Hepatitis B is an important agent of liver disease in patients with chronic kidney disease and chronic HBV infection promotes the development of CKD in the adult general population. Patients with CKD have a suboptimal response to various vaccines, and it remains unclear how we boost the immune response of CKD patients to HB vaccine.
Study aims and designWe performed a narrative review to assess the mechanisms of lower immunogenicity of HBV vaccine in CKD population; multiple approaches to improve the response rate of CKD patients to HBV vaccine have been reported. This is a very important topic for nephrologists who often serve as primary case providers for patients with CKD.
ResultsThe recommended vaccine schedule for CKD patients including those on maintenance dialysis is based on recombinant vaccine, four doses (month 0,1,2, and 6; 40mcg each) by intramuscular route (deltoid muscle). According to RCTs or observational studies, some recombinant vaccines with adjuvants (i.e., HBV-AS02 and HBV-AS04) look promising. HBV-AS04 showed to give better seroprotection rates and durable immune response over extended follow-ups compared with licensed HBV vaccine in CKD patients. The seroprotection rate was 95% (97/102) and 82% (202/248) in pre-dialysis and dialysis patients, respectively, one month after completing vaccine schedule with HBV-AS04. HBV-AS02 was superior to licensed vaccine in terms of seroprotection rate, 76.9% vs. 37.6%.
ConclusionsWe suggest adjuvanted recombinant (HBV-AS04) vaccine (0,1,2 and 3 months; 20 mcg each dose) and post vaccination testing of anti-HBs antibody after vaccination. Booster doses to patients whose anti-HBs titers fall below the seroprotection level (<10IU/mL) during the follow-up are appropriate. The patho-physiologic mechanisms responsible for the poor immunogenicity of HBV vaccine in CKD patients are under active investigation.
La hepatitis B es un importante agente de la enfermedad hepática en pacientes con nefropatía crónica (NC) y la infección crónica por el virus de la hepatitis B (VHB), promueve el desarrollo de la NC en la población general adulta. Los pacientes con NC tienen una respuesta subóptima a varias vacunas, y no está claro cómo podemos aumentar la respuesta inmunológica de estos pacientes a la vacuna contra el VHB.
Objetivos y diseño del estudioRealizamos una revisión narrativa para evaluar los mecanismos de menor inmunogenicidad de la vacuna contra el VHB en la población con NC; se han documentado varios enfoques para mejorar la tasa de respuesta de los pacientes con NC a la vacuna contra el VHB. Este es un tema muy importante para los nefrólogos, que a menudo atienden como médicos de atención primaria a pacientes con NC.
ResultadosEl programa de vacunación recomendado para los pacientes con NC, incluidos los que están en diálisis de mantenimiento, se basa en una vacuna recombinante de cuatro dosis (meses 0, 1, 2 y 6; 40 mcg cada dosis), administrada por vía intramuscular (músculo deltoides). Según los ECA, o estudios observacionales, algunas vacunas recombinantes con adyuvantes (es decir, HBV-AS02 y HBV-AS04) parecen prometedoras. La HBV-AS04 demostró ofrecer mejores tasas de seroprotección y una respuesta inmunitaria duradera durante los seguimientos prolongados, en comparación con la vacuna autorizada contra el VHB en pacientes con NC. La tasa de seroprotección fue del 95% (97/102) y del 82% (202/248), en pacientes en prediálisis y diálisis, respectivamente, un mes después de completar el programa de vacunación con HBV-AS04. La HBV-AS02 fue superior a la vacuna autorizada con respecto a la tasa de seroprotección, 76,9 vs. a 37,6%.
ConclusionesSugerimos una vacuna recombinante con adyuvante (HBV-AS04) (meses 0, 1, 2 y 3, 20 mcg cada dosis) y pruebas de anticuerpos anti-HB después de la vacunación. Se consideran adecuadas las dosis de refuerzo para los pacientes cuyos títulos de anticuerpos anti-HB sean inferiores al nivel de seroprotección (< 10 UI/mL) durante el seguimiento. Los mecanismos fisiopatológicos responsables de una inmunogenicidad deficiente de la vacuna contra el VHB en pacientes con NC son objeto de investigaciones exhaustivas.
Patients with CKD on maintenance dialysis have reduced survival compared with those having intact kidneys; cardiovascular diseases, infections, and neoplastic disorders are the leading causes of morbidity and mortality in CKD population, including those treated by dialysis or transplantation.1
The incidence of infections and infection-related hospitalizations has been reported to increase as kidney function declines even if the risk remains poorly characterized by individual stages of CKD. High rates of infections among patients with end-stage renal disease and earlier stages of CKD have been related to the immune compromise conferred from uremia. In addition, advanced age, co-morbidities such as diabetes, and high rates of hospital admissions play a role.2
Active immunization is an important piece of the preventive management for patients with CKD, as has been pointed out in the past and recently.3–4 It is well known that vaccination rates are suboptimal in patients with CKD; in fact, individuals with advanced chronic kidney disease and/or treated with immunosuppressive agents have lower rates of seroconversion, lower antibody titers, and a less sustained response over time in comparison with non-uremic individuals.3 The Advisory Committee on Immunization Practices (ACIP) and the American Academy of Pediatrics (AAP) have given special emphasis on hepatitis B, influenza, and pneumococcal immunization in CKD patients and routinely recommend these vaccines for ESRD population.5 Previous studies and recent outbreaks within dialysis units of developed countries suggest low compliance to these recommendations, particularly among non-caucasian individuals.6 This is a very important topic for nephrologists who frequently serve as primary case providers for their patients with CKD.
The largest body of evidence regarding vaccines in CKD patients mostly regards hepatitis B virus vaccine in dialysis population. In fact, hepatitis B virus has been an important concern within dialysis units of industrialized countries in the 1960s and 70s; the frequency of HBV is currently low but not negligible among patients undergoing dialysis in the industrialized world.7 In addition, recent data has been accumulated showing that chronic HBV infection promotes the development of CKD in the adult general population.8
The aim of this study is to review the most important evidence concerning HBV vaccine in the CKD population. We have highlighted the recent advances which have been made in the field.
Epidemiology of hepatitis B virus in CKDHepatitis B virus (HBV) is an important agent of liver disease including cirrhosis, hepatocellular carcinoma, and hepatic failure. According to World Health Organization, 257 million people were living with chronic hepatitis B virus infection (HBsAg positive) in 2015. Hepatitis B resulted in an estimated 887,000 deaths in 2015, mostly from cirrhosis and hepatocellular carcinoma. WHO calculated that 27 million people (around 10% of all people estimated to be living with hepatitis B) were aware of their infection in 2016. Hepatitis B can be prevented by vaccines that are safe, available, and effective.9
The spread of HBV infection has significantly lowered over the recent decades and the control of spread of HBV within dialysis units of developed world has been a milestone in the management of ESRD. The implementation of routine screening of blood derived products, and infection control practices including universal precautions, separation of rooms and machines for HBsAg positive patients, monthly serological testing for HBsAg of all susceptible patients (and prompt review of the results) have sharply lowered the incidence of HBV infection in dialysis units even if outbreaks continue to occur in HD units.10
The prevalence of HBV infection is now low within dialysis units from these countries (chronic HBsAg seropositive status ranging from 0% to 10% in patients on regular dialysis).10 The epidemiology of HBV among dialysis patients in the less-developed world is not well known. The evidence gathered to date is mostly based on single-center surveys, with rates of chronic HBsAg carriers ranging between 2% and 20%.10 The greater frequencies of HBV infection within dialysis units from developing countries can be attributed to several factors such as a higher prevalence of HBV in the respective general population and an incomplete implementation of infection control strategies against HBV. A lack of financial resources could in part explain the low compliance to infection prevention measures within dialysis units from less-developed world.
Additional factors which helped the control of HBV infection among patients on maintenance haemodialysis likely were lower blood transfusion requirements due to increased erythropoietin use, and vaccination. Although consistent progress has been made, haemodialysis patients remain at increased risk of HBV acquisition due to persistent exposure to blood products, uremic immunodeficiency and sharing of haemodialysis equipment.10
The low immunogenicity of HBV vaccines in CKD: the aetiologiesPatients with advanced CKD show a decreased response to vaccination mostly concerning thymo-dependent antigens (i.e., hepatitis B, diphtheria, or tetanus) while the immune response to thymo-independent antigens (i.e., pneumococcal disease) appears normal. A defect in the relationship between B and T lymphocytes rather than intrinsic B lymphocyte has been emphasized. There is solid evidence in the medical literature reporting that patients on maintenance dialysis who receive a full course of recombinant (i.e., Engerix-B) HBV vaccine (four doses at 0,1,2, and 6 months, 20 mcg each dose by intramuscular route) show a seroprotection rate around 50–60%. In addition, the anti-HBs antibody levels are low and fall logarithmically with time.3
Numerous clinical, demographic and biochemical parameters have been advocated to explain the poor immunogenicity of HB vaccines in advanced CKD such as age,11 gender,12 overweight,13 positive serologic status for HCV,14 and human immunodeficiency virus infection,15 blood transfusion history,16 interleukin genotypes,17 possession of the major histocompatibility complex haplotype HLA-B8, SCOI, DR3,18 and inappropriate nutritional status.19–20 According to a single-center report, vitamin D deficiency has been linked with poor response to HB vaccine (n=3 doses, 40 mcg recombinant HB vaccine) in CKD stages 3-5D.21 The failure to complete the full course of HBV vaccine plays also a role.22 A recent survey assessed vaccination coverage among fee-for-service (FFS) Medicare beneficiaries with ESRD who received dialysis at any point from 2006 through 2015 in the US.23 A total of 350,000 ESRD dialysis beneficiaries who began dialysis over the 10-year study window were identified. 68% of patients received at least one administration of the vaccine during the study window (2006–2015). However, only 89,589 (25%) completed the four-dose series and about 11% of individuals received serologic testing within 60 days following fourth dose. The investigators also adopted a more restrictive definition (i.e., completing the series according to the ACIP-recommended dosing schedule); only 33,032 (9%) patients completed the four –dose series.23
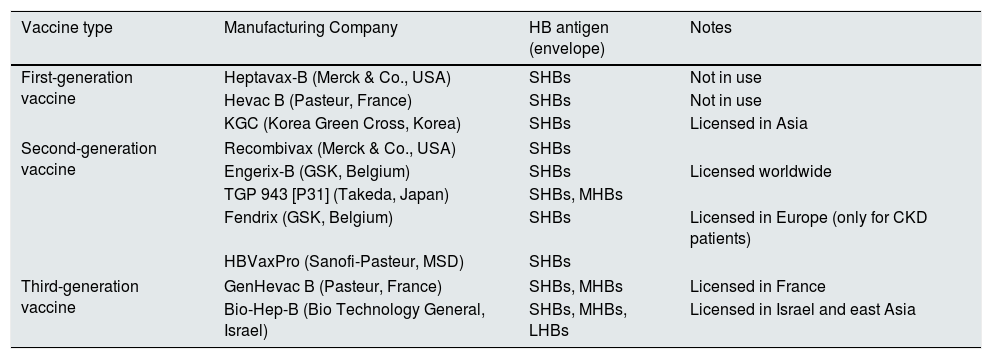
HB virus vaccine in patients and CKD: historical perspectiveFirst generation vaccine was developed from plasma of HBsAg carriers in the late 1970s in France and the US (Table 1). HBsAg was extracted by plasma-exchange from HBsAg carriers and then inactivated by heat or chemically. Good evidence reported that it was safe and effective.24 During the 1980s, three large, placebo-controlled, double-blind, randomized trials were published showing the efficacy and safety of plasma-derived vaccine in patients on maintenance haemodialysis.25
Hepatitis B virus vaccines.
| Vaccine type | Manufacturing Company | HB antigen (envelope) | Notes |
|---|---|---|---|
| First-generation vaccine | Heptavax-B (Merck & Co., USA) | SHBs | Not in use |
| Hevac B (Pasteur, France) | SHBs | Not in use | |
| KGC (Korea Green Cross, Korea) | SHBs | Licensed in Asia | |
| Second-generation vaccine | Recombivax (Merck & Co., USA) | SHBs | |
| Engerix-B (GSK, Belgium) | SHBs | Licensed worldwide | |
| TGP 943 [P31] (Takeda, Japan) | SHBs, MHBs | ||
| Fendrix (GSK, Belgium) | SHBs | Licensed in Europe (only for CKD patients) | |
| HBVaxPro (Sanofi-Pasteur, MSD) | SHBs | ||
| Third-generation vaccine | GenHevac B (Pasteur, France) | SHBs, MHBs | Licensed in France |
| Bio-Hep-B (Bio Technology General, Israel) | SHBs, MHBs, LHBs | Licensed in Israel and east Asia | |
Nephrologists had been reluctant to offer plasma-derived vaccine to their patients because of the (unjustified) concern over transmission of the HIV virus by vaccine. HBV vaccines replaced the plasma-derived vaccines – they were made by recombinant DNA technology (1980s). Recombinant technology gave the possibility to express HBsAg in prokaryotic as well as eukaryotic cells such as yeast cells, Saccharomyces cerevisiae. Yeast cells are transfected with HBV DNA sequences which coded for SHBs (small hepatitis B virus surface protein). Genetically engineered yeast-derived vaccines have been commercially available since 1986; Jilg et al.26 were the first authors to publish their experience on HBV vaccine made by recombinant DNA technology
No RCTs have been published on this point and the evidence in the medical literature is mostly made by a great number of single center surveys that have been published during the following two decades. Second-generation vaccines are currently adopted for universal vaccination of newborns and adults in >170 countries all over the world.
A new generation of recombinant HBV vaccine has been then developed in some countries (third-generation vaccines)- these are recombinant HBV vaccines expressed in mammalian cells and containing additional envelope proteins (Pre-S1 and Pre-S2). Third generation vaccines have been licensed in some countries only- this could explain why the evidence in the scientific literature is so limited.27–29
The low immunogenicity of HBV vaccines in CKD: the answersVarious approaches have been suggested to improve the immunogenicity of the HB vaccine in uremia such as administration of vaccines at pre-dialysis stage,30 intradermal route of vaccination,31 supplementary vaccine doses,32 double vaccine doses,33–34 and concomitant administration of immune modulators including oral levamisole,35–36 thymopentin,37–38 granulocyte macrophage colony-stimulating factor (GM-CSF),39–40 recombinant gamma (γ-IFN)41 or alpha (α-IFN) interferon,42 zinc supplementation,43 interleukin-2,44 and erythropoietin (EPO).45
Vaccination of haemodialysis patients with a combined hepatitis A and hepatitis B regimen may be more effective than hepatitis B monovalent vaccine in providing seroprotection. However, vaccination against HAV in dialysis patients is not routinely performed because it is neither associated with HD therapy nor transmitted through parenteral mechanisms.46
The low immunogenicity of HBV vaccines in CKD: PMMA membraneThe thymo-dependent humoral response is abnormal in uremia and a lack of contact between CD40 and CD40L has been considered to play a pivotal role in the impairment in B lymphocyte immune response of these patients. CD40 activation by CD40 ligand (CD40L) promotes an important signal in B lymphocytes during primary response.47,48
Preliminary studies have shown greater levels of soluble CD40 (CD40s) in advanced CKD, CD40s is the extracellular part of the CD40 product and is released by the metalloprotease TACE (ADAM17) which plays a proteolytic activity on the CD40s’ membrane. CD40s is a natural inhibitor of the CD40/CD40L interaction. It has been mentioned a great increase of CD40s in uremia and this could, at least in part, explain the poor response to HB vaccine in the HD population.47
15 patients on maintenance dialysis who were not responders to recombinant HB vaccine underwent HD therapy for 40 weeks with PMMA dialysis membranes; 60% of them developed seroprotection after a second course of HB vaccine.49 Similar findings have been obtained by another group.50 Furthermore, HD sessions with PMMA membranes gave a 30% reduction of CD40s levels (post-dialysis versus pre-dialysis levels); such a phenomenon did not occur with other membranes.51
The EPADIAL study, a multicentric RCT from France included patients on maintenance HD on polysulfone (n=11) or PMMA (n=14) for 40 weeks. According to a intention-to-treat analysis, there was no difference with regard to the seroprotection rate between the two groups, 50% vs. 54.5% (week 40) (NS). Of 20 patients with available data, the median CD40s titer at week 12 in non responders was lower than that observed in responder patients, 193 vs. 413pg/mL (P=0.08). The investigators concluded that there was not a better vaccine response with the PMMA membrane in comparison with high-flux polysulfone. Dialysis with a PMMA membrane did not restore the abnormal immune response to the HBV vaccine.52
The low immunogenicity of HBV vaccines in CKD: the adjuvantsAttempts to overcome the impaired immune response in patients on maintenance dialysis have produced mixed results. Adjuvants are thought to improve immune response by various mechanisms as an example improving antigen presentation to T cells. Aluminum salts have been widely adopted for more than 70 years and oil in water emulsion is commercially available for influenza vaccines. AS04 is another adjuvant (combination adjuvant) that has been approved for human papilloma virus and HBV.
In November 2017, FDA approved Heplisav-B (Dynavax Technologies Corporation, US), a hepatitis B vaccine that combined hepatitis B surface antigen with Toll-like receptor 9 agonist adjuvant (TLR) to enhance the immune response in adults. Heplisav B is the first new hepatitis B vaccine in the United States in more than 25 years and the only two-dose hepatitis B vaccine for adults. The evidence about Heplisav B in the CKD population is limited. According to a multicenter RCT (n=467 patients with CKD), the percentage of patients with anti-HBs antibody titers>100mIU/mL in the HBsAg-1018 arm was significantly greater than that observed in the Engerix arm (74% vs. 32%).53,54
HBV-AS02 is an adjuvanted HBV vaccine where recombinant HBsAg is formulated with AS02. AS02 is an oil-water emulsion-based adjuvant system consisting of MPL and QS21, a highly purified immunostimulant extracted from the bark of the South American Quillaja saponaria tree. HBV-AS02 does not contain any aluminum salt- its efficacy and safety has been assessed in two multi-center, open, randomized comparative trials. In study A, a group of patients with CKD (pre-dialysis, peritoneal dialysis and haemodialysis) received HBV-AS02 (n=125) or a licensed conventional recombinant HB vaccine (HBVaxPRO) (n=126). These patients had failed to respond to prior vaccination with a conventional HB vaccine. In study B, a large group (n=181) of CKD patients who failed to maintain protective antibody concentrations after prior HB vaccination was included. In study A, HBV-AS02 was superior to conventional recombinant HB vaccine in terms of seroprotection rate (76.9% vs. 37.6%) and anti-HBs mean geometric antibody concentration (GMC, 139.3 vs. 6.9mIU/mL). In study B, rates of seroprotection one month after administration of the booster dose was 89% and 90.8% in the HB-AS02 and in the licensed vaccine group, respectively. The frequency of individuals with anti-HBs titer≥100mIU/mL was greater in the HB-AS02 group than in the licensed vaccine group, 81.3% vs. 60.9% respectively. Anti-HBs geometric mean antibody concentration were more than 9-fold higher in the HB-AS02 group than in the licensed vaccine group, one month after booster administration.55
The same group of investigators evaluated the persistence of immune response up to 36 months after primary vaccination in an open, international, Phase III follow-up study in a cohort of (n=151) pre-dialysis, peritoneal dialysis and haemodialysis patients>15 years of age. At month 36, 89.5% of subjects in the HB-AS02 group and 72.6% of those in the HB-AS04 had seroprotection. Anti-HBs geometric mean antibody concentrations were greater in the HB-AS02 group over the 36 months of follow-up. The authors concluded that HBV-AS02 vaccine potentially reduces the need for booster doses as it induces high and persistent anti-HBs antibody levels.56
HBV-AS04 vaccine in CKD populationA recombinant HB vaccine adjuvanted by a novel system (AS04) has been commercialized (2005) in Europe for patients with kidney impairment aged over 15 years; each 0.5mL dose of the HBV-AS04 vaccine contained AS04 [50 mcg MPL adsorbed on aluminum salt (500 mcg Al3+)] and 20 mcg recombinant HBsAg. 3-0-desacyl-4′-monophosphoryl-lipid A (MPL) is adsorbed on aluminum phosphate and synthesized in Saccharomyces cerevisiae by DNA recombinant techniques. MPL stimulates the immune system and acts through binding on the Toll-like receptor 4 on antigen-presenting cells. MPL-stimulated antigen-presenting cells produce good levels of co-stimulatory molecules (including CD86 molecules) and cytokines and provide consistent cellular and humoral activities.
The registration trial of HBV-AS04 in CKD population was an open, randomized clinical trial conducted in pre-HD (creatinine clearance≤30mL/min) and HD patients, over 15 years of age and naïve for HB. A large cohort (n=165) of patients was enrolled, HBV-AS04 (four single doses) was compared to Engerix (four double doses) administered at 0,1,2, and 6 months, and followed-up for 36 months. After the vaccine course, seroprotection rates were 91% versus 84% in the HBV-AS04 and standard vaccine groups (NS). At month 36, a seroprotection rate of 72.9% was noted in the HBV-AS04 versus 52% in the conventional vaccine group (P=0.03).57
A few years later, Kong and colleagues reported the results of the follow-up study evaluating antibody persistence and anamnestic response and safety of HBV-AS04 booster doses up to 42 months after the initial vaccine course. Antibody persistence was greater in the HBV-AS04 than in the standard HBV vaccine group (78.4% vs. 51.4%, P=0.023).58
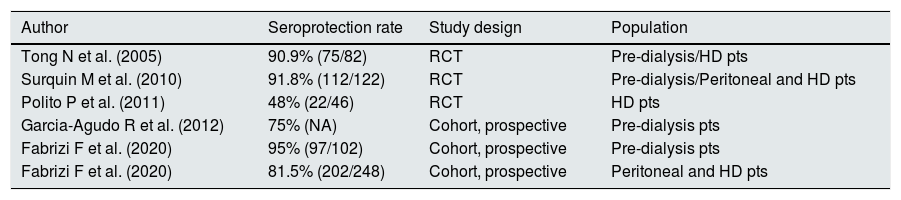
The efficacy and safety of recombinant adjuvanted HBV vaccine (HBV-AS04) has been explored in additional RCTs and observational studies (Table 2).59–62 The conclusion is that HBV-AS04 provides greater immunogenicity than conventional recombinant HB vaccines. What we need now is the evidence regarding the persistence of anti-HBs antibody after a primary vaccine course – we noted a sero-protection rate of 77% at month 72 but only a limited sample was available (n=7 patients).63 Studies provided with long follow-ups are hampered by the high drop-out rate typically observed in the CKD population (high mortality rate, renal transplant, transfer to another dialysis unit).
Adjuvanted recombinant HBV vaccine (HBV-AS04): evidence from medical literature.
| Author | Seroprotection rate | Study design | Population |
|---|---|---|---|
| Tong N et al. (2005) | 90.9% (75/82) | RCT | Pre-dialysis/HD pts |
| Surquin M et al. (2010) | 91.8% (112/122) | RCT | Pre-dialysis/Peritoneal and HD pts |
| Polito P et al. (2011) | 48% (22/46) | RCT | HD pts |
| Garcia-Agudo R et al. (2012) | 75% (NA) | Cohort, prospective | Pre-dialysis pts |
| Fabrizi F et al. (2020) | 95% (97/102) | Cohort, prospective | Pre-dialysis pts |
| Fabrizi F et al. (2020) | 81.5% (202/248) | Cohort, prospective | Peritoneal and HD pts |
The frequency of HBV infection among patients on maintenance dialysis in the developed world is currently low but not negligible and HBV vaccine is an important tool to prevent the spread of HBV in this clinical setting. It is well known that patients with chronic kidney disease have lower rates of seroprotection, and lower antibody titers after completing vaccine course; in addition, anti-HBs titers fall logarithmically over time. Numerous host factors have been retrieved which play a role in the reduced response to HBV vaccine in CKD. Various approaches have been tried to address this point; according to the evidence in the medical literature, we recommend adjuvanted HBV vaccine (HBV-AS04) (months, 0,1,2 and 3; 20 mcg each dose) and post vaccination testing of anti-HBs antibody after vaccination. Booster doses to patients whose anti-HBs titers are lower than 10IU/mL are appropriate. Studies are under way to develop vaccines provided with greater efficacy and satisfactory tolerability.
FundingThis paper was not funded.
Conflict of interestAll the authors have no relevant affiliations or financial involvement with any organization or entity with a financial interest in or financial conflict with the subject matter or materials discussed in the manuscript.