Pruritus associated with chronic kidney disease (Pa-CKD) is a disabling disease, very common in patients with advanced CKD (ACKD). With no clear diagnostic options, the therapeutic approach is inadequate and there is not a clear awareness of the clinical relevance among nephrologists. Our current perception is that presently the Pa-CKD is an unresolved chronic problem, with a significant impact on the quality of life (QoL) of our patients.
General characteristics of Pa-CKD: it is an unpleasant and particularly annoying sensation in hemodialysis (HD) patients, which makes the individual to scratch itself. Obviously, other dermatological or systemic causes of pruritus should be ruled out.1 Pa-CKD is chronic and persists for weeks. The urge to scratch can affect the whole body and is more intense in advanced stages of renal function impairment and in peritoneal dialysis (PD) or HD.2
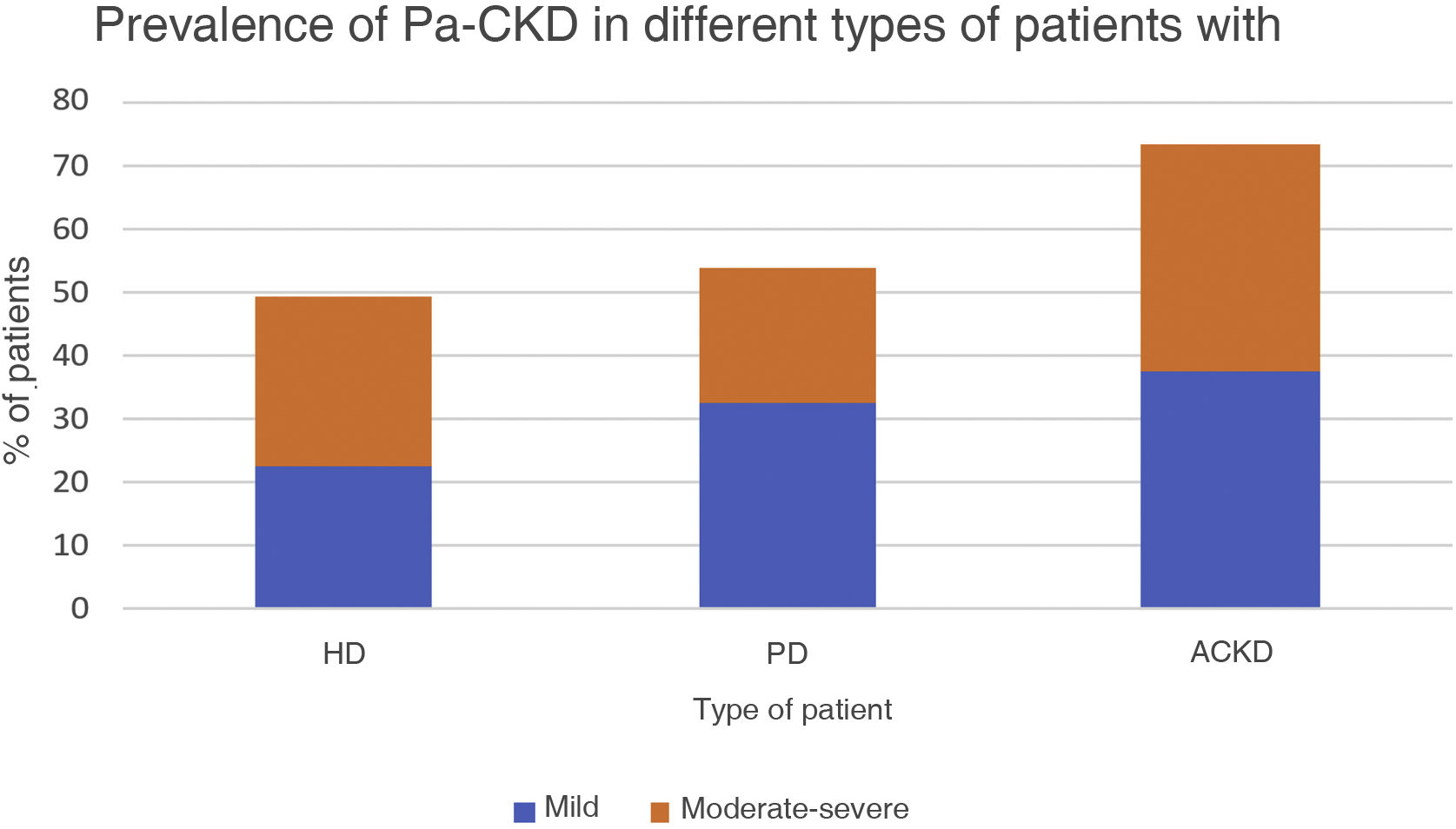
Prevalence of Pa-CKD in our setting: the results of a study to evaluate the prevalence of pruritus and its impact on QoL in the Spanish population with advanced CKD have recently been published.3 The study included 7 questions previously validated in pruritus assessment scales (presence, intensity, frequency, distribution, mood, sexual activity and sleep quality), distributed in collaboration with the Spanish Society of Nephrology (SEN). A total of 1605 patients answered these questions (mean 68 years, 92% on HD). The prevalence of Pa-CKD was 50.5% and, of these, 26.7% were from moderate to severe intensity. The prevalence was highest in non-dialyzed patients with advanced CKD (73.2% vs. 49.4% in HD, and 54.1% in PD) (Fig. 1).3 The conclusion of the study was that Pa-CKD in advanced CKD (dialyzed or non-dialyzed) is very prevalent in our setting and has negative consequences on QoL, including mood changes, depression, sexuality and sleep disorders. This is in agreement with other published pruritus studies, on the prevalence and impact on QoL, mood, sexual activity and sleep pattern alterations.2
Prevalence of Pa-CKD CKD.
ACKD, advanced chronic kidney disease; PD, peritoneal dialysis; HD, hemodialysis.
Adapted from Aresté et al.3
Pruritus has a subjective component, making this entity difficult to identify and diagnose. Very often, the patient does not refer it to the nephrologist.4 A recent qualitative study analyzed the reasons for underdiagnosis, highlighting the lack of knowledge of the association of pruritus with CKD, identifying it as something consubstantial an unavoidable.5 In general, the nephrologist’s attitude has not been very active. It has been considered difficult to manage, with no clear therapeutic options, and its prevalence has been underestimated, and has been associated mainly with hyperphosphoremia.6,7 At the health care level, the use of scales and Pa-CKD coding in the clinical history is not a common practice.4
The etiopathogenesis of Pa-CKD has not been totally elucidated. Among the mechanisms involved, there have been described alterations in the structure and function of the skin, as well as in the immune response and the chronic inflammatory state associated with uremia; alterations in the regulation of the endogenous opioid system and uremic neuropathy, and also accumulation of uremic toxins.8
Pruritus and quality of lifePa-CKD has clinical significance, it is associated with impaired QoL, including sleep impairment, interferes with social and work life,9 and it is a cause mood alterations (depression, frustration, embarrassment).1 Pa-CKD is an independent predictor of mortality,7,10,11 including cardiovascular mortality12 and long-term morbidities.13
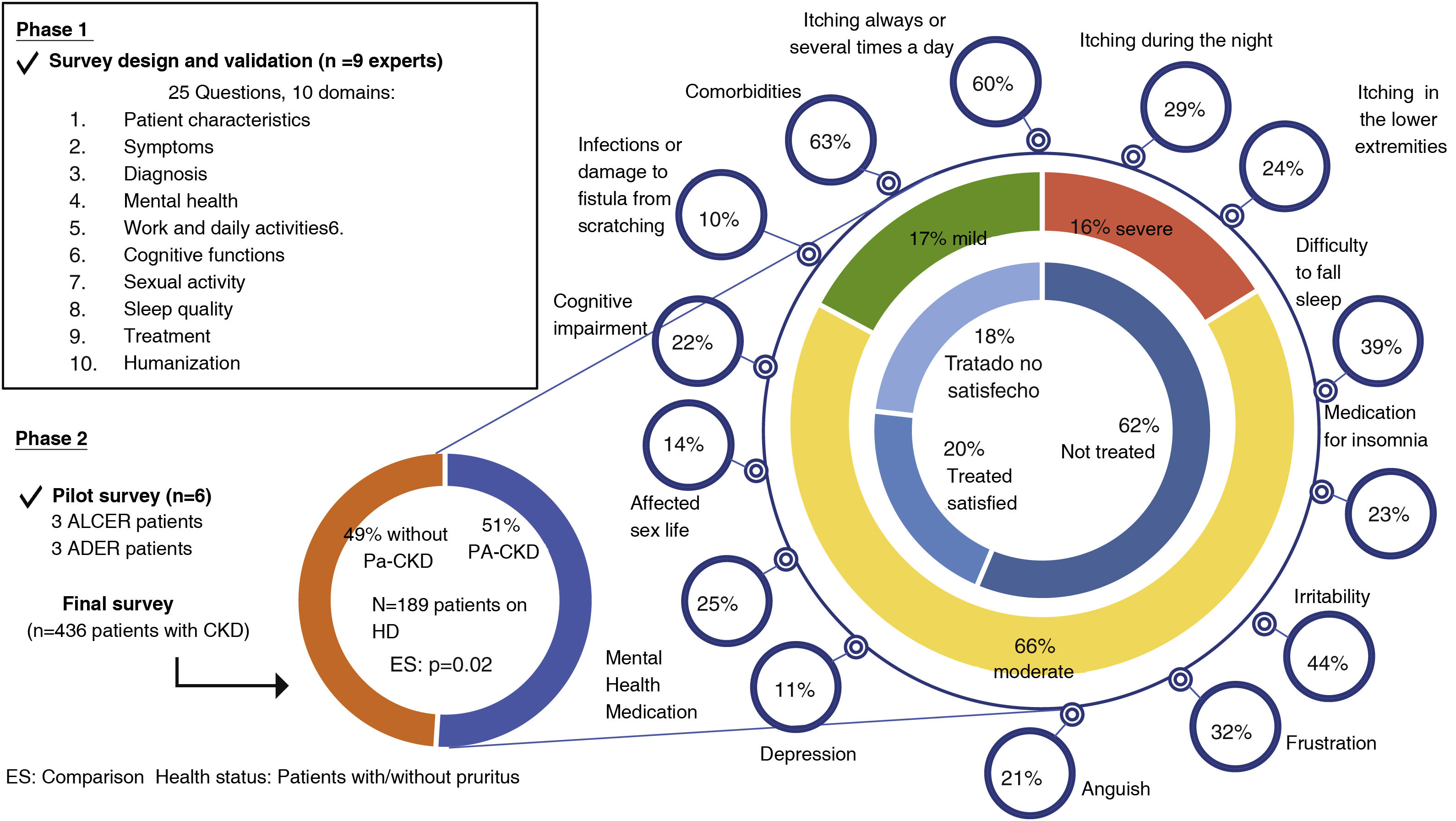
Survey on the impact of Pa-CKD on the quality of life of HD patientsDespite its clinical significance, in our setting few studies have shown the impact of Pa-CKD on QoL. A survey has recently been conducted in collaboration with the SEN and 2 patient organizations (Asociación para la Lucha Contra la Enfermedad Renal [ALCER] and Asociación de Enfermos de Riñón [ADER]) with the aim of analyzing how Pa-CKD affects QoL in people with kidney disease. Fig. 2 summarizes the methodology and results of the survey.
The design and validation of the survey was performed by a multidisciplinary group of 9 experts (2 representatives of ALCER patients, 1 representative of ADER; 1 expert in economics; 3 experts in quality of care and 2 nephrologists).
The essential scales used were: 5-D Itching scale,14 Skindex-10,15 Itching Severity Scale (ISS),16 Dermatology QoL index (DQLI),17 Kidney Disease Quality of Life Short Form (KDQOL-SFtm),18 EuroQoL-5D,19 Medical Outcomes Study Sleep Scale (MOS-Sleep)20 and Pittsburgh Sleep Quality Index (PSQI).21
The survey consisted of 25 questions divided into 10 domains, which together with the used variables are summarized in Fig. 2.
The survey included patients with CKD on HD with pruritus in the previous 3 months. It was estimated that 375 patients would be a representative sample (95% CI; 5% margin of error). A pilot survey was conducted with 3 ALCER patients and 3 ADER patients to identify possible barriers in the responses. The final version was sent to all members of the aforementioned associations and dialysis centers. Microsoft Office Excel v.365 was used for statistical analysis. Multiple responses were analyzed individually. Continuous variables were analyzed by calculating the means that compared by Student’s t-test.
The results showed that a total of 436 patients with CKD answered the survey. Of these, 189 (43%) were on HD, of whom 97 (51%) reported Pa-CKD (mean age 58 years, 68% male). Patients with Pa-CKD on HD reported significantly lower health status (HS) (46/100) than patients on HD without pruritus (53/100; p = 0.02). Moreover, HS worsened with increasing severity of pruritus (mild = 51/100; moderate = 48/100; severe = 32/100).
Of the 97 patients with Pa-CKD on HD, 63% reported comorbidities, including heart disease (28%), diabetes (20%) and hypertension (9%). Of these, 16% of patients reported severe, 66% moderate and 17% mild Pa-CKD. In reference to the total number of patients (189), this means that 42% of them had moderate to severe Pa-CKD. These data contrast with those mentioned above in which only 26.7% of patients with Pa-CKD experienced moderate to severe pruritus.3
In addition, 60% of patients reported pruritus always or several times a day and 32% several times a week, and its intensity was higher in patients who had it more frequently (always present or several times a day) compared to those who had it several times a week. Pruritus was more frequent throughout the day (30%) or at night (29%) than in the morning (2%). The most affected body areas were the lower and upper extremities (24% and 21%, respectively) and the back (23%).
The quality of sleep was affected by the pruritus and a 23% of patients received some treatment to facilitate sleep. Thirty-nine percent of patients reported difficulty falling asleep several times a week. In line with this, the DOPPS study reported that 30% of Pa-CKD patients with poor sleep quality were prescribed hypnotic medication to improve sleep quality.7
The negative effect of the Pa-CKD at the level of emotional burden and mental health was manifested in the form of irritability (44%), frustration (32%), anguish (21%) and depression (11%). Twenty-five percent were receiving hypnotic or anxiolytic pharmacological treatment (diazepam, lorazepam, bromazepam, alprazolam and hydroxyzine dichlorohydrate). This indicates that Pa-CKD increases the economic burden of the disease since a study carried out in Catalonia estimated that the average annual cost per case of depression treated was €1800, being 21.2% of the direct costs and 78.2% indirect (loss of productivity, days off work, etc.).22
A 22% of patients with pruritus reported impaired cognitive function attributed to pruritus, with lack of concentration or confusion. In addition, 10% of patients reported infections or damage to the fistula due to scratching.
According to Weiss et al.23 Pa-CKD limits patients’ social and daily activities. Likewise, 15% of the patients who responded to the survey commented that their ability to perform sports was limited; limitations were also reported in their ability to do housework (12%), their ability to eat out (11%), and in their ability to perform sex activity (14%). Only 15% of patients had been employed with salary during the previous 3 months, this is consistent with the DOPPS data, where 45% of patients found it difficult to work.9
In relation to the treatment received, 62% of the patients with pruritus had not received any treatment for pruritus and only 18% were satisfied with the treatment received (Fig. 2).
In Spain, the diagnosis of Pa-CKD was based on the direct communication from the patient to the healthcare personnel.4 The survey showed that 35% of patients do not report having pruritus for different reasons (not received attention or not being listened to, assumption that there was no a remedy, not awareness of the relationship with CKD or lack of opportunity). This correlates with the DOPPS data, which attributes it to symptom resilience, language problems, time available and awareness on the part of the nephrologist.9
Consensus documentThe Consensus Document for the diagnostic and therapeutic management of Pa-CKD in hemodialysis patients in Spain, written by nephrologists members of the Spanish group of Pruritus Associated with CKD and dermatologists members of the Spanish group of Research in Contact Dermatitis and Cutaneous Allergy (GEIDAC), has recently been published.24 This document has been endorsed and validated by the SEN to cover the current need for lack of specific guidelines for the differential diagnosis and management of Pa-CKD in Spain. The document focuses on screening, differential diagnosis and therapeutic alternatives, including a new drug, difelicefalin, currently not marketed in Spain, but available as an early use medication, which is the only existing drug indicated for the treatment of moderate to severe Pa-CKD in HD patients.
Key points in relation to the Pa-CKDPa-CKD is a very prevalent and disabling disease, with a great impact on the QoL of patients with CKD. In our setting, it is still an underestimated problem, underdiagnosed, without clear recommendations or guidelines and without adequate treatment.4
We propose 3 initiatives related to the clinical implications, diagnosis and treatment of Pa-CKD, which offer an opportunity to establish proactive attitudes in the management of Pa-CKD and thus favor the quality of life of these patients.
The first of these is the recent publication of the prevalence of Pa-CKD and its impact on QoL in patients with advanced CKD, carried out by the SEN,3,25 which indicates that it is a very prevalent problem and that up to 50% of patients on HD could be suffering from it.
The second, described in this article, is a proposal by the SEN, ALCER and ADER, aimed at investigating how Pa-CKD affects QoL in Spain, through a survey whose results have revealed the need for clinical guidelines and instructions for Pa-CKD.
The third is the publication of a consensus document by the SEN in collaboration with the GEIDAC, which presents an algorithm with guidelines aimed at facilitating diagnostic and therapeutic decisions for Pa-CKD to professionals involved in the care of people with CKD on HD.24
FinancingThe study reported was funded by CSL Vifor.
Conflict of interestPoS: lecture fees from Vifor Pharma, Amgen, Fresenius, Nipro, Astra Zeneca, Braun and Baxter; consulting fees from Astellas, Vifor Pharma, Baxter, Astra Zeneca.
JMB: fees for conferences, consultancies and travel vouchers for Vifor Pharma congresses.
JCJ: participation in advisory boards for the companies Astellas Pharma Europe Ltd., Astra Zeneca, Bristol-Myers Squibb, Boerhinger Ingelheim, Ipsen Pharma, GlasoSmithKline, Hansa Biopharma AB, Novartis Inc., Novartis Pharmaceuticals, Pfizer Ltd., and Travere Therapeutics.
The rest of the authors confirm that they have no conflict of interest.