Iron deficiency in congestive heart failure (CHF), with or without concomitant anaemia, is associated with health-related quality of life, NYHA functional class, and exercise capacity. Prospective, randomised studies have demonstrated that correcting iron deficiency improves the quality of life and functional status of patients with CHF, including those who do not have anaemia.
ObjectiveThe aim of this study was to analyse how frequently these iron parameters are tested and thus determine the extent to which this quality improvement tool has been implemented in patients admitted with CHF.
MethodsRetrospective observational study of patients from a university hospital diagnosed with CHF on admission between 01/01/2012 and 11/06/2013.
ResultsIron parameters were tested in 39% (324) of the 824 patients analysed. There was no significant difference in age between the patients whose iron was tested and those whose iron was not tested, but the difference in terms of gender was significant (p=0.007). Glomerular filtration rate and haemoglobin, were significantly lower in the group of patients whose iron was tested (p<0.001). The proportion of patients with anaemia, renal failure or both was significantly higher in the group of patients who had iron tests (p<0.001).
Of the 324 patients whose iron parameters were tested, 164 (51%) had iron deficiency. There were no differences between patients with and without iron deficiency in terms of age or gender. The iron parameters in both groups, ferritin and transferrin saturation index were significantly lower among the patients with iron deficiency (p<0.001). The glomerular filtration rate values were significantly lower in patients with no iron deficiency (p<0.001). Significant differences were also observed between those with and without iron deficiency in the proportion of patients with renal failure (79 vs. 66%, respectively, p=0.013), but not in terms of haemoglobin concentration.
ConclusionCongestive heart failure is very frequently associated with anaemia, iron deficiency and renal failure. Despite the fact that correcting iron deficiency is known to improve symptoms, testing of iron parameters in patients admitted with CHF is not performed as often as it should be.
La deficiencia de hierro en la insuficiencia cardiaca crónica (ICC), con o sin anaemia concomitante, se halla asociada a la calidad de vida relacionada con la salud, clase funcional NYHA, y a la capacidad de realización de ejercicio. Estudios prospectivos aleatorizados han demostrado que la corrección de la deficiencia de hierro mejora la calidad de vida y el estadio funcional de estos pacientes con ICC, incluidos aquellos que no presentaban anaemia.
ObjetivoEl objetivo de este estudio es analizar la frecuencia de determinaciones de estos parámetros de hierro y, por consiguiente, conocer la implementación de esta herramienta de mejoría de la calidad en pacientes que ingresan por ICC.
MétodosEstudio observacional retrospectivo sobre pacientes de un hospital universitario, que fueron diagnosticados al ingreso de ICC, entre el 1/1/2012 y el 11/6/2013.
ResultadosEl número de pacientes analizados fue de 824, de los que a un 39% (324) les fueron evaluados los parámetros de hierro. Entre los pacientes no evaluados y sí evaluados de hierro, no se observó diferencia significativa en la edad, aunque sí en el género, (p=0,007). Los valores del filtrado glomerular y de hemoglobina fueron significativamente inferiores en el grupo de pacientes analizados de hierro (p<0,001). La proporción de pacientes con anaemia, insuficiencia renal y de aquellos que presentaban conjuntamente ambas comorbilidades fue significativamente superior en el grupo de pacientes analizados de hierro (p<0,001).
Entre los 324 pacientes evaluados de parámetros férricos, 164 pacientes (51%) mostraban deficiencia de hierro. Entre los no deficientes y sí deficientes en hierro, no se observaron diferencias significativas en edad, ni en género. Los parámetros férricos de ambos grupos, ferritina e índice de saturación de la transferrina fueron significativamente inferiores entre los deficientes de hierro, (p<0,001). Los valores de filtrado glomerular fueron significativamente inferiores en aquellos que no mostraban deficiencia de hierro, (p<0,001). Se observaron igualmente diferencias significativas en la proporción de pacientes con insuficiencia renal, entre no deficientes y sí deficientes de hierro, (79 vs. 66%; p=0,013), aunque no en los valores de hemoglobina.
ConclusiónLa ICC se asocia con alta frecuencia a anaemia, deficiencia de hierro e insuficiencia renal. El estudio de los parámetros férricos en los pacientes que ingresan con ICC, pese a que la corrección de la deficiencia de hierro se asocia a mejoría de la sintomatología, no se realiza con la frecuencia necesaria.
Congestive heart failure (CHF) is associated with marked deterioration in health-related quality of life (HRQoL). Patients report symptoms such as dyspnoea during exercise, limited capacity for physical work, tiredness, susceptibility to develop stress and reduced mental and cognitive performance.1,2 Its prevalence is 1–2% in the general population, and may exceed 10% in individuals over 80 years of age.3
A common feature of CHF is iron deficiency, resulting from exhaustion of iron stores, a deficient intestinal absorption of iron and reduced bioavailability.4,5 Various randomised prospective studies have demonstrated that in patients with CHF and iron deficiency with or without anaemia, iron repletion improves symptoms, physical performance and quality of life.6 The FAIR-HF7 study shows the importance of diagnosing and treating iron deficiency in patients with CHF. A post hoc of the FAIR-HF study found significant improvement in patients after iron therapy. The clinical benefit was similar in anaemic and non-anaemic patients, in terms of patients’ overall self-perception, NYHA class, HRQoL and exercise capacity.8
It is widely known that anaemia is a common comorbidity in patients with CHF9; it is an independent prognostic marker of mortality, hospital admissions and poor quality of life.10,11 Correction of anaemia to normal or near-normal values has been associated with an improvement in HRQoL, exercise capacity and symptoms of CHF.5,6
Congestive Heart Failure and CKD may share the cause (e.g. hypertension), comorbidities (e.g. malnutrition) and risk factors (e.g. advanced age). Therefore, it is not rare to observe these two diseases together in what is known as cardio-renal syndrome.12–14 In addition, if both entities occur together with anaemia, it is known as cardio-renal anaemia syndrome which represents a major independent risk factor for CHF.15,16
Study design and objectivesA retrospective observational study conducted in 824 patients diagnosed on admission with CHF at Hospital Universitario Marqués de Valdecilla in Santander (Spain) between 1 January 2012 and 11 June 2013.
The primary objective of the study was to determine how many of these CHF patients underwent laboratory testing for iron status evaluation (ferritin and transferrin saturation index [TSI]). The secondary objectives were to determine the percentage of patients with iron deficiency, with or without anaemia, and to quantify the degree of renal impairment.
The number of determinations of serum iron (ferritin or TSI), and haemoglobin (Hb), as well as calculations of glomerular filtration rate (GFR). It should be kept in mind that a single patient corresponded to one hospitalisation with one or more rehospitalisation; none of one, more than one laboratory determinations could be generated in each hospitalisation. Patients’ iron parameters were considered to have been investigated when they had undergone one determination of ferritin or TSI. Additional determination during their hospital stay, were not included in the analysis.
Concomitant comorbidities, degree of CHF and stability of CHF were not analysed.
Anaemia was defined as Hb level <13g/dl in men and <12g/dl in women. Iron deficiency was considered if ferritin levels <100μg/ml, or serum ferritin between 100 and 300μg/ml plus a TSI <20%. GFR was calcululated using the MDRD equation. Patients were divided according to GFR into grades 3–5 and >60ml/min/1.73m2, as recommended by the KDIGO guidelines. A GFR <60ml/min/1.73m2 was considered to be kidney failure.
Statistical analysis was performed using the SPSS v. 15.0 programme (SPSS Inc., Chicago, United States). Quantitative variables with a normal distribution were expressed as mean±standard deviation, and those without normal distribution were expressed as median and interquartile range. Qualitative variables were expressed as relative frequencies. Normality was confirmed with the Kolmogorov–Smirnov test, and homogeneity of variance was confirmed with the Levene test. Comparison of means between 2 groups was performed depending on the variable's distribution, with Student's t test for independent groups or its non-parametric equivalent (the Mann–Whitney U test). Comparison between groups for qualitative variables was performed with the χ2 test. A p value<0.05 was considered to be statistically significant.
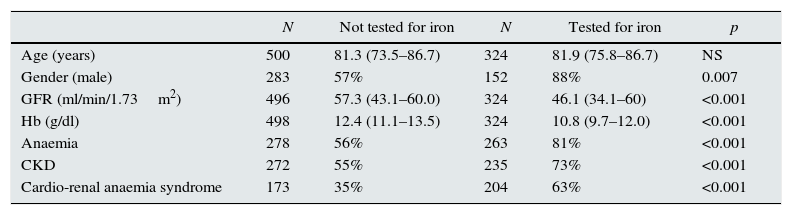
ResultsA total of 824 patients were analysed. Of them, 39% (324) were evaluated for iron parameters. No significant differences were observed with respect to age (81.3 [73.5–86.7] vs 81.9 [75.8–86.7] years), although significant differences were observed with respect to gender (57 vs 88% men; p=0.007). Values of GFR (57.3 [43.1–60.0] vs 46.1 [34.1–60] ml/min/1.73m2) and Hb (12.4 [43.1–60.0] vs 10.8 [9.7–12.0] g/dl) were significantly lower in the group of patients tested for iron (p<0.001). The percentage of patients with anaemia (56 vs 81%), kidney failure (55 vs 73%) or both comorbidities at the same time (35 vs 63%) was significantly greater in the group of patients tested for iron (p<0.001) (Table 1).
Comparison of parameters between patients not tested for iron and tested for iron.
| N | Not tested for iron | N | Tested for iron | p | |
|---|---|---|---|---|---|
| Age (years) | 500 | 81.3 (73.5–86.7) | 324 | 81.9 (75.8–86.7) | NS |
| Gender (male) | 283 | 57% | 152 | 88% | 0.007 |
| GFR (ml/min/1.73m2) | 496 | 57.3 (43.1–60.0) | 324 | 46.1 (34.1–60) | <0.001 |
| Hb (g/dl) | 498 | 12.4 (11.1–13.5) | 324 | 10.8 (9.7–12.0) | <0.001 |
| Anaemia | 278 | 56% | 263 | 81% | <0.001 |
| CKD | 272 | 55% | 235 | 73% | <0.001 |
| Cardio-renal anaemia syndrome | 173 | 35% | 204 | 63% | <0.001 |
Values in parentheses are interquartile ranges.
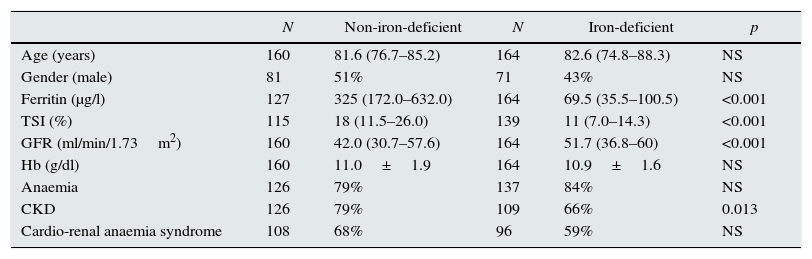
Among the 324 patients evaluated for iron parameters, 164 patients (51%) showed iron deficiency. No significant differences were observed with respect to age or gender between those without iron deficiency and those with iron deficiency. Ferritin was evaluated in 291 patients (90%), 127 (44%) of whom had a level <100μg/l. TSI was estimated in 254 patients (78%), 192 (76%) of whom had a level <20%. Iron parameters for the two groups—ferritin (325 [172.0–632.0] vs 69.5 [35.5–100.5] μg/l) and TSI (18% [11.5–26.0] vs 11% [7.0–14.3])—showed significant differences (p<0.001). GFR also reflected significant differences (42.0 [30.7–57.6] vs 51.7 [36.8–60] ml/min/1.73m2; p<0.001), as did the percentage of patients with CKD (79 vs 66%; p=0.013). By contrast, Hb did not reflect significant differences between the two groups (11.0±1.9 vs 10.9±1.6g/dl) (Table 2).
Comparison of parameters between non-iron-deficient and iron-deficient patients.
| N | Non-iron-deficient | N | Iron-deficient | p | |
|---|---|---|---|---|---|
| Age (years) | 160 | 81.6 (76.7–85.2) | 164 | 82.6 (74.8–88.3) | NS |
| Gender (male) | 81 | 51% | 71 | 43% | NS |
| Ferritin (μg/l) | 127 | 325 (172.0–632.0) | 164 | 69.5 (35.5–100.5) | <0.001 |
| TSI (%) | 115 | 18 (11.5–26.0) | 139 | 11 (7.0–14.3) | <0.001 |
| GFR (ml/min/1.73m2) | 160 | 42.0 (30.7–57.6) | 164 | 51.7 (36.8–60) | <0.001 |
| Hb (g/dl) | 160 | 11.0±1.9 | 164 | 10.9±1.6 | NS |
| Anaemia | 126 | 79% | 137 | 84% | NS |
| CKD | 126 | 79% | 109 | 66% | 0.013 |
| Cardio-renal anaemia syndrome | 108 | 68% | 96 | 59% | NS |
Values in parentheses are interquartile ranges.
This study showed that potential iron deficiency is only studied in 39% of patients who are admitted with CHF to our centre, meaning that opportunities for clinical improvement are lost in many patients. This requires a reconsideration of routine clinical practice in patients with CHF.
In our study, the age structure of the population analysed matched that reflected by the Spanish Statistical Office (INE) in its survey on hospital morbidity17. Thus, 1% of patients were 45 years of age or less, and more than 80% of the population analysed was older than 75 year.
Regarding the prevalence of iron deficiency in CHF, methodological differences in the design of several study have yielded to non uniform results ranging from 13.7%, observed by Hug et al.18; to intermediate reports in the 36–43% range, like those indicated by Range et al.20 and Macdougall et al.4; to 63%, in a study by Comín-Colet et al.19. In our work, iron was only evaluated in 39% of the population, with a prevalence of iron deficiency of 51%, a figure greater than the mean reflected in the studies. This may probably be explained by the limited percentage of population analysed and the older age.
The prevalence of anaemia in CHF has been found to be between 4% and 50%,21,22 depending on the study population and the cut-off values for Hb used to define the lower limit of normal. In a systematic review and meta-analysis, Groenveld et al.23 noted a prevalence of 37%. Extreme prevalences like those noted by Silverberg et al.24 (79%) have undoubtedly been due to methodological differences in study design. In our study, we found an overall prevalence of 66% of anaemic and in the subgroup of 324 patients whose potential iron deficiency had been investigated the prevalence rose to 79% among those who did not have iron deficiency and 84% in those who did have it. In general, our study reflected a greater prevalence than the majority of the studies evaluated. We believe that this may be mainly due to patients’ older age.
Regarding the prevalence of CKD in CHF, the studies analysed have established it in the 30–64% range.25–27 In our study, the prevalence of CKD was 62% overall and 73% in the subgroup of patients who were evaluated for iron (79% in those without iron deficiency and 66% in those with iron deficiency). These percentages were close to the upper end of or even above the range reflected in the studies analysed. Once again, the explanation for this result may be found in the patients’ older age.
The epidemiology of cardio-renal anaemia syndrome is complicated, since it depends on the prevalence of each of its components, which in turn depend to a large extent on the definitions used and the severity of the disease in the population studied. As a result, there has been considerable variation among the published data: from 3% to 22%.28,29 Our results indicated a prevalence of cardio-renal anaemia syndrome of 46% relative to the total population. In the subgroup evaluated for iron parameters, the prevalence rose to 63% (68% in those who did not have iron deficiency and 59% in those who did). As mentioned, the methodological differences in study design, including the age of the population, may account for this difference in prevalence between our study and those reviewed.
Weak aspects of our study were its observational nature, the fact that CHF was diagnosed by assigned physicians without uniform criteria, the fact that it did not analyse reason for admission or degree of CHF decompensation and the fact that it did not include treatments for or analysis of causes of iron deficiency. However, it should be noted that the data that we have presented concerned a single centre, although this does not mean that other centres act differently. The uniformity of the data, as they came from a single centre, and the resulting uniformity of the analytical techniques, must be noted as study strengths.
We believe that the results shown may represent a clear area of improvement for the treatment of heart failure.
ConclusionsIron deficiency, with or without concomitant anaemia, was found to be significantly associated with HRQoL, NYHA functional class and exercise capacity. Bearing in mind the data from prospective studies that have demonstrated clinical improvement with the administration of iron in patients with iron deficiency, early detection should be given more substantial consideration as a therapeutic target in the treatment of CHF. Our results have merely aimed to show that gap in routine medical practice, with limited laboratory determinations of iron levels in patients with CHF.
Conflicts of interestThe authors declare that they have no potential conflicts of interest related to the contents of this article.
Please cite this article as: Belmar Vega L, De Francisco, ALM, Albines Fiestas Z, Serrano Soto M, Kislikova M, Seras Mozas M, et al. Estudio de la deficiencia de hierro en pacientes con insuficiencia cardiaca congestiva: una práctica clínica que precisa mayor atención. Nefrologia. 2016;36:249–254.