positive grieving process (I/ex-coordinator/physician/50 years/10 years).
I want them to be well informed about everything and all their fears resolved… Because of this I do not have negative feelings about the family members (I/nurse/47 years/18 years).
The emotions experience of a "yes" to donation also has different pathways, although they trigger a unanimous sensation of professional and personal success. Happiness and satisfaction for the positive interview outcome, hope for the possibility of saving other patients, as well as admiration and respect for the donor families predominate. However, the feeling of stress about organising the transplant process also reactivates.
The proactivity of that family in favour of donation had a larger emotional repercussion on me (…), the generosity of people moves me more emotionally than egotism (…), I'm worn out but I feel good (I/physician/50 years/10 years).
(I feel) hope that the patient's death will be the start of a new opportunity (Q/physician/51 years/20 years).
(I feel) happy knowing that these decisions help a lot and surprised by things that we sometimes do not expect in these situations. Then total tranquillity and calmness (Q/physician/56 years/6 years).
(I feel) satisfaction at the time they say "yes" (Q/physician/43 years/2.5 years).
After the interview, if it is positive, a feeling of stress starts because of all the calls that I have to start making (Q/physician/49 years/UK/NR).
Regarding expressing emotions or crying, different patterns by sex appear, with emotional closeness and emotional expression being more common among women, also understood as elements of professional and personal quality.
I learned to hug (…) and to cry with the donors and I don't feel like less of a doctor because of this, but like a much better doctor. Doctors have been seen as poor professionals for showing emotions or letting themselves cry (…), because of being men and because of being doctors (…) (ex-coordinator/physician/50 years/10 years).
On the other hand, some men emphasise the risk of expressing emotion for efficiency and obtaining objectives, although there are also opinions which emphasise the intensity of the emotions experienced, the difficulty managing such emotions, and the feeling of vulnerability and defencelessness they experience due to the lack of resources and support and the rigidity of the system.
Up to a certain point we are empathetic with the family, but also objective about what we do. Because at that point we cannot share the emotions at the family level, because then we would not be doing our job (…), we would end up not being efficient. A little like soldiers, right? (I/physician/38 years/3 years).
Letting our emotions out is making our vulnerability and fragility clear… And we are the ones who grit our teeth (…). And then, who will take care of us? (I/physician/50 years/10 years).
It is presumed that we are superheroes, that we have teeth made of steel and that we can chew through everything, that we are strong (…). Theoretically, we are 90%… but with what side effects? That doesn't matter… It is a very pragmatic and utilitarian viewpoint from the coordination structure… (I/nurse/62 years/27 years). "Lots of wishful thinking, if not, it's impossible". Coping strategies and proposals for improvement
With emotional intensity, it is expressed the lack of formal resources and skills and personal and self-taught coping: 1. Individual and internal strategies: emotional neutralisation and negation, making the experiences positive. 2. Group strategies: emotional expression by sharing among equals and seeking family support, physical or leisure activities (Table 5).
Coping strategies and needs/proposals for improvement.
| Topic | Results | Verbatim quotes |
|---|---|---|
| [27,0]Coping strategies | [7,0]Relaxation, self-management, denial, isolation, waiting | "I try to relax, I breathe deeply, I concentrate and breathe deeply" (Q/nurse/56 years/25 years) |
| "The emotional burden is difficult to avoid. Day by day I try to make sure what happened doesn't get to me" (Q/physician/56 years/6 years) | ||
| "Talking about them, even though I try to forget what I experienced and leave what happens in the hospital" (Q/physician/47 years/UK/NR) | ||
| "Putting up a shield and doing my coordinator work, for better or worse, but I do my job (…) For as much as people want to help you, no one reaches the same place, the same thought, for as much as you tell them about it, no one has experienced it, and even though my colleague can experience it, they live it differently than me, so no one thinks or feels what you do, so no one can help you 100% and that's it, let time pass and return" (I/physician/34 years/1.5 years) | ||
| "I've had to do it alone, developing defence mechanisms to not bring it home" (I/nurse/47 year/18 years) | ||
| "When I suffer, I don't do anything to cure myself, but I wait until it passes. (…) And it's not brushed off, it builds up little by little" (I/nurse/40 years/1 year) | ||
| "You take your emotions home with you, but we also have resources to say "this was a completely unfair and inexplicable tragedy", but when you get home, what you do is put up a barrier and be normal, (if not) it would be unfair for your family and for you. (…) And I would consider myself a little cold, in the sense that I'm closed off" (I/physician/38 years/3 years) | ||
| "The way to not focus on emotions is to rise up to the intellectual world, so we intellectualise things, much easier to put a name, last name, label, classify, and so on, than to get it out" (I/physician/50 years/10 years) | ||
| [6,0]Making it positive: Thinking about positive outcomes. Giving meaning to the loss and comforting the family members of donors. Saving the life of organ recipients | "You learn to manage your feelings, "It’s not my fault that they died", "the studies say that what I'm going to do brings them something positive", ""how could I be so bad as to not give them that option?"" (I/nurse/44 years/1 year) | |
| "The family of donors who are destroyed, when the donation finishes, they are usually calm, comforted by having donated, the more organs you tell them that were donated, the more content they are. I've discovered that by being really sincere and opening up your heart, they resolve their questions and they become content and I don't feel anything negative" (I/nurse/47 years/18 years) | ||
| "If the family knows that their child continues living through another child, to some extent, the grief and the loss, although still suffering, that helps them to getting out of the pit of grief a little bit easier" (I/physician/38 years/3 years) | ||
| "If I was not there, this family would be suffering alone" (I/physician/38 years/3 years) | ||
| "Remembering that it is all for a good reason" (Q/physician/46 years/9 years) | ||
| "Thinking that you have to keep moving forward and thinking about the positive, about the donation outcome, about the people who have improved their quality of life" (Q/physician/59 years/22 years) | ||
| "I'm practical and I don't like to get off the boat without having found something positive. And I get it in the family and in the final objective which is the transplant patients…" (I/nurse/40 years/1 year) | ||
| [3,0]Communication/sharing with equals | "I try to talk about it with other colleagues, sometimes it helps me to get it out, with people who understand you" (Q/physician/46 years/9 years) | |
| "You find support from the rest of the coordinators, it is very important" (I/physician/55 years/7 years) | ||
| "For me, the recognition of my colleagues" (I/ex-coordinator/physician/50 years/10 years) | ||
| "We contact each other because we know that the other understands us. (…) it is hard (for them to understand you) outside the group and what we do is unusual outside the group, we tend to do it amongst ourselves or we do not do it…" (I/physician/50 years/10 years) | ||
| [8,0]Leisure, sports, and family support | "Going out for a walk, soaking up some sun, spending time with family, doing sports" (Q/physician/51 years/20 years) | |
| "I try to go out to the country if I can, walking. Other times I just want to be quiet at home, because a donation leaves you physically and mentally exhausted" (Q/nurse/56 years/25 years) | ||
| "You will run, you will drink a beer or play paddle tennis, you put on a film, you play music, or you work… and you carry on" (I/physician/50 years/10 years) | ||
| "Thinking about my family who are well and I have the opportunity to be with them and enjoy more of my live" (Q/physician/43 years/2.5 years) | ||
| "I try to distract myself, enjoy being with friends, laugh, my family helps me avoid the bad moments" (Q/physician/46 years/9 years) | ||
| "Having the next day off and being with my children" (Q/physician/56 years/UK/NR) | ||
| "I have a lot of support from my wife, my kids (…) they have always supported me" (I/physician/55 years/7 years) | ||
| "Music is essential in my life (…) and then I have the recognition in my house (my son and my husband), both are very proud of me" (I/ex-coordinator/physician/50 years/10 years) | ||
| "I would not have endured this if my wife had not supported me, because this robs you of time with your family, your private life" (I/nurse/62 years/27 years) | ||
| [18,0]Needs, demands, and proposals for emotional management and training | [10,0]Training and therapy/group sessions for emotional self-management and anticipation | "Maybe training actions and group sessions to share could help to resolve the emotions that we feel during the donation interview" (Q/physician/56 years/UK/NR) |
| "Especially training actions that help you to face an interview properly" (Q/physician/43 years/2.5 years) | ||
| "I believe that a mixture of an improvement in training, both in managing emotions themselves as well as managing the environment, conflict situations, would help and it would perhaps be interesting to schedule periodic psychological evaluation sessions or meetings with other coordinators for that, for sharing and group therapy" (Q/physician/46 years/9 years) | ||
| "Group sharing sessions for experiences, activities to share experiences" (Q/physician/56 years/6 years) | ||
| "Shared training sessions with personnel who usually work in this setting" (Q/physician/47 years/UK/NR) | ||
| "Trying to explain the experiences is much easier with someone who has lived and gone through the same as us" (I/nurse/44 years/1 year) | ||
| "(The strategy of) sharing experiences seems very good to me (…) perhaps I do see that, meetings at the National Transplant Organisation or wherever, discussing experiences… And then communication courses…" (I/ex-coordinator/physician/50 years/10 years) | ||
| "Sharing inspires, how other people have managed a problem… and then conferences, studies, also help" (I/nurse/44 years/1 year) | ||
| "We have done one course on bad news in our entire career as coordinator, so, zero training. And I go home with baggage daily, that I say at some point will overflow…" (I/physician/34 years/1.5 years) | ||
| "Recounting the experiences we each have too, you can learn a lot, the diversity helps" (I/nurse/47 years/17 years) | ||
| "I would have needed someone to explain to me… "don't worry if that happens", because I went in with nothing and no one explained anything to me. (…) I would have been nice if my superior (…) would have dedicated time to teaching me, looking at me and saying "you are going to face this, and be careful with this and that", as I think I have taught and tried to have my colleagues do so" (I/ex-coordinator/physician/50 years/10 years) | ||
| [7,0]Coaching/continuous and cyclical psychological help | "Coaching sessions for emotional management" (Q/physician/49 years/UK/NR) | |
| "I don't believe any of them would be miraculous. Although I'm inclined towards coaching and deepening my emotional intelligence" (Q/physician/51 years/20 years) | ||
| "There will be people who are not trained in ethics or simply the emotional burden is too big for them to be able to assimilate it, for those coaching or psychological help can do good" (Q/physician/43 years/2.5 years) | ||
| "Courses and a psychologist… yes, there's nothing, despite being transplant pioneers in Spain, but no, no psychological support, not for the family or for us. Because of that, a psychologist, but not personal, for the group (…) The essential is psychological support and coaching sessions (…), someone who re-educates me on what I should do and what I am not doing, something every x time and continuous, since courses are forgotten…" (I/physician/34 years/1.5 years) | ||
| "The targeted (strategies), coaching, everyone has their own way of facing their emotions, and not all are equal…" (I/nurse/46 years/0.2 years) | ||
| "Coaching or psychotherapy… because at times you need something more specific or individual for you (…) and from an external perspective, an audit that is not self-audited, by a competent person, in this case, like a psychologist…" (I/nurse/44 years/1 year) | ||
| "There would be a big lack of psychological support or coaching… I don't like being told how I have to do things, but rather to have several paths, in transplant coordination there has to be various resources to reach from here to there, this is the path and it has to be done the easiest way each time, if the coaching sessions are like that…" (I/nurse/47 years/18 years) | ||
| "Survival tools for the coordinator, that is, "this will happen like this, and that will affect you like that"…" (I/nurse/62 years/27 years) |
The identification of the verbatim quotes is given in parentheses in the format: technique (Q: questionnaire; I: interview/professional category/age/experience in coordination).
The main needs, demands, and proposals for improvement reveal the importance of training for managing emotions and refer to training activities, directed group therapy, psychological support, and coaching (Table 5).
DiscussionThis study shows the emotional complexity and intensity of transplant coordination work and reveals the variability in the emotional experiences surrounding the donation interview, highlighting as conditional factors professional experience and the interpretation of family reactions. Similarly, it collects the needs and demands for training and support for emotional training and management expressed by the coordination teams.
The study has a series of limitations. The first is related to the qualitative design, which does not allow the results to be extrapolated, although methodological similarities with other available studies are in favour of a comparative focus. The second refers to the sample selection, where mediation by key informants may have biased the selection and information, although it also facilitated access to professionals with little time and availability. The combination of interviews and questionnaires may have generated results with different degrees of depth. However, doing it this way gave the entire study population the opportunity to participate and made it possible to delve into their experiences, to analyse their experiences in context. The usefulness and application of the qualitative methodology in the study on the donation and transplant processes has valuable precedents in the national context.12
When describing the coordination work, the high professional responsibility assumed around diverse duties—clinical, treatment, relational, organisational, communication and social campaigns, leadership, or management10,13,20—show the complexity,6 emotional intensity,6,7,21 and impact of this professional activity on the ontological perspective, lifestyles, professional identity,9,13,22 or the physical and mental health of the health care professionals themselves.8,14,23,24
The dichotomy that combines challenge and opportunity, satisfaction and stress, pride and effort, comfort and fatigue coincides with the ambivalent "fascinating and exhausting" experience reported by transplant coordinators in the USA8 and verifies the apparently contradictory coexistence between the positive experience and large difficulties of the coordination work encountered in the literature.4,7
In our study, the gratifying experience is essentially based on the orientation towards the outcomes10,25 and the quality of the relationship with patients and family members,8,10,13 but it also highlights the professional context of excellence and development opportunities, as well as the benefits of working in multidisciplinary teams, in which discrimination by professional category are minimised and the recognition of knowledge is prioritised. In this sense, the organisational model of intra-hospital coordination is highly valued, although some criticism has arisen towards professional attitudes and resistance or the requirements and rigidity of the organisation system.
Among the most difficult aspects, the donation interview appears as the moment of the most emotional complexity and intensity, an issue which in the literature is shown to have high stress and drama,22,26 fatigue, and emotional shock.14,27 Like in other previous research, the emotional experiences related to the interview are full of nervousness, uncertainty, and apprehension,11 which create a background of concentration and stress.9
The contribution of our study refers to how the emotional routines diverge depending on professional experience: fear and pressure8,9,13 are very intense among recently joined individuals, while those who are more experienced channel the stress through confidence and serenity. Transitioning from the first path to the second occurs, according to the discussions with professionals, over time and based on internal and self-conducted processes, since institutional support or formal resources are few or non-existent. This result is confirmed based on the reported coping strategies, which are often individual, leisure, and sports,26 avoidance or denial7, making the experience positive,8,10,25 confirming the sensation of professional "solitude" and "isolation"8 (p. 12), although a generalised agreement on the benefits of cohesion, collaboration, and group interventions does appear.28
In this sense, among the practical application of the results, we highlight the need and explicit demands for therapy and group support for professionals, with special attention to those who were recently hired, more exposed to the impact of the stress and at risk of abandoning transplant coordination. The training to provide resources, strategies, and emotional management and communication skills has already demonstrated its effectiveness in the transplant field14,22,29 and for retaining quality health care personnel.30
Another relevant topic in the emotional paths of coordination teams arises at the end of the donation interview, with the "yes" or "no" from the family, how this response was interpreted, and the professional self-evaluation. For a "yes", the emotional path tends to be uniform, with predominately positive emotions which reflect the unequivocal sensation of satisfaction and professional success.10,11,13
For a "no", the professionals who adopt a relational-emotional model with the families emphasise the benefits of the interview for listening5,31 and accompanying the grief and search for meaning because of the loss,8,9,32 experiencing compassion and sensitivity.32 This result was confirmed in our study, through the bad grief-acceptance/respect-pity/tranquillity-professional success pathway.
When the donation interview approach prioritises the clinical aspects and efficiency in procuring organs,9,32 a "no" from the families generates exhaustion and emotional burnout among the coordination teams,14 results which in our study are reflected in the non-solidarity/egotism-anger/helplessness-worry-responsibility-frustration/professional failure emotional path.
Another controversial aspect related to the difficult emotional experiences is emotional expression. In our study, the debate was organised around the meaning of a "good" professional: the women advocate the benefits of expressing emotion, important when seeking balance between negative and positive emotions,8 for overcoming difficult situations and strengthening empathy and trust with the families.27,33 The men mostly associate expressing emotions with a loss of a professional image,34 although some identify the costs of this emotional camouflage, in the same vein as the risk to psychological health, it brings to mind the metaphor of "hiding behind a mask" expressed by some Australian professionals6 (p. 705).
ConclusionsBased on these results, there is a clear need to prioritise a strategy for the mental and emotional health of transplant coordinators, by implementing emotional evaluation and care plans, aimed at improving training for optimal emotional management in stressful situations that put health at risk.
FundingThis study has received no specific funding from public, private or non-profit organisations.
Conflict of interestNone.
We want to thank all the study participants for their time, dedication, and commitment.
Please cite this article as: Danet AD, Cardoso PMJ, Villares JMP. Rutas emocionales en las experiencias profesionales de losequipos de coordinación de trasplantes. Nefrologia. 2020;40:75–90.