La enfermedad falciforme (EF) es la hemoglobinopatía estructural más frecuente en el mundo. Su afectación renal clínicamente significativa ocurre más frecuentemente en los individuos homocigotos que en los heterocigotos o con hemoglobinopatías mixtas, con la excepción del carcinoma medular renal, que es más frecuente en los portadores del rasgo falciforme. Como en otras manifestaciones de la EF, los fenómenos vasooculsivos son el principal mecanismo etiopatogénico. Sus manifestaciones más frecuentes son la hematuria macroscópica asintomática, las alteraciones funcionales tubulares y la necrosis papilar. Menos frecuentes, pero de peor pronóstico, son la glomerulopatía que conduce a enfermedad renal crónica y el carcinoma medular renal. Debido a la alta tasa de inmigración en España y a una mayor supervivencia de estos pacientes se espera una prevalencia creciente en nuestro país. En 2009, la Asociación Española de Hematología y Hemoterapia elaboró las Guías de manejo de la enfermedad falciforme. Este artículo reproduce el capítulo sobre afectación renal actualizado para su difusión en NEFROLOGÍA.
Patients with sickle cell disease exhibits numerous kidney structural and functional abnormalities, changes that are seen along the entire length of the nephron. Changes are most marked in patients with homozygous sickle cell anemia, but are also seen in those with compound heterozygous states and the sickle cell trait. The renal features of sickle cell disease include some of the most common reasons for referral to nephrologists, such as hematuria, proteinuria, tubular disturbances and chronic kidney disease. Therapy of these conditions requires specialized knowledge of their distinct pathogenic mechanisms. Spanish Haemathology and Hemotherapy Association has recently publicated their Clinical Practice Guidelines of SCD management. Renal chapter is reproduced in this article for Nephrology difussion.
INTRODUCTION
Haemoglobin S (HbS) is the most common and well-known structural haemoglobinopathy in the world. This abnormality causes sickle cell disease (SCD), which is a group of disorders that includes the most severe homozygote state (HbSS) and the double heterozygote states (HbSC and HbSβ thalassemia [βº o β+]). SCD is expressed as chronic haemolytic anaemia and a large variety of vaso-occlusive phenomena and their consequences, proliferative vasculopathy, and a predisposition to infections, leading to very high early morbidity and mortality rates. This is therefore a chronic disease with severe economic and psychosocial implications. An early diagnosis of SCD allows the implementation of necessary preventative measures (antibiotic prophylaxis and vaccination) that reduce mortality and morbidity. Kidney abnormalities in SCD start in childhood, with haematuria being the most common manifestation (the leading cause in African Americans), along with renal papillary necrosis and tubular function abnormalities, which are triggered by vaso-occlusive phenomena. The long-term consequences of this condition are sickle cell glomerulopathies (albuminuria in 68% of SCD adults), with evolution to chronic renal failure (CRF) in as many as 20% of homozygous patients.1 Since the life expectancy of patients with SCD has increased in the last decade, the prevalence of CKD secondary to SCD has increased significantly, becoming an independent factor for mortality in these patients.2-4 Renal medullary carcinomas are also associated with the sickle cell trait (HbAS) and, to a lesser degree, with SCD.
The global prevalence of the S gene is estimated at 30 million people. It is especially common in individuals from the areas of tropical and subtropical Africa, the Arabian Peninsula, India, Central America, and the USA. Global epidemiological estimates place the annual birth rate at 300 000-400 000 infants with hereditary haemoglobin diseases (83% SCD, 17% thalassemia syndromes).5-7 In the USA, 8% of the African Americans are heterozygous carrier of the HbS gene, and 1500 homozygous children are born annually. Between 15% and 30% of people in Sub-Saharan Africa are HbS carriers, with SCD present in 2%-3% of the population, with approximately 180 000 new births every year affected with SCD in Sub-Saharan Africa.6 Haemoglobinopathies in the Americas are the result of migrations and mixing with other races. The African slave market had a decisive impact on the presence of abnormal haemoglobin in the Caribbean and tropical America, such that the prevalence of sickle cell anaemia at birth in Latin America is 16%, with a frequency of 6.1%-18% of HbS gene carriers in Caribbean populations of African descent.
Since 2000, Spain has experienced one of the largest immigration rates in the world. According to data from December 2010,8 12.2% of Spanish residents are foreigners, and 44.22% of them are Latin American and 39% African. This has led to a progressive increase in the incidence of haemoglobinopathies in Spain, along with the growing immigrant birth rate, which surpassed 15% in the regions of the Northeast, centre, and East of the Iberian Peninsula. According to data from the Programa de Prevención de Minusvalías en Recién Nacidos (Handicap Prevention Programme in Newborns) which has implemented a universal screening programme for haemoglobinopathies in the region of Madrid since May 2003, there is a progressive increase in the incidence of haemoglobinopathies in this region (prevalence of haemoglobinopathies in 2005 was 6.17%, compared to 5.13% in 2004, with a global prevalence of 5.57% for the time period of 2003-2005, [personal communication]). This trend is without a doubt due to the increased rate of immigration from high-risk countries in recent years along with the birth rate in our country (74.21% of all foreigners born in Spain are of African descent, especially from the country of Morocco, with 59.13% of all foreign births in Spain).8
Given the limited clinical experience in Spain and the recent advances made in the treatment of this disease (treatment with hydroxyurea [HU], treatment of the life-threatening complications of the disease such as stroke and acute chest syndrome, haematopoietic progenitor transplantation, transfusion programmes, and chelation therapy) that improve quality of life and extend the mean survival of these patients, the Grupo de Eritropatología,Sociedad Española de Hematología y Hemoterapia (Erythropathology Group of Spanish Society of Haematology and Haemotherapy) started the initiative of elaborating a set of treatment guidelines for SCD that was recently published.9 In this article, we reproduce the chapter regarding kidney abnormalities for dissemination in Nefrología. Table 1 summarises the various manifestations of SCD in the kidneys.
HAEMATURIA AND RENAL PAPILLARY NECROSIS
Asymptomatic haematuria
This is the most common form of SCD. It can be microscopic, or more commonly, macroscopic and self-limiting. It is frequently unilateral, and is more often found in the left kidney, due to the longer left renal vein and its anatomical location, compressed between the aorta and the superior mesenteric artery. This subjects this vessel to a greater venous pressure with relative hypoxia in the renal medulla that favours cell sickling. It can develop at any age, and has been primarily described in patients with sickle cell trait (HbAS) much more frequent than in the homozygous form (HbSS).
Renal papillary necrosis and renal infarction
They are also common complications of SCD, with an estimated prevalence of 30%-40% in homozygous HbSS patients.10 The clinical presentation of this condition varies from asymptomatic macroscopic haematuria (not always present) to an acute condition involving pain, fever, and even obstructive acute renal failure (ARF). However, a similar frequency of renal papillary necrosis (RPN) has been described in symptomatic and asymptomatic individuals (65% and 62%, respectively).11 This may be at times associated with urinary tract infections (61.5%), for which it is considered a favouring factor or risk modifier.
Pathological anatomy
The histological changes that tend to occur in isolated haematuria are relatively minor and are primarily manifested as medullary congestion. After the initial phase of dilation and congestion, the vasa recta are destroyed in fibrotic areas. The papillae are dependent on the vasa recta; therefore, when they are destroyed it produces small repeated focal infarctions of the papillae. The subsequent RPN is a focal process, and some collecting tubules survive within a diffuse area of fibrosis. The most important changes produced in the renal medulla affect the internal medulla and papilla, resulting in dysfunction of the collecting tubules of the juxtamedullary nephrons.
Aetiopathogenesis
Haematuria is probably a consequence of cell sickling in the renal medulla combined with vascular obstruction and extravasation of erythrocytes. The medullary environment is by nature prone to producing sickle cells due to the partial pressure of O2 at 35-40mm Hg, below the sickling threshold of 45mm Hg, along with high osmolarity that dehydrates erythrocytes and concentrates the HbS and the acidic pH that also increases the probability of sickling.
Diagnosis
Continuous or persistent macroscopic haematuria in a patient with SCD or sickle cell trait (HbAS) indicates a renal sickle cell crisis. However, other more severe and treatable causes of haematuria, such as renal medullary carcinoma, must first be ruled out. The presence of intense pain widens the potential differential diagnosis, especially in the presence of a renoureteral crisis (lithiasis or renal papilla) or renal infarction. Haematuria may be asymptomatic or produce a moderate lumbar pain, which, if unilateral, can indicate the location of bleeding.
Clinical suspicion is very important for the diagnosis of RPN. Renal ultrasound is the technique of choice for the detection and differential diagnosis against lithiasis and renal medullary carcinoma. The earliest finding in RPN is increased echogenicity in the medullary pyramids (the innermost region of the medulla), which, in the absence of hypercalciuria in a patient with SCD and haematuria suggests RPN. In later stages, calcification may appear in the medullary pyramids with a typical 'garland pattern' surrounding the renal pelvis, or a defect in echogenicity in the pyramids due to detachment of the papilla. Intravenous pyelogram, which should be avoided in these patients due to the elevated risk of nephrotoxicity from iodinated contrast solutions, was used in initial studies of SCD and showed a 39% calyceal clubbing deformity or swelling, which is not accompanied by the cortical scarring characteristic of chronic pyelonephritis. In cases of uncertainty, helical CT scans are more sensitive than ultrasound for early detection of RPN, as well as for renal medullary carcinoma, although prophylactic measures must always be taken to prevent nephrotoxicity from iodinated contrast solutions, and especially volume expansion.
Treatment
Since the pathology of sickle cell haematuria is generally benign and self-limiting, a conservative treatment with bed rest is appropriate for avoiding the detachment of microthrombi.
Forced diuresis should be maintained (at 4l/1.73m2 per day) using hydration, preferably with hypotonic solutions, along with administration of thiazide or loop diuretics. This will reduce medullary osmolarity and may reduce cell sickling in the vasa recta, as well as aids in eliminating clots in the urinary tract. Volume expansion with saline solution must be avoided, since this would be ineffective at reducing blood osmolarity, and transfusions can increase the risk of heart failure.
Combined treatment with vasopressin is defended by some authors, since this would induce hydration of the erythrocytes, decreasing the concentration of HbSS and thus the rate of cell sickling.12
Alkalisation is also recommended, as this is potentially useful for increasing the affinity of Hb for O2 and decreasing the rate of cell sickling, as well as reducing tubule toxicity in haemoglobinuria. However, it has not been proven as an effective treatment method.
The use of ε-aminocaproic acid is reserved for those cases in which previous treatment methods have failed, and this method requires a great deal of precaution due to the high risk of thrombosis.
In isolated cases of severe haematuria that has not responded to the previously mentioned treatment options, arteriographic localisation and selective embolisation of the affected renal segment may ensue in order to prevent a nephrectomy.
In any case, the treatment of haematuria must be included within the general treatment of SCD, especially the use of hydroxyurea (HU), which has been proven effective in both adults and children at reducing the incidence of crises with an acceptable safety profile.13 The use of antioxidant agents such as ascorbic acid could protect kidney cells from oxidative damage from HU and increase safety.
TUBULAR FUNCTION ABNORMALITIES
Functional abnormalities in the distal nephron
1. Hyposthenuria. Defective urine concentrations or hyposthenuria is the earliest and most common tubular abnormality in SCD. The maximum urine concentration that these patients can reach is 400-450mosm/Kg, but this generally has no clinical consequences. This condition can appear very early in homozygous individuals, and manifests itself as enuresis and a greater risk of dehydration. Dehydration is more likely in the case of coexisting extra-renal water losses or insufficient input if ingestion is not possible. This condition can be reversible in children under 10 years of age using blood transfusions. In older patients, generally after 15 years of age, microthrombi in the vasa recta lead to their progressive loss with obliteration and tortuosity of the remaining vasa recta, as observed using angiographic techniques and the observation of fibrosis in the renal medulla. In this case the diagnosis is irreversible nephrogenic diabetes insipidus, whose most common clinical manifestations are nocturia, polyuria, and polydipsia.
2. Distal tubular acidosis. The most incipient abnormality is the incomplete distal tubular acidosis that accompanies hyposthenuria. The appearance of hyperkalaemia is rare unless there are concurrent conditions that affect renal compensatory mechanisms, such as concomitant treatment with non-steroidal anti-inflammatory agents, renin-angiotensin-aldosterone system inhibitors, betablockers, or renal failure.
Supranormal proximal tubular function
Abnormal proximal tubular function in SCD increases the reabsorption of sodium and decreases its urine excretion, diminishing or nullifying the response to loop diuretics. These abnormalities could be adaptive due to compensation for the incapacity of the renal medulla to reabsorb water and sodium. Proximal reabsorption of phosphate that is generally accompanied by sodium reabsorption is also increased, leading to hyperphosphataemia, above all in the presence of phosphate overload, such as in haemolysis. Since the tubular secretion of creatinine (cr) is preserved, serum cr and cr clearance (Ccr) tests overestimate glomerular filtration rate (GFR). Differences have been observed of up to 30% in the estimation of GFR using inulin clearance and Ccr values in these cases.
The secretion of uric acid is increased, possibly as an adaptive mechanism to the increased in uric acid production during haemolysis, which tends to coexist with high serum levels and the risk of gout. An increase in the reabsorption of β2-microglobulin has been described, with consequent increases in blood levels.
Aetiopathogenesis
An intact collecting tube is required in close proximity with medullary vasa recta in order to concentrate urine. The juxtamedullary nephrons are the most highly implicated in urine concentration mechanisms, since these collecting tubules reach the deepest areas of the renal medulla. If reabsorbed sodium cannot be cleared by circulation through the vasa recta, reabsorption is affected. As we have explained earlier, since cell sickling is initially produced in the vasa recta in a highly hypertonic, acidic, and relatively hypoxic environment, their obliteration alters counter-current medullary mechanisms, impeding the reabsorption of free water and leading to medullary congestion.
However, the urinary diluting capacity remains intact, as well as the secretion of ADH, due to the preservation of the superficial area of the loops of Henle in the cortical nephrons, irrigated by peritubular capillaries.
Acid excretion requires a proton gradient from the cellular apex of the tubule to the lumen, and occurs in the collecting tubule. Although the exact aetiopathogenic mechanism of distal renal tubular acidosis of SCD patients is unknown, it is believed that the damage to renal medullary vascularisation and secondary hypoxia may affect the supply of energy needed to maintain the electrochemical and hydrogen ion gradients in the collecting tubules. Since the primary damage produced in SCD occurs in the deepest segment of the loop of Henle, a severe defect in urinary acidification would be very rare in SCD, such that acidosis is incomplete. However, there may be disorders in the acidification and excretion of potassium when administering angiotensin converting enzyme (ACE) inhibitors, betablockers, and potassium-sparing diuretics, or when the patient suffers from renal failure.
With regard to supranormal proximal tubular function, the aetiopathogenic mechanism suggested by some authors14 is the release of prostaglandins stimulated by ischaemia in the renal medulla. An inhibitory effect of indometacin has been observed in the proximal reabsorption of sodium, which is greater in patients with SCD than those without it.15 The inhibition of prostaglandins re-establishes normal proximal sodium reabsorption, which is increased in SCD, causing the decreased natriuretic response to loop diuretics observed in these patients. Furthermore, the increased levels of prostacyclins and prostaglandin E2 found in patients with SCD13 could at least partially mediate the secretion of renin into the bloodstream and the synthesis of aldosterone (high levels of plasma renin have been observed in of SCD patients),16 although the tendency for hyperkalaemia is practically independent of aldosterone.
Diagnosis
Patients with SCD and hyposthenuria reach a maximum urinary osmolarity of 400-500mOsm/kg after 8 hours to 10 hours thirst, in comparison to 900-1200mOsm/kg in normal subjects. Additionally, this condition does not respond to vasopressin.
Incomplete distal renal tubular acidosis occurs following an overload of ammonium chloride, which would cause reduced urine acidification (pH of 5.8 vs 5.1) in normal subjects, in spite of normal ammonium excretion. The titratable acidity is thus reduced in these subjects.
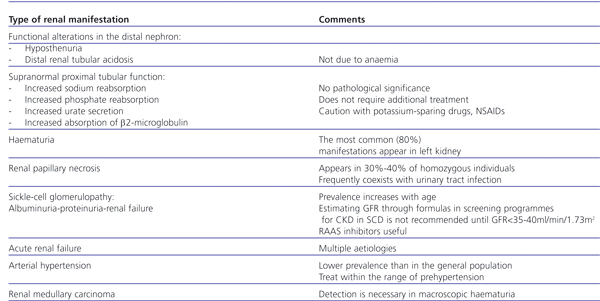
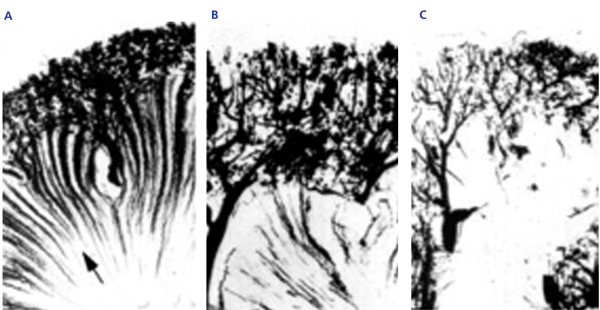
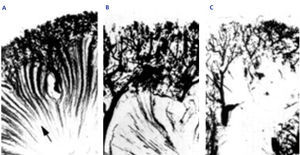
Damage and destruction of the vasa recta, both in sickle cell trait patients and more severely in SCD, can be observed using angiographic techniques (Figure 1).
Treatment
The majority of tubular abnormalities in SCD patients do not require treatment in addition to symptomatic treatment in pathological situations leading to dehydration or volume overload, according to the predominant functional abnormality.
Thus we recommend establishing preventative measures in these cases, as well as being cautious when using drugs that favour hyperkalaemia such as betablockers, COX-2 inhibitors, or renin-angiotensin-aldosterone system inhibitors, and avoid nephrotoxic compounds, especially in patients with hyposthenuria.
SICKLE CELL GLOMERULOPATHY
Patients with SCD may develop proteinuria and renal failure that progresses into terminal chronic kidney disease (CKD). The renal involvement responsible is a glomerulopathy whose initial marker is albuminuria. The prevalence increases with age, ranging between 21.3%17 and 28%18 in patients aged 3 to 20 years, of which 10.5% of cases progress to proteinuria within a 20-month follow-up period. In most cases (72%) it continues to progress into renal failure, according to retrospective studies. A cross-sectional study involving 90 children reported that prehypertension and hypertension, along with level of anaemia, were independently associated with the presence of albuminuria.19 Prospective studies are needed to determine the causal relationship of these findings, as well as the potential benefits of treatment for the development of albuminuria.
In a recent prospective study involving 300 adults aged 20 to 70 years,1 the prevalence of albuminuria was 68% (26% proteinuria) in homozygous individuals, as opposed to 32% (10% proteinuria) in heterozygous ones. In this same study, 21% of patients had renal failure as calculated using the Cockroft-Gault formula. However, determining serum cr or even the GFR using this value, which is a parameter used for staging CKD under the current classification system,20 would not be useful in SCD until advanced stages of the disease (GFR<30-40ml/min/1.73 m2),21 since tubular secretion of cr is maintained with an abnormal GFR, as explained earlier. When albuminuria appears in SCD patients, the glomerular ultrafiltration coefficient is significantly reduced compared to SCD patients without albuminuria, even in those with preserved GFR, meaning that albuminuria is a very sensitive marker for the glomerular damage caused in SCD, unlike in other nephropathies such as type-2 diabetes. For this reason, some authors15 have recommended measuring blood levels of cystatin C as a better approximation of GFR than those based on serum cr levels, although more studies are needed to confirm this.
Although proteinuria can reach nephrotic levels, it increases gradually with age, and so its clinical progression is different from the sudden onset type observed in nephrotic syndromes such as idiopathic focal segmental glomerulosclerosis (FSGS) and minimal-change glomerulonephritis.
Proteinuria is associated with higher levels of anaemia, haemolysis, and reticulocytosis,22 and has also been correlated with the incidence of painful crises, cholelithiasis, acute chest syndrome, and stroke. This condition is more prevalent in patients with 4 intact α-globin genes and less prevalent among α-thalassemia patients, with prevalence of 40% among HbSS adults without α-thalassemia, and only 13% in HbSS adults with α-thalassemia. Additionally, mean BP is greater with 4 intact α-globin genes than in subjects with α-thalassemia.23
The prevalence of arterial hypertension (AHT) in CKD from SCD is notably lower than in other causes of CKD,17 as previously mentioned.
Pathological anatomy
Four different types of glomerulopathy have been described in SCD: FSGS, membranoproliferative glomerulonephritis (MPGN), glomerulopathy specific to SCD, and thrombotic microangiopathy (TMA).24 Regardless of which type of glomerular damage is present, all renal biopsies from SCD patients show hypertrophied glomeruli with distended capillaries due to the sickled blood cells, which is described as a glomerulopathy specific to SCD, and is also found in subjects with SCD and no clinical evidence of CKD. Haemosiderin deposits in tubular cells are an almost universal finding. The most common glomerulopathy is FSGS,24,25 which was observed in 39% of renal biopsies taken from 18 patients with SCD and proteinuria and/or renal failure, which until now is the largest study recently published.24 According to the Columbia classification system, there are different subtypes: NOS, tip, perihilar, and collapsing, as well as mixed forms.24 Interstitial fibrosis is frequently observed with tubular atrophy adjacent to sclerotic glomeruli. Since this disease mainly affects juxtamedullary glomeruli vascularised by the vasa recta, it is frequently accompanied by severe medullary fibrosis. Both immunofluorescence and electron microscope analyses provide evidence of an absence of immune deposits. In a smaller percentage of cases, global glomerular sclerosis is observed.26 There have also been cases of focal cortical infarcts.
The second most frequently observed type is MPGN, which was originally the first glomerular abnormality reported in SCD. Although it has been associated with nephropathy due to HCV and HIV, none of the 5 cases described in the study by Maigne et al24 were attributable to this relationship. Indirect immunofluorescence tests can reveal immune deposits predominantly in the capillary wall of IgG, IgM, IgA, C3, and C1q. Interstitial fibrosis is found in most cases.
Characteristic lesions from TMA are evident in 17% of cases accompanied by some level of interstitial fibrosis.24
Aetiopathogenesis
It is believed that the initial mechanism for the development of a glomerulopathy in this context is hyperfiltration or increase in GFR, which is common in SCD patients, especially children.14 Additionally, renal plasma flow is elevated even more than GFR, such that the filtration fraction is reduced in SCD patients as compared to normal subjects.15 One explanation for this finding could be that increased cortical plasma flow caused by the vasodilatory effect of prostaglandins could reduce the efficacy of diffusion due to the increased velocity (inhibition of prostaglandins re-establishes normal renal plasma flow and filtration fraction). However, hyperfiltration in SCD is not only associated with haemodynamic changes, but glomerular permeability and the glomerular filtration coefficient (Kf) are also increased.27 Increased transglomerular traffic of macromolecules associated with defects in the podocyte barrier due to glomerular hypertrophy could be the cause of SCD-associated glomerulosclerosis27 in a similar manner as in non-insulin-dependent diabetes mellitus.28
The glomerular hypertrophy consistently found in SCD could be at least in part secondary to chronic anaemia (concordant with a lower prevalence of renal damage in patients with other types of less anaemic SCD, such as HbSC). However, proteinuria in SCD is not universal, nor is it related to the number or severity of crises, indicating that other factors are involved.
Hyperfiltration, glomerular hypertrophy, and FSGS are not necessarily sequential or causal. Some common mechanism may act in all three conditions, such as growth factors or inflammatory cytokines. FSGS may be the cause, and not the consequence, of interstitial fibrosis. This could obstruct efferent arterioles, thus increasing intraglomerular pressure and resulting in glomerular sclerosis.
We have already commented on the protective role of α-thalassemia against the development of sickle cell glomerulopathy, which is more prevalent with four intact α-globin genes and is not related to the level of anaemia. Improved rheology and decreased erythrocyte adhesiveness would imply a reduced damaging effect on the endothelium, and thus, reduced organ damage.1
Other genes may be involved in the development of CKD in patients with SCD. Recently, the haplotype of gene MYH9 was proven to be associated with CKD due to its involvement in podocyte malfunction due to defects in the structure of myosin IIA.29 This gene is very common (>60%) in African Americans and people from Sub-Saharan Africa, populations in which SCD is also particularly common. Currently, insufficient evidence exists in the medical literature regarding the role of MYH9 mutations as modifiers of the phenotypic expression of SCD. In a recently published study regarding genetic modulators of the severity of SCD, involving 1265 patients from the Cooperative Study of Sickle Cell Disease, the MYH9 gene was not mentioned.30
Diagnosis
Patients with SCD must be considered at-risk for CKD, and should have regular (at least once per year) measurements of the urinary albumin to creatinine ratio (UACR) for early detection in children, for example, after 7 years of age, particularly in severe cases of SCD.
The first urine in the morning is recommended for laboratory analyses. In cases of positive UACR, a second measurement is required for confirmation. The criteria for positive albuminuria (UACR>30mg/g) and proteinuria (UACR>300mg/g) are those used for CKD.18
When patients test positive for albuminuria, we recommend measuring blood levels of cystatin C or using isotope analyses (99Tm-DTPA, 125I-iothalamate) for estimating GFR. We do not recommend estimating GFR using formulas recommended by international guidelines for CKD screening programmes in SCD patients until there is a significantly altered GFR (<35-40ml/min/1.73m2).
Seropositivity must be tested for hepatitis virus and HIV due to the elevated prevalence of these diseases in SCD patients and their association with glomerulopathies.
A kidney biopsy must be considered in cases of rapid-onset nephrotic syndrome or rapidly progressing kidney disease.
Treatment
The evolution of patients with albuminuria should be monitored, and at least those patients with proteinuria should be treated, due to the increased probability of renal function deterioration. Sickle cell nephropathy, as well as other proteinuric glomerulopathies, is probably modifiable using measures to halt its progression, such as renin-angiotensin-aldosterone system inhibitors. More evidence has been compiled for ACE inhibitors, which have been shown to reduce proteinuria in adults and children with SCD.16,26 The use of these drugs implies a greater risk of hyperkalaemia in patients with SCD due to haemolysis, making preventative measures especially necessary, along with monitoring potassium levels and even suspending treatment in haemolytic crises.26
It is possible that HU or transfusions may have some protective value, especially because of the importance of anaemia and haemolysis as risk factors for kidney disease. Treatment with HU has been shown to prevent the development of proteinuria in children and even decrease the rate of albuminuria.16 This drug improves anaemia and erythrocyte rheology, reduces leukocytosis, and modulates the expression of adhesion molecules. The combined use of ACE inhibitors and HU can prevent the progression of microalbuminuria to proteinuria,31 although its effect in preventing renal failure has not been evaluated.
Steinberg et al32 recently published their results from a long-term follow-up of 299 patients included in the Multicenter Study of Hydroxyurea in Sickle Cell Anemia spanning 17.5 years. These authors observed a global prevalence of CKD of 17.4%, 19% in patients that received HU during a cumulative period less than 5 years, and 5% in patients treated with HU for 15 years or more. The safety of this drug and the reduced mortality observed in patients receiving long-term HU treatment show that CKD could become one of the expanded criteria indicated for HU treatment in SCD patients without frequent vaso-occlusive events.32
ACUTE RENAL FAILURE
Acute renal failure (ARF) is not uncommon in SCD. An estimated 10% of patients that require hospitalisation have at least doubled values of serum cr, which may be due to various causes that often coexist. The most commonly observed precipitating factor is depleted volume. The use of NSAIDs is probably at least partially responsible for many cases of acute renal failure by inhibiting the previously mentioned renal compensatory mechanisms mediated by prostaglandins. It is usually associated with infections, rhabdomyolysis, and anaemia (mean Hb: 6.4g/dl vs Hb: 8.7g/dl in patients without acute increase in cr levels). The majority of patients survives and recovers kidney function.33
The incidence of ARF during acute vaso-occlusive crises is low (4.3%) and appears to be related to the severity of the crisis, 13.6% in severe acute chest syndrome. It appears to be limited to patients with pulmonary hypertension (PHT); therefore, venous congestion may be implicated as the pathogenic phenomenon.34 Acute failure of at least two major organ systems (kidneys, heart, lungs, etc.) during an acute painful vaso-occlusive crisis is considered to be a multi-organ failure. In these cases, individualised erythrocyte exchange may be indicated, according to the USA guidelines for apheresis.35
Obstructive ARF may be produced due to papillary necrosis or macroscopic haematuria.
ARF has also been described in subjects with sickle cell trait (HbAS) associated with rhabdomyolysis and disseminated intravascular clotting after rigorous military training.
ARTERIAL HYPERTENSION
Patients with sickle cell disease have lower blood pressure (BP) than healthy African American controls adjusting for age, but this is not the case for patients with sickle cell trait, who have similar BP values.17 The prevalence of AHT is estimated to be lower than in the general population (2%-6% vs 28%, respectively).
The potential aetiopathogenic mechanisms are obstruction of the vasa recta and repeated ischaemia in the renal medulla, which are involved in hyposthenuria, as well as the lower body mass index and reduced arterial rigidity described in these patients. Recent studies have also suggested that endothelial dysfunction and systemic vasculopathy are associated with a decreased bioavailability of nitric oxide in SCD patients. Even within the normal range of BP, the occurrence of stroke36 has been associated with systolic BP of 120-139mm Hg or diastolic BP of 70-89mm Hg, defining the category of relative systemic AHT in SCD patients, also associated with a higher risk of PHT and renal dysfunction.37
The relationship between PHT and higher BP values in adults with SCD supports the possibility of a pathophysiological mechanism acting in both conditions. Additionally, AHT contributes to left ventricular diastolic dysfunction, which has been shown to be an independent predictive factor for SCD patient death. Even mild increases in pulmonary arterial pressure are poorly tolerated by SCD patients, which could be extrapolated to AHT.
Given this evidence, antihypertensive treatment may be indicated in the category of prehypertension36 (systolic BP: 130-139mm Hg; diastolic: 80-89mm Hg) or even earlier in SCD patients due to the risk of target organ damage (heart, lungs, and kidneys). This condition would be a new component to be added to the six situations enumerated in the seventh report by the Joint National Committee38 with indications for antihypertensive treatment for patients in the prehypertension phase: heart failure, post-myocardial infarction, high risk of coronary disease, diabetes mellitus, CKD, and the prevention of stroke recurrence. Nevertheless, more clinical trials are needed in order to establish the guidelines for treatment and objectives of BP in SCD patients.
Given the aetiopathogenic mechanisms established in SCD-related CKD and their extrapolation to other glomerulopathies, renin-angiotensin-aldosterone system inhibitors would be the treatment of choice for pre-AHT in SCD with albuminuria or PHT. In the case of AHT, this recommendation remains valid along with measures for avoiding hyperkalaemia, especially with regard to potassium-sparing drugs, as previously mentioned.
We do recommend special precaution when using diuretics, since dehydration may precipitate vaso-occlusive crises, and we must also remember that these patients are predisposed to these crises due to the almost universal hyposthenuria observed in SCD patients.
RENAL MEDULLARY CARCINOMA
Renal medullary carcinomas are rare, with an extremely poor prognosis, and are described almost exclusively in the black population with sickle cell trait, and less frequently with SCD. It appears in the majority of cases before the patient has reached 20 years of age, with a higher incidence in men. A genetic predisposition has been suggested, and this disease is distinguished from carcinoma of the collecting tubules by certain markers, including a factor that is inducible by hypoxia. Medullary hypoxia in SCD can promote its development.
Its most common clinical presentation is macroscopic haematuria, lumbar pain, and abdominal mass and/or constitutional syndrome. By the time the carcinoma is diagnosed, usually it has already metastasised, making extirpation of the tumour a non-curative approach. Survival after diagnosis does not surpass 6-12 months.
The appearance of macroscopic haematuria should alert the physician to the possible diagnosis of renal medullary carcinoma in children with sickle cell trait or SCD. The diagnosis should be confirmed by a CT scan.
URINARY TRACT INFECTIONS
Patients with SCD have reduced humoral immune response due to splenic infarctions, which predisposes them to encapsulated bacterial infections, including urinary tract infections (UTI). Special attention must be given to its appearance during gestation, and we have already mentioned that it can contribute to RPN.
As in other infections, UTI can cause sickle cell crises, which should be taken into consideration in children due to the higher frequency of asymptomatic UTI.
ADVANCED CHRONIC KIDNEY DISEASE
Sickle cell disease accounts for less than 1% of patients that start renal replacement therapy in the USA.39
In this article we have reviewed the various renal manifestations of SCD, its pathophysiological mechanisms, risk factors, diagnosis, and treatment. CKD has been described frequently in adults and children with SCD, almost always secondary to sickle cell glomerulopathy. In principle, any advancement in the treatment of SCD that limits the frequency and severity of sickling would improve the renal consequences of SCD. We will comment on the particularities of CKD stages 3b-5 in patients with SCD in this section.
Anaemia in SCD patients with CKD can be multifactorial, due to decreased erythropoiesis and haemolysis, but a ferropoenic condition is also quite common due to gastrointestinal losses. As such, appropriate treatment must take these aspects into account.
Treatment is based on transfusions and/or erythropoiesis stimulating agents, whether alone or in combination with HU,40 although the use of erythropoiesis stimulating agents is not entirely established. The target haemoglobin is also uncertain, although it is not recommended to correct it when levels are greater than 10g/dl, and when correcting, avoid haematocrit increases greater than 1%-2% weekly, since greater haemoglobin levels or a faster correction could cause vaso-occlusive crises.
HU is eliminated by the kidney, and so doses must be adjusted in renal failure.
Dialysis
In a study using data from the USRDS registry involving 397 incident patients on dialysis with SCD,41 global two-year mortality was similar to values in patients with terminal CKD (TCKD) without SCD (33% and 37%, respectively). However, patients with SCD were much younger at the start of renal replacement therapy (mean age of 40 years vs 60 years). Adjusting for age, patients with SCD had a lower survival rate than patients without SCD, such that the survival rate at a mean age of 35 years in patients with TCKD and SCD was 60% at three years and 40% at 5 years, compared to 80% and 70% in the population of patients with TCKD and no SCD, respectively.
Transplant
A recent study42 demonstrated a 1-year-survival rate adjusted for age in kidney transplant recipients that was similar between the group with SCD and the group without SCD. However, graft loss increased significantly with the duration of follow-up in transplanted patients with SCD, compared to patients without SCD. Scheinman et al43 analysed USRDS data up to the year 2000. A total of 237 transplant patients with SCD had a survival rate of 56%, whereas 1419 SCD patients on dialysis had a survival rate of 14%. In addition, only 53 of the transplant patients corresponded to the era of anticalcineurinic agents, i.e. 1991, as opposed to TCKD 957 patients with SCD in the same period. As such, we believe that the best option for renal replacement therapy in patients with TCKD is kidney transplantation, although a greater frequency of post-transplant crises has been described in correlation with anaemia correction. Moreover, sickle cell nephropathy can recur in the graft even within 3.5 years, although graft loss due to this cause is rare. HU has been suggested to prevent recurrence.
Due to the high rate of hyperimmune individuals among SCD patients, new immunosuppression treatments may offer advantages in the prognosis of kidney transplants in SCD.
Patients must be well informed about the potential benefits and complications before being included on a transplant list.
SICKLE CELL TRAIT
The prevalence of sickle cell trait (HbAS) is approximately 8%-10% in African Americans, and reaches 25%-30% in certain areas of Western Africa. Approximately 30 million people in the world (2.5 million in the USA) are heterozygous for the HbS gene. Sickle cell trait is a benign carrier state with no haematological manifestations, and normal erythroid parameters (morphology, corpuscular indices, reticulocytes). These individuals do not suffer from anaemia, and do not require treatment or suffer work restrictions.
Although this condition is asymptomatic in the large majority of affected individuals, some clinical complications are possible due to vaso-occlusion in the case of very high fever and/or in conditions of significant hypoxia (such as high altitude mountain climbing), vigorous exercise, and anaesthetic complications. There is a low risk of sudden death associated with vigorous exercise, particularly at high altitudes and when complicated by dehydration and acidosis, which are circumstances that may produce rhabdomyolysis, disseminated intravascular coagulation, and renal failure.
Spontaneous sickling can occur in the renal papilla (normally under low oxygen pressure) in patients with RPN; therefore, 5% of patients with sickle cell trait (HbAS) can suffer episodes of haematuria at some point during their lives (this is a common cause of haematuria in African Americans). The majority of patients develop a deteriorated capacity for concentrating urine, which is directly related with the percentage of intra-erythrocyte HbS. Hyposthenuria develops over time, but is reversible until a certain age with the aid of transfusions. Urinary infections may be more common, and there is an association with renal medullary carcinoma.
Gestating women with sickle cell trait have a greater incidence of bacteriuria and pyelonephritis, as well as pregnancy-related hypertension.
Acknowledgements
The authors would like to thank the Grupo de Eritropatología de la Asociación Española de Hematología y Hemoterapia for their permission for publication of this article, which is a section from their Guía de Manejo de la Enfermedad Falciforme (Sickle cell Disease Management Guidelines), for dissemination in Nefrología.
Table 1. Renal manifestations of sickle cell disease
Figure 1. Arteriography of a normal subject (A), a subject with sickle cell trait (B), and a subject with sickle cell disease (C)