Liver failure is a severe condition with a high mortality rate resulting from the loss of the liver's capacity for detoxification of endogenous substances (ammonium, bilirubin, glutamine, lactate), regulation and synthesis function (coagulation factors, albumin).1,2 The consequences are coagulation disorders, circulatory dysfunction, encephalopathy, and multi-organ failure including kidney failure.2 Treatment of liver failure depends on its cause and reversibility. Liver transplantation is an effective treatment in fulminant failure or progression of chronic liver disease, while in transient situations (viral infections, poisoning) there may be regeneration of the liver parenchyma and functional recovery.1,2 In these situations (awaiting transplantation or functional improvement), supportive therapies aimed at clearing liver toxins may become necessary, to which dialysis may be added to counteract the accompanying kidney failure.2 For the treatment of acute liver failure there are five artificial systems in use: molecular adsorbent recirculation system (MARS); single-pass albumin dialysis; fractionated plasma separation and adsorption (Prometheus); selective plasma filtration therapy; and haemodiafiltration.2–5 Single-pass albumin dialysis was described as an alternative to sophisticated devices (MARS) in the late 1990s. It is the simplest artificial liver device and can be applied in any unit where a standard dialysis monitor is available. No additional adsorbent columns or circuits are required. The patient's blood is dialysed through a high-flux dialyser using an albumin-containing dialysis fluid. After passing through the dialyser, the dialysate is discarded (in contrast to MARS, where albumin dialysate is regenerated), and toxins are thus removed from the system. Considerable amounts of albumin are used, making this treatment potentially costly.4 We describe here a case of liver failure associated with acute renal failure, in which extended online haemodiafiltration associated with single-pass albumin dialysis was performed.
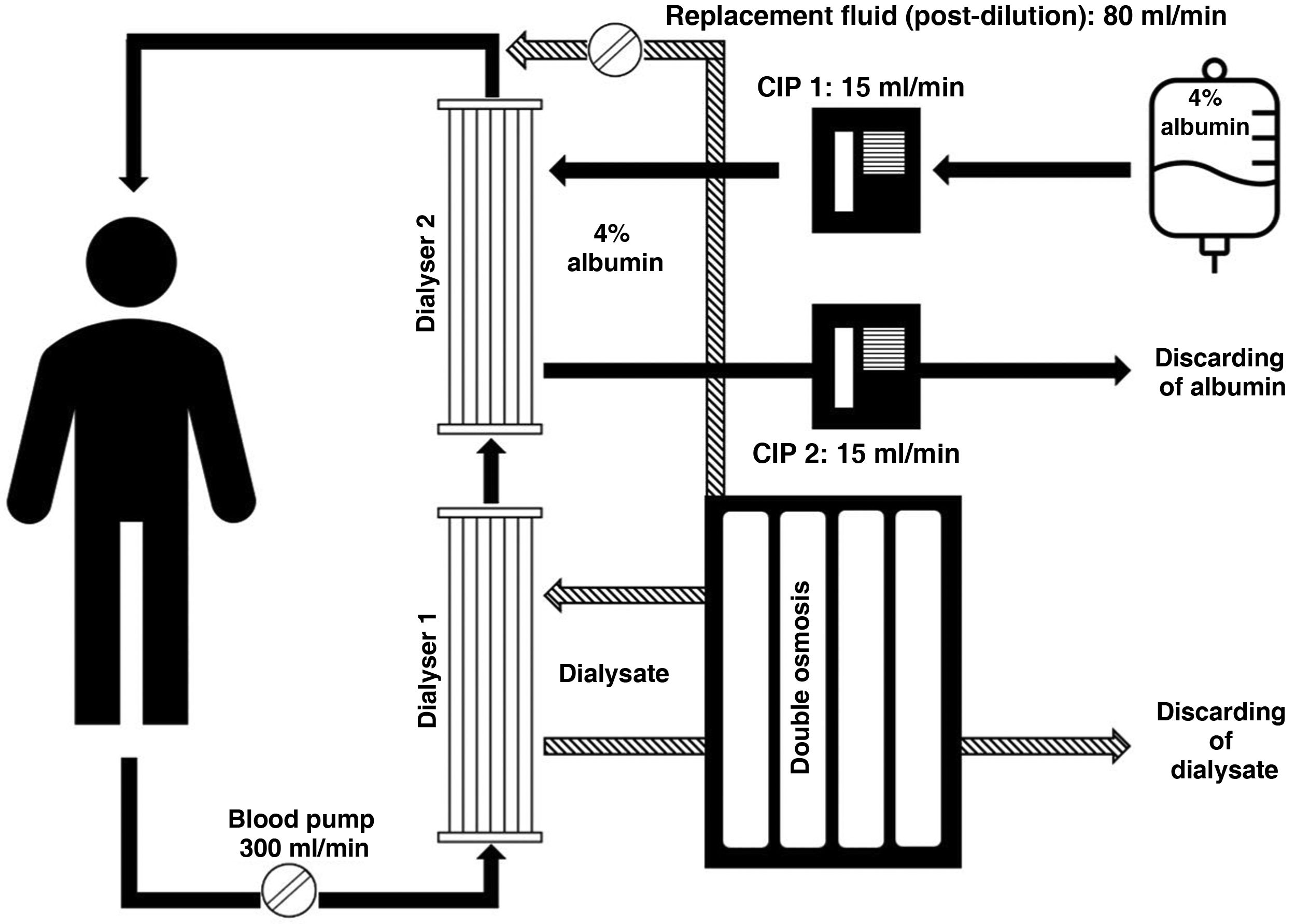
The patient was a 39-year-old woman diagnosed with adenocarcinoma of the colon with liver metastases in the left lobe. Reversed chemotherapy with adjuvant criteria was chosen as a therapeutic strategy, producing a good response with a reduction in the volume of the primitive tumour and liver metastases, for which reason a coordinated left hepatectomy was performed. At 48h, the patient showed a progressive increase in bilirubin and transaminases, associated with a severe decrease in prothrombin time and lactic acidosis (Table 1). Clinically she had marked jaundice, hepatic encephalopathy and sustained haemodynamic deterioration with shock. In this context, she also developed anuric acute kidney injury (KDIGO 3). In view of the patient’s acute liver failure and anuric acute kidney injury, renal replacement therapy with extended online haemodiafiltration (8h) was opted for, combined with dialysis with single-pass albumin (treatment of acute liver failure). Haemodiafiltration provides an additional contribution to the clearance of water-soluble residues associated with liver failure. For the procedure we used a Fresenius-4008H® monitor, Fresenius-Acqua1C®multipass osmosis, Fresenius-FX80® high-flux dialysers (2), continuous infusion pump (2) to generate circulation of the albumin bath, and 4% albumin bath at an estimated volume of 15ml/min/procedure. The structure of the assembled device is shown schematically in Fig. 1. The procedure was well tolerated, and vasopressor support with noradrenaline was maintained during the procedure with the addition of terlipressin. The values of the different biomarkers before and after the procedure are shown in Table 1. Unfortunately the patient died some hours later, with subsequent histopathology showing a pattern of diffuse hepatitis with extensive distortion of the liver parenchyma, which was attributed to probable cytotoxicity due to previous chemotherapy.
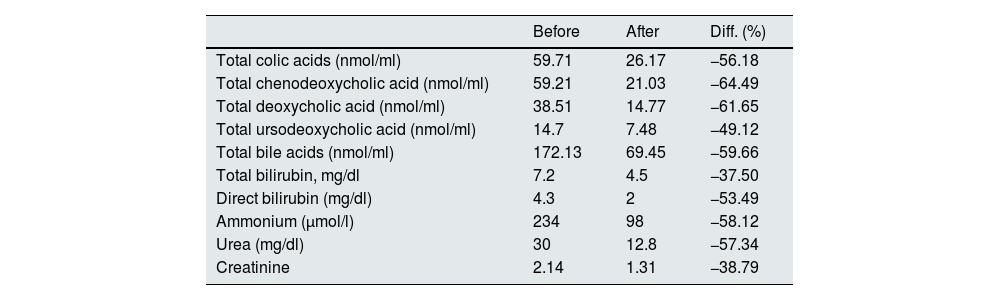
Pre- and post-procedure plasma values.
| Before | After | Diff. (%) | |
|---|---|---|---|
| Total colic acids (nmol/ml) | 59.71 | 26.17 | −56.18 |
| Total chenodeoxycholic acid (nmol/ml) | 59.21 | 21.03 | −64.49 |
| Total deoxycholic acid (nmol/ml) | 38.51 | 14.77 | −61.65 |
| Total ursodeoxycholic acid (nmol/ml) | 14.7 | 7.48 | −49.12 |
| Total bile acids (nmol/ml) | 172.13 | 69.45 | −59.66 |
| Total bilirubin, mg/dl | 7.2 | 4.5 | −37.50 |
| Direct bilirubin (mg/dl) | 4.3 | 2 | −53.49 |
| Ammonium (μmol/l) | 234 | 98 | −58.12 |
| Urea (mg/dl) | 30 | 12.8 | −57.34 |
| Creatinine | 2.14 | 1.31 | −38.79 |
Diff (%): percentage difference.
We present here our experience in the use of extended online haemodiafiltration associated with single-pass albumin dialysis. It proved to be a well-tolerated and efficient procedure for the removal of water-soluble substances (urea, ammonium) by haemodiafiltration, and removal of hydrophobic substances (bilirubin, bile acids) by albumin dialysis. It costs significantly less than MARS or Prometheus liver support systems, does not require additional training of human resources, and can provide liver support and associated renal replacement with outcomes comparable to other technologies. Unlike other systems, it does discard the used albumin (single step),3 which is the most costly step of the procedure in financial terms. The practicality of mounting the device, the accessibility of the different circuit components (common connectors, high-flow fibres) and dialysates (haemodialysis bath and 4% albumin) make this procedure a suitable and feasible alternative for the supportive treatment of hepatorenal failure.
Conflicts of interestThe authors have no conflicts of interest to declare.