To the Editor:
Retroperitoneal fibrosis represents a diagnostic challenge due to the low frequency of presentation and the lack of specific symptoms. It is characterised by the presence of fibro-inflammatory tissue that surrounds the abdominal aorta and the iliac arteries1 extending to the retroperitoneal space and it covers neighbouring structures, such as ureters, causing obstructive uropathy (OU).
Although cases associated with multiple conditions (drugs, neoplasias, radiation and infection, amongst others) have been described, the most common cause is idiopathic.2
Idiopathic retroperitoneal fibrosis is more common in men aged 50-60 years old and, in most patients, it presents as non-specific lower back or abdominal pain.3
When the retroperitoneal tissue covers one or both ureters, potentially reversible obstructive renal failure occurs.1,2,4
We report the case of a patient with idiopathic retroperitoneal fibrosis that progressed to marked OU and an ultrasound showed slight unilateral dilation of the excretory system.
Our patient was a 54-year-old male, with no relevant personal or family history, referred by the General Practitioner due to incidental findings in the blood test of creatinine 2.74mg/dl. The patient had a history of three weeks of nausea, non-specific abdominal pain and slight testicular pain, with no other accompanying symptoms. Upon physical examination, he was normotensive and afebrile, with diuresis maintained, without macroscopic abnormalities, at around 2000ml/day.
In the blood test obtained from the Emergency department, the following parameters are notable: haemoglobin 15.3g/dl, leukocytes 6700/µl, platelets 305,000/µl, sodium 133mEq/l, potassium 3.6mEq/l, hepatic-pancreatic profile with no abnormalities, lactate hydrogenase 270U/l, plasma creatinine 3mg/dl, urea 116mg/dl. Urine biochemistry displayed values for sodium of 96mEq/l and potassium of 28mEq/l.
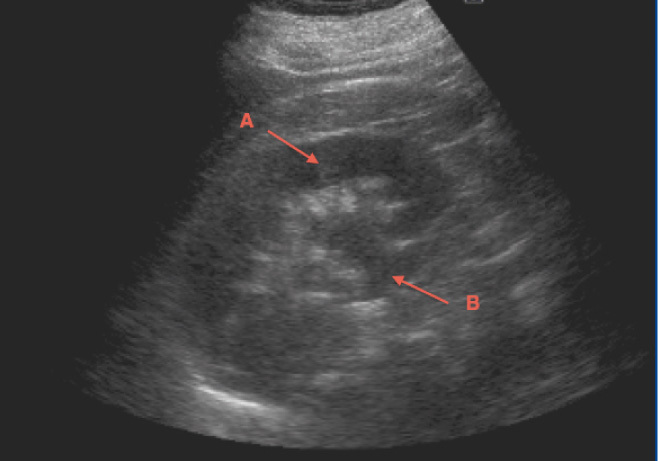
The renal ultrasound (Figure 1), showed normal-sized kidneys with cortical thickness maintained and we noted that the right side was larger and thicker. It showed slight dilatation of the right renal calyces (Figure 1) and no cause of dilation was seen with a bilateral positive ureteral jet on colour Doppler ultrasound.
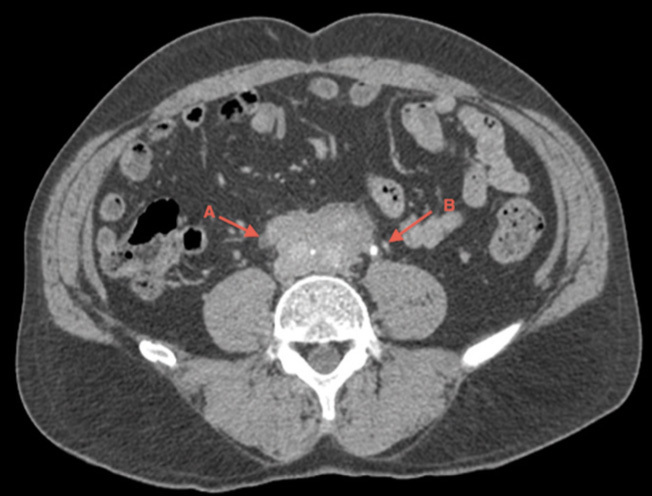
Given the poor test performance with progressive deterioration of renal function, a computerised tomography (CT) scan of the abdomen was carried out (Figure 2). It revealed a large retroperitoneal mass that covered the right ureter, with the left ureter free, but on the limit of the edge of the latter, resulting in bilateral OU, although it was more pronounced on the right side. The left side only showed incipient signs of obstruction.
After the diagnosis, he was treated empirically with high doses of prednisone and it was decided to use bilateral double-J catheters; following this treatment immediate improvement was noted. Five days later, the patient was asymptomatic and 30 days after starting steroid treatment, plasma creatinine was 1.02mg/dl. The double-J catheters were removed 6 months after the start of treatment, with stable plasma creatinine figures being maintained.
This case is of interest because, in spite of being an obstructive disease, ultrasound does not make clear the cause of obstruction, and on many occasions it fails to reveal the existence of the urinary tract obstruction itself. This is due to ureteral rigidity that conditions the disease itself, preventing dilation of the ureter covered by fibro-inflammatory mass.
In the case that we have presented, the patient displayed a significant impairment in renal function secondary to bilateral OU (right established and left incipient), with CT being required for its diagnosis.
Therefore, it is necessary to evaluate the need for other imaging techniques such as CT or MRI,5 in order to diagnose this entity, since treatment started at an early stage improves the clinical profile.
Conflicts of interest
The authors declare that they have no conflicts of interest related to the contents of this article.
Figure 1. Right kidney ultrasound
Figure 2. Computerised tomography