Osteoporosis (OP) and chronic kidney disease (CKD) both independently affect bone health. A significant number of patients with CKD have decreased bone mineral density (BMD), are at high risk of fragility fractures and have an increased morbidity and mortality risk. With an aging population, these observations are not only dependent on “renal osteodystrophy” but also on the associated OP. As BMD predicts incident fractures in CKD patients (part I), we now aim to analyze the potential therapeutic consequences. Post hoc analyses of randomized studies have shown that the efficacy of drugs such as alendronate, risedronate, raloxifene, teriparatide and denosumab is similar to that of the general population in patients with a mild/moderate decline in their glomerular filtration rate (especially CKD-3). These studies have some flaws however, as they included mostly “healthy” women with no known diagnosis of CKD and generally with normal lab test results. Nevertheless, there are also some positive preliminary data in more advanced stages (CKD-4), even though in CKD-5D they are more limited. Therefore, at least in the absence of significant mineral metabolism disorders (i.e. severe hyperparathyroidism), the potential benefit of these drugs should be considered in patients with a high or very high fracture risk. It is an important change that the new guidelines do not make it a requirement to first perform a bone biopsy and that the risk/benefit ratio of these drugs may be justified. However, we must also be aware that most studies are not consistent and the level of evidence is low. Consequently, any pharmacological intervention (risk/benefit) should be prudent and individualized.
La osteoporosis (OP) y la enfermedad renal crónica (ERC) influyen independientemente en la salud ósea. Numerosos pacientes con ERC presentan una disminución de densidad mineral ósea (DMO), un elevado riesgo de fracturas por fragilidad ósea y un incremento de su morbimortalidad. Con el envejecimiento de la población estos hechos no son dependientes solo de la «osteodistrofia renal» sino también de la OP asociada. Dado que la DMO tiene capacidad predictiva en pacientes con ERC (parte I), ahora analizaremos las implicaciones terapéuticas derivadas. Análisis post hoc de estudios aleatorizados han mostrado que fármacos como alendronato, risedronato, raloxifeno, teriparatida o denosumab tienen una eficacia comparable a la población general en pacientes con una disminución leve-moderada del filtrado glomerular (especialmente ERC-3). Estos estudios tienen limitaciones, pues incluyen mayoritariamente mujeres «sanas», sin diagnóstico conocido de ERC y habitualmente con parámetros normales de laboratorio; sin embargo, también existen datos positivos preliminares en estadios más avanzados (ERC-4) y más limitados en ERC-5D. Por todo ello, al menos en ausencia de alteraciones significativas del metabolismo mineral (i.e., hiperparatiroidismo severo), el beneficio potencial de dichos fármacos debería ser considerado en pacientes que presenten un riesgo de fractura elevado o muy elevado. Es novedad importante que las nuevas guías no condicionan su uso a la práctica de una biopsia ósea previa y que el beneficio/riesgo de estos fármacos podría estar justificado. Sin embargo, debemos considerar que la mayoría de estudios no son consistentes y tienen un bajo grado de evidencia, por lo que la indicación farmacológica (riesgo/beneficio) debe ser individualizada y prudente.
Osteoporosis (OP) and chronic kidney disease (CKD) increase with aging causing an exponential increase in the incidence of fractures with significant clinical consequences.1–4 We have described that CKD and alterations in bone-mineral metabolism (CKD-MBD) are also associated with accelerated aging,5 and in a first part of this review1 we showed that, especially in early stages of CKD without important biochemical abnormalities of CKD-MBD, the risk of fracture could be more related to “primary” OP (postmenopausal and senile) than to “renal osteodystrophy” (ROD) itself. In fact, the incidence of fractures does not seem to be reduced in recent years despite the evident improvements in the treatment of hyperparathyroidism and/or hyperphosphatemia.6 Although there are data that show that correction of these abnormalities may reduce the risk of fracture,7 the number of clinical studies are not sufficient and it is necessary to evaluate other risk factors present in this population. For all these reasons, we emphasize that the nephrologist should not ignore the importance of assessment of fracture risk in CKD patients, as it is recommended for the general population.1,2
Although this issue is being addressed by clinical guidelines8,9 (Table 1), nephrologists do not systematically evaluate for the diagnosis and treatment of OP of patients with CKD. A possible explanation is the limitations to perform a bone biopsy in patients with glomerular filtration rate (GFR) <30ml/min/1.73m2.8 Bone biopsy was considered necessary to rule out the presence of adynamic bone disease (ABD) or osteomalacia in which antiresorptive drugs would not be indicated. However, according to the new KDIGO 2017 guidelines (implemented by the American KDOQI) the measurement of bone mineral density (BMD) (guide 3.2.1) could come first, before the bone biopsy (guide 3.2.2)10,11 (Table 1). It is also stated that the absence of a bone biopsy should not preclude the use of antiresorptive therapies, at least in some patients10,11; therefore a nihilistic attitude while facing a major clinical problem should be avoided.1,2,4 In this second part of the review, and pending more specific prospective studies in CKD, we will examine the existing evidence on treatments aiming to increase BMD and prevent the risk of fractures, as well as the risk/benefit associated with the use of these drugs in CKD patients.
Comparison of KDIGO-CKD-MBD guidelines on bone mineral density (BMD) and osteoporosis (OP) in patients with chronic kidney disease (CKD).
| KDIGO 2009 | KDIGO 2017 | Reasoning and reflections |
|---|---|---|
| In patients with CKD stages 1–2 with OP and/or high risk of fracture, by criteria of the World Health Organization, we recommend management of OP similar to the general population (evidence 1A). In patients with CKD stage 3 with PTH in the normal range and OP and/or high risk of fracture, by criteria of the World Health Organization, we suggest similar treatment as in general population (evidence 2B) | In patients with CKD stages 1–2 with OP and/or high risk of fracture, by the criteria of the World Health Organization, we recommend a management similar to the general population (guide 4.3.1, evidence 1A). In patients with CKD stage 3a–3b with PTH in the normal range and OP and/or high risk of fracture, by criteria of the World Health Organization, we suggest treatment like in the general population (guide 4.3.2, evidence 2B) | Without changes |
| In patients with CKD stages 3–5D, with evidence of CKD-MBD, we suggest that the BMD should not be routinely measured because BMD does NOT predict the risk of fracture as in the general population and BMD does NOT predict the type of renal osteodystrophy (guide 3.2.2, evidence 2B) | In patients with CKD stages 3a–5D with evidence of CKD-MBD or risk factors of OP, the BMD should be measured to assess the risk of fracture if the resulting information could affect therapeutic decisions (guide 3.2.1, evidence 2B) | Multiple new prospective studies have documented that low BMD by DEXA predicts incident fractures in patients with CKD stages 3a–5D. The order of these recommendations (BMD vs. bone biopsy) has changed since the result of the measurement of BMD by DEXA could have an impact on the decision to perform a bone biopsy |
| In patients with CKD stages 3–5D it would be reasonable to perform a bone biopsy in several circumstances, including, but not limited to: unexplained fractures, persistent bone pain, unexplained hypercalcemia–hypophosphatemia, possible aluminum toxicity, and before bisphosphonate therapy in patients with CKD-MBD (guide 3.2.1, level of evidence not graduated) | In patients with CKD stage 3a–5D it is reasonable to perform a bone biopsy if knowledge of the type of renal osteodystrophy could affect therapeutic decisions (guide 3.2.2 level of evidence not graduated) | The primary motivation for this review was the growing experience on the use of OP drugs in patients with CKD, decreased BMD, and high risk of fracture. The inability to perform a bone biopsy may not justify delaying or ruling out or retaining antiresorptive therapy in patients with a high risk of fractures. It is commented that up to now the studies in patients with CKD have not definitively shown that bisphosphonates cause ABD and that the concerns in patients with CKD are more theoretical than based on the evidence. This fact is particularly relevant due to the aging of the general population, in which fragility fractures, reduction of GFR and decrease in BMD are all highly prevalent |
| In patients with CKD stage 3 with biochemical abnormalities of CKD-MBD, decreased BMD and/or fragility fractures, we suggest that treatment options should take into account the magnitude and reversibility of biochemical alterations and the progression of CKD, considering a Bone biopsy (guide 4.3.3, 2D evidence) | In patients with CKD stage 3a–5D with biochemical abnormalities of CKD-MBD and decreased BMD and/or fragility fractures, we suggest that treatment options should take into account the magnitude and reversibility of biochemical alterations and the progression of CKD, considering a bone biopsy (guide 4.3.3, evidence 2D) | The previous recommendations for bone biopsy before treatment with antiresorptive therapies or other treatments for OP should be extended from CKD stage 3 to CKD stages 3a–5D only if knowledge of the type of renal osteodystrophy could affect therapeutic decisions |
| In patients with CKD stage 4–5D with biochemical abnormalities of CKD-MBD and decreased BMD and/or fragility fractures, we suggest additional investigation with a bone biopsy before treatment with antiresorptive agents (guide 4.3.4, evidence 2C) | Idem |
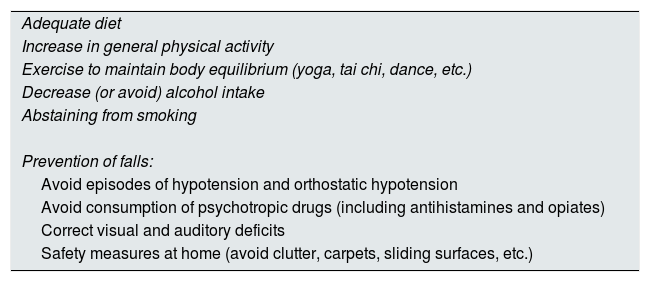
The ultimate goal in the treatment of OP is the prevention of fractures and their consequences.12 In 2017, it was published a Spanish consensus among different specialists, in which the absence of new fractures, the reduction of fracture risk (FRAX®) and the increase of BMD (T>−2.5 for column and T>−2.5/−2 for femoral neck) were considered appropriate objectives (“treat to target”).13 To this end, changes in lifestyle such as healthy dietary habits, increasing physical activity and exercise (yoga, tai chi, dancing, etc.), decreasing alcohol intake and smoking abstinence are considered important strategies (Table 2).14,15 It is also essential to adopt measures to prevent falls, mainly in the elderly, patients with cognitive and functional impairment, previous falls, orthostatic hypotension or consumption of psychotropic drugs (including antihistamines and opiates).12,14–16 OP and sarcopenia (osteosarcopenia) is a well-documented association in fragile patients.17 Other important actions are to correct visual and auditory deficits, as well as to adapt the physical environment.14,17–19 Approximately 30% of the population >65-year-olds suffer one fall per year, and 40% if they are >80-year-old. A 5% of these falls will cause a fracture.15 All these measures should also be implemented in patients with CKD.5
Non-pharmacological general measures in the treatment of patients with osteoporosis.
| Adequate diet |
| Increase in general physical activity |
| Exercise to maintain body equilibrium (yoga, tai chi, dance, etc.) |
| Decrease (or avoid) alcohol intake |
| Abstaining from smoking |
| Prevention of falls: |
| Avoid episodes of hypotension and orthostatic hypotension |
| Avoid consumption of psychotropic drugs (including antihistamines and opiates) |
| Correct visual and auditory deficits |
| Safety measures at home (avoid clutter, carpets, sliding surfaces, etc.) |
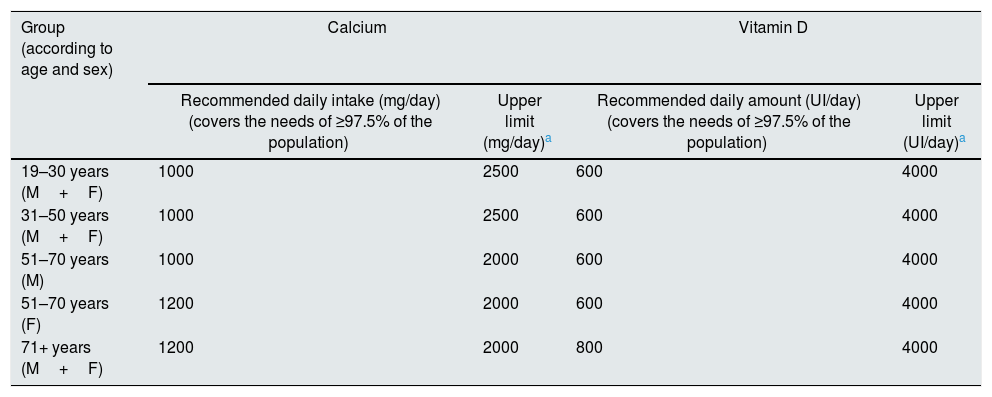
Clinical guidelines for the general population complementary supplementation of calcium and vitamin D in addition to the specific treatment of OP.18 Long term calcium deficiency may predispose to OP, but it is a mistake to believe that the loss of BMD related to age or menopause can be avoided simply with the supplementation of calcium.19–22 Furthermore, isolated calcium supplements (without vitamin D) may even increase the risk of hip fracture.22 Other negative effects associated with the indiscriminate use of Ca are the increased risk of nephrolithiasis, arrhythmias and cardiovascular risk, although these results are to some extent inconclusive or contradictory.1,5,14,19,21,23,24 The consumption of excessive amount of calcium in adults can be especially harmful in patients with CKD (or “hidden” CKD),10,25,26 especially in the presence of hypercalcemia, relative hypoparathyroidism (this is normal or low parathyroid hormone (PTH) in the presence of CKD), ABD, patients treated with warfarin and/or with cardiovascular calcifications.8,10 Therefore, a reasonable approach, as a first measure, is to encourage an appropriate intake of dietary calcium,27–29 prudent daily sun exposure and do not use routinely pharmacological supplementation of Ca10,14,18,25,26,28 or calcium-based calcium binders.10 The recommended Ca intake for the general population would be around 1000–1200mg/day28 (Table 3), depending on the patient and the age, but the dietary recommendations should take into account the abnormalities of mineral metabolism that are associated to the CKD stage.9,10,25,26
Recommended dietary intake for calcium and vitamin D in adults (by age and sex) of the general population.
| Group (according to age and sex) | Calcium | Vitamin D | ||
|---|---|---|---|---|
| Recommended daily intake (mg/day) (covers the needs of ≥97.5% of the population) | Upper limit (mg/day)a | Recommended daily amount (UI/day) (covers the needs of ≥97.5% of the population) | Upper limit (UI/day)a | |
| 19–30 years (M+F) | 1000 | 2500 | 600 | 4000 |
| 31–50 years (M+F) | 1000 | 2500 | 600 | 4000 |
| 51–70 years (M) | 1000 | 2000 | 600 | 4000 |
| 51–70 years (F) | 1200 | 2000 | 600 | 4000 |
| 71+ years (M+F) | 1200 | 2000 | 800 | 4000 |
F: females; IU: international units; M: males.
The upper limit indicates the level above which there is a risk of adverse events. It is not a a target of treatment, since there is no evidence of a greater benefit at levels higher than the recommended daily amount. The upper limit of calcium suggested for the general population far exceeds the capacity to be handled by a patient with CKD due to the decrease in glomerular filtration; thus, these maximum amounts should be avoided in CKD patients to avoid undesirable calcium accumulation.25,26 Therefore, we must also take into account dietary recommendations or limitations established for the management of mineral metabolism as a function of the stage of CKD.10,25,26,90
Source: Institute of Medicine (IOM).28 Adapted from Ross et al.28
Phosphate overload (that has direct and indirect effects on bone fragility)4 should also be avoided in patients with CKD, especially phosphate from processed foods which is easily absorbed.10 The use of calcium based phosphate binders has been associated with an increase in the progression of vascular calcifications,10,30 although it has not been definitively demonstrated that its restriction is associated with increased survival.31 Nevertheless recent prospective studies such as COSMOS,32,33 meta-analysis34,35 and the new KDIGO 201710 guidelines emphasize the need to restrict the Ca based P binders.
Vitamin D deficiency is very common in CKD patients but the administration of native vitamin D (i.e., cholecalciferol) in CKD is not clearly established.10,36,37 The current Spanish guidelines recommend the supplementation of native vitamin D if the serum level of calcidiol (25-OH vitamin D) is below the range of 20–30ng/ml.9,38,39 The recommended dose for the general population is 600–800IU/day28 (Table 3) and about 1000IU/day for patients with OP. Supplementation with native vitamin D, even in patients on dialysis, would improve bone mineralization, although with a limited effect on the control of PTH.4,22 These supplements (including calcifediol [calcidiol], frequently used in Spain) should be administered at low doses with frequent monitoring of calcium and phosphorus. It is also important to note that native vitamin D in daily dosing and in patients with vitamin D deficiency could modestly contribute to increase muscle strength and decrease the risk of falls.28,39–42 However, a recently published meta-analysis shows that there is no lower risk of fracture with the use of calcium, vitamin D or both in 51,145 non-institutionalized individuals from the general population >50-year.43 The results of this study are not applicable to patients with OP, with other metabolic diseases or those who take medications to protect bone, as recently highlighted by the American Society for Bone and Mineral Research.43
Thus, multiple studies show that inadequate response to medication for OP is more frequent in patients with calcidiol levels <20–30ng/ml,44,45 and that the correction of vitamin D deficiency is necessary to prevent not infrequent cases of osteomalacia46 (e.g., in patients with low serum levels of calcium, calcidiol and/or phosphate that frequently have disproportionately high alkaline phosphatase, with significant bone pain or multiple fractures).4,46,47
Finally, in addition to PHOSPAHTE restriction, the treatment of secondary hyperparathyroidism and/or high-turnover ROD classically includes active vitamin D metabolites (e.g., calcitriol, paricalcitol)±calcimimetics (in dialysis patients). However, there is still some debate about their appropriate use in patients with CKD.10,11,36,37 Vitamin D derivatives are the only drugs specifically indicated for the control of secondary hyperparathyroidism before the onset of dialysis48,49; they have been associated with an increase in survival50,51 and it is suggested that they should be used judiciously to avoid hypercalcemia, hyperphosphatemia or excessive suppression of PTH.9,52,53
The use of cholecalciferol, ergocalciferol, calcifediol, alfacalcidol and/or calcitriol could be effective (although not fully demonstrated), together with bisphosphonates, in patients with prolonged exposure to corticosteroids.14,54
Antiresorptive drugs for the treatment of osteoporosisBisphosphonatesBisphosphonates are structural analogues of inorganic pyrophosphate, which modulates bone remodeling55 (Table 4). Bisphosphonates have a high affinity for bone because it binds to hydroxyapatite crystals (with a variable half-life in the skeleton that could be up to 10 years).55,56 Bisphosphonates reduce the rate of bone resorption by inhibiting the activity of osteoclasts and, through different mechanisms, induce apoptosis of all bone cells.55,57
Comparison of antiresorptive and anabolic agents for the treatment of osteoporosis in patients with chronic kidney disease.
| General description | Potential benefits |
|---|---|
| Antiresorptive agents | |
| Bisphosphonates | |
| Structure P–C–P, similar to P–O–P of native pyrophosphate (analog of inorganic pyrophosphate) | Cheap and easily available all over the world |
| It accumulates in bone independently of renal function, but if renal clearance is reduced bone deposit increases due to prolongation of its half-life. | Increase in BMD and it decreases fractures in patients with CKD before dialysis in “post hoc” analysis. A high risk of bias |
| Since it is bound to the bone a residual effect remains after withdrawal (advantage and inconvenience). In fact, “therapeutic holidays” are advised after a period of treatment | Potential attenuation of the progression of vascular calcification (benefits described in calciphylaxis) |
| Potential risk of ABD and systemic toxicity | |
| Not recommended in fertile, sexually active women, without effective contraceptive control. | |
| Potential reduction of intestinal absorption (low bioavailability) and interactions with other drugs (phosphate binders, calcium, among others) | |
| Denosumab | |
| Anti-RANKL monoclonal antibody that produces inhibition of OPG/RANK/RANKL pathway | No renal clearance |
| Higher price | Large increase in BMD after short periods of treatment |
| Potential risk of ABD | Increase in BMD and decrease in fractures in patients with CKD before dialysis in post hoc analysis, but with a high risk of bias |
| Hypocalcemia and rebound hyperparathyroidism; need monitoring in advanced CKD | Minor renal side effects and rarely associated with atypical fractures |
| Not recommended in fertile, sexually active women, without effective contraceptive control | Shorter half-life than bisphosphonates and the effects are reversible, but would require indefinite therapy (or sequential therapy), switching to a SERM (women) or lower doses of oral bisphosphonates. |
| Inadequate data on infections in immunosuppressed patients (e.g., urinary tract infections, skin infections), although a higher incidence of opportunistic infections has not been reported | |
| Subcutaneous injection every 6 months | |
| Anabolic agents | |
| Teriparatide | |
| Recombinant human 1–34 N-terminal PTH sequence | No renal clearance |
| Risk of hypercalcemia | Increase in bone mass and turnover, no risk of ABD; in fact, it is a potential indication for ABD |
| Very expensive (4 fold increase in price during the last decade) and the use is limited to 2 years due to the risk of osteosarcoma | Increase in BMD and decrease in fractures in patients with CKD before dialysis in post hoc analysis, but with a high risk of bias |
| Daily subcutaneous injection | |
| Romosozumab | |
| Monoclonal antibody against sclerostin | No renal clearance |
| Trials still in phase III in the general population | Large increase in BMD after short periods of treatment |
| Potential not well defined undesirable cardiovascular effects | Increase in bone mass and turnover, no risk of ABD; in fact, it could be a potential indication for the ABD |
| Not approved by the FDA | |
Bisphosphonates are drugs of first choice in the current treatment of all types of OP. This is based on years of clinical experience, multiple indications in different types of metabolic bone disorders and their low cost.58–61 The difficulty of absorption in the oral presentations (alendronate, risedronate) and the risk of esophagitis make it necessary to take it on an empty stomach, with water, in an upright position and to wait 30min before any additional oral intake. In the KDIGO 2009 guidelines (Table 1) it was suggested that patients with CKD stages 1–2 with OP and/or high risk of fracture, and CKD stage-3 with PTH in the normal range should be followed the same treatment as in the general population.18 In fact, patients with CKD stage 3 usually have few identifiable abnormalities of mineral metabolism, sharing the same risk factors as the general population.62 Alternatively, in patients with CKD stages 1–3 with biochemical abnormalities of CKD-MBD and decreased BMD and/or fragility fractures, it was suggested that there were other factors to be considered in order to decide treatments8 (Table 1). Finally, in CKD stages 4–5D, it was suggested additional evaluation including bone biopsy before administration of antiresorptive therapy.8
Today, we know that with the deterioration of kidney function there is an increase in the prevalence of OP,63 especially in CKD stages 4–5D. Other factors (ROD, metabolic acidosis, vitamin D deficiency, excess of FGF23, hyperparathyroidism, skeletal resistance to PTH, etc.) complicate the diagnosis of OP based on BMD. Although bone biopsy is the only method to exclude other abnormalities of advanced CKD, there is a growing consensus that basing OP treatments on the need for a bone biopsy could impermissibly limit treatment in patients who have a very high risk of fracture. Bisphosphonates seem to prevent the loss of BMD in CKD64–66 but it has not been proven to be effective in reducing the risk of fractures; this is why it is recommended a prudent and individualized (risk/benefit) use of bisphosphonates.2,62,67
Guidelines for the use of bisphosphonates in the general population (applicable to patients with mild CKD without significant alterations of the mineral metabolism)5,14 propose to initiate treatment with oral bisphosphonates in the situations such as those indicated in Table 5. Also, in the general population it is indicated to re-evaluate the fracture risk by BMD 2 or 3 years after the initiation of treatment. In a recent consensus14 it is being considered FRAX®+BMD together as appropriate objectives. Patients who are receiving bisphosphonates and who are no longer at a high risk of fracture are potential candidates for “drug holiday”.13,14,68 Conversely, in patients with a BMD with T<−2.5 in the femoral neck, patients with history of fractures and with T<−2.0 in the femoral neck, or family history of fragility fractures, treatment with oral bisphosphonates could be extended up to 10 years, since the benefit would probably be greater than the associated risks.14,68 If after this period of time the risk persists, it would be indicated the transition to another drug (sequential therapy).14
Indications for the use of bisphosphonates in the general population in different guidelines, possibly applicable to CKD patients without significant alterations in mineral metabolism and with little risk of adynamic bone disease.a
| a) Patients with history of hip or vertebral fracture |
| b) Patients with a BMD (T-score) ≤−2.5 SD in the hip or spine (measured for any reason). |
| c) BMD in the range of osteopenia (T-score) between −1.0 and −2.5 SD, especially if ≤−2.0 and at least two factors associated with a high risk of fracture, part I)20,118 |
| d) Patients with osteopenia and with 10-year probability of hip fracture greater than 3% or a 10-year probability of osteoporotic fracture greater than 7.5–20% (depending on countries and based on FRAX®)11,12,20,37 |
| e) In a recent study, patients with a very high risk of fracture were considered those with T≤2.5 and one or more moderate or severe vertebral fractures; or a T≤2.0 and two or more moderate or severe vertebral fractures, or a fracture of the proximal femur130 |
It is known that patients at risk of ABD are primarily those in peritoneal dialysis, diabetes, older or malnourished which is the presence of relative hypoparathyroidism (low levels of PTH or relatively low than expected for degree of CKD).52 In dialysis patients these levels have undoubtedly been established in intact PTH values <2 times the upper limit of normality for the assay used. Moreover, the combination of intact PTH and alkaline phosphatase (especially the bone fraction) provides greater predictive power for the differential diagnosis of high or low turnover bone disease (e.g., PTH<200 pg/ml and bone alkaline phosphatase <20ng/ml).4,47,52 In these patients it would be indicated the use of antiresorptive agents and should be evaluated the possibility of a bone biopsy before initiation of treatment (or to indicate an anabolic treatment); the strategy should be similar if osteomalacia is suspected (mentioned in the text) as well as possible poisoning by aluminum or other metals.
The reason for these limitations in the length of treatment are fundamentally linked to two adverse effects: osteonecrosis of the jaw (ONJ) and atypical fractures of the femur (subtrochanteric-diaphyseal). In addition to an individual predisposition, they have been associated with comorbidity (mainly neoplastic), use of intravenous route (i.e., zoledronate) or high doses, prolonged exposure or co-administration with glucocorticoids.68–70 The risk of ONJ is estimated at 1/10,000 and <1/100,000patients-year,14,15,69 and is also associated to poor oral hygiene, history of dental procedures and the use of dental prosthesis.55 The risk of atypical fractures of the femur seems to be more associated with an individual predisposition in patients with OP than with the treatment itself since there is lack of association of atypical fractures with cumulative doses.14,70,71 In the general population, it has been estimated that for every atypical fracture that occurred in a treated patient, there would have been prevented 50–100 hip fractures and hundreds of vertebral and non-vertebral fractures with the consequent reduction in mortality.14,15
Finally, the inhibition of osteoclastic activity induced by bisphosphonates has raised questions about the possibility of generating an “adynamic bone” due to excessive suppression of bone remodeling and, therefore, reduced capacity for microfracture repair and greater skeletal fragility.55,72,73 At least in the general population, it has been shown that the benefit of reducing fractures outweighs the potential risk.68 However, in dogs treated with high doses of bisphosphonates, it has been observed an increase in microfractures,74 and a recent study showed less porosity but more microfractures in the fractured bones of patients treated with bisphosphonates compared with patients with untreated fractures or healthy controls.75 However, iliac crest biopsies performed after 5–10 years of treatment do not seem to show oversuppression of bone remodeling76–78 and, in other studies, an increase in microfractures has not been detected.79,80 Although not constant, the positive (although not constant) effect of anabolic teriparatide in some patients with atypical femoral fractures, previously treated with bisphosphonates, merits consideration. Therefore, the optimal duration of bisphosphonate therapy should be individualized according to the risk factors of the patient, and although the risk seems to be low even in treatments up to 10 years,68,77 the risk/benefit of the extended use remains to be assessed in low-risk patients or patients with CKD.5,81
With regard to the use of bisphosphonates in CKD, it is well known the contraindication of intravenous bisphosphonates with creatinine clearances below 30ml/min since they can cause various types of kidney damage.82,83 However, in a post hoc analysis of clinical trials with oral alendronate and risedronate including patients with decreased GFR (CKD stages 3–4) for a maximum of 3 years, there were no differences in the occurrence of renal adverse effects.64,65 Since bisphosphonates can potentially accumulate in the bone of patients with advanced CKD84,85 (Table 4), the KDIGO 2009 suggested to perform a bone biopsy prior to therapy with bisphosphonates before its use in CKD 4–5 (Table 1).8 As discussed in the KDIGO 2017, this claim was based on a cross-sectional study of 13 patients with CKD stages 2–4 who underwent a bone biopsy after a variable period of treatment with bisphosphonates (4–60 months), all of them being diagnosed of ABD.84 In addition, Coco et al.86 showed that 6/6 patients with functioning renal transplant treated with intravenous pamidronate (with a frequency of administration much higher than usual) had ABD vs 3/8 in the controls, although the pretransplant bone status was not known. Only 14/72 patients were biopsied, so it is difficult to extrapolate these data. Currently, the prevalence of ABD is increasing,52,84,87 and it could even precede the high-turnover disease during the evolution of CKD.88,89 Aging, diabetes, calcium overload, malnutrition, inflammation and relative hypoparathyroidism (low or relatively low PTH levels) are risk factors for ABD that should be taken into consideration before the indication of bisphosphonates.52,84,90 In fact, all of them have warnings or contraindications regarding their use in patients with CKD with creatinine clearances <30–35ml/min).
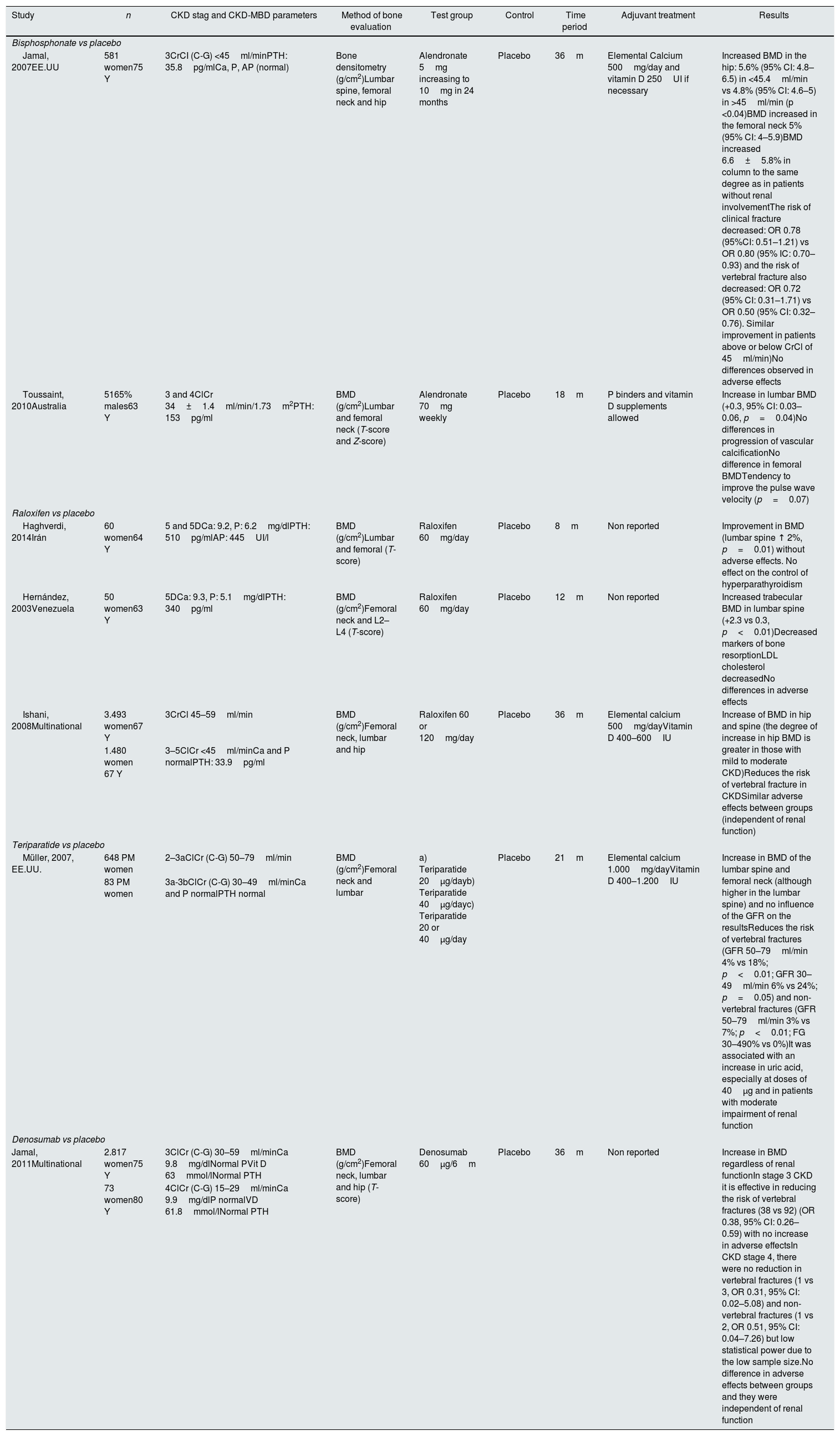
Since the publication KDIGO 2009 guidelines.8 several studies have shown that BMD does predict the risk of fracture in patients with CKD.91–94 Other post hoc analysis of large randomized trials for treatment of postmenopausal OP with alendronate and risedronate have described that, in CKD patients (most of them women in stages 3–4), these drugs improve BMD and reduce the risk of fractures64,65 (Table 6). Therefore, at least in the absence of significant abnormalities in mineral bone metabolism, the use of bisphosphonates and other drugs approved for the treatment of OP could be appropriate in patients with “normal” creatinine levels and a decreased GFR.2,10,11,64,65 Thus, the update of the KDIGO guidelines in 201710 (Table 1) suggests that the need for a previous bone biopsy before deciding treatment is not mandatory in patients with advanced CKD. It is considered that there is not convincing evidence that bisphosphonates cause ABD, and that the accumulation of data after the use of antiresorptive drugs would potentially allow us their use without a bone biopsy is necessary.10 Therefore, the “difficulty” to obtain histomorphometric diagnosis of the type bone disease does not justify therapeutic nihilism in patients with a high risk of fracture.10 However, beyond the guidelines, we must also recognize that other analyses highlight the fact that antiresorptive treatment does not consistently demonstrate additional beneficial effects beside an improvement in BMD, and there is no absolute evidence on a reduction of fracture risk or vascular calcification67 (Table 6). This last issue is important given the important relationship between bone and vessels and its potential additional beneficial effect.95–97 Experimental work and small clinical studies in dialysis patients, suggest a beneficial effect of some bisphosphonates on decreasing the progression of vascular calcifications and in the treatment of calciphylaxis.98–100
Clinical studies.
| Study | n | CKD stag and CKD-MBD parameters | Method of bone evaluation | Test group | Control | Time period | Adjuvant treatment | Results |
|---|---|---|---|---|---|---|---|---|
| Bisphosphonate vs placebo | ||||||||
| Jamal, 2007EE.UU | 581 women75 Y | 3CrCI (C-G) <45ml/minPTH: 35.8pg/mlCa, P, AP (normal) | Bone densitometry (g/cm2)Lumbar spine, femoral neck and hip | Alendronate 5mg increasing to 10mg in 24 months | Placebo | 36m | Elemental Calcium 500mg/day and vitamin D 250UI if necessary | Increased BMD in the hip: 5.6% (95% CI: 4.8–6.5) in <45.4ml/min vs 4.8% (95% CI: 4.6–5) in >45ml/min (p <0.04)BMD increased in the femoral neck 5% (95% CI: 4–5.9)BMD increased 6.6±5.8% in column to the same degree as in patients without renal involvementThe risk of clinical fracture decreased: OR 0.78 (95%CI: 0.51–1.21) vs OR 0.80 (95% IC: 0.70–0.93) and the risk of vertebral fracture also decreased: OR 0.72 (95% CI: 0.31–1.71) vs OR 0.50 (95% CI: 0.32–0.76). Similar improvement in patients above or below CrCl of 45ml/min)No differences observed in adverse effects |
| Toussaint, 2010Australia | 5165% males63 Y | 3 and 4ClCr 34±1.4ml/min/1.73m2PTH: 153pg/ml | BMD (g/cm2)Lumbar and femoral neck (T-score and Z-score) | Alendronate 70mg weekly | Placebo | 18m | P binders and vitamin D supplements allowed | Increase in lumbar BMD (+0.3, 95% CI: 0.03–0.06, p=0.04)No differences in progression of vascular calcificationNo difference in femoral BMDTendency to improve the pulse wave velocity (p=0.07) |
| Raloxifen vs placebo | ||||||||
| Haghverdi, 2014Irán | 60 women64 Y | 5 and 5DCa: 9.2, P: 6.2mg/dlPTH: 510pg/mlAP: 445UI/l | BMD (g/cm2)Lumbar and femoral (T-score) | Raloxifen 60mg/day | Placebo | 8m | Non reported | Improvement in BMD (lumbar spine ↑ 2%, p=0.01) without adverse effects. No effect on the control of hyperparathyroidism |
| Hernández, 2003Venezuela | 50 women63 Y | 5DCa: 9.3, P: 5.1mg/dlPTH: 340pg/ml | BMD (g/cm2)Femoral neck and L2–L4 (T-score) | Raloxifen 60mg/day | Placebo | 12m | Non reported | Increased trabecular BMD in lumbar spine (+2.3 vs 0.3, p<0.01)Decreased markers of bone resorptionLDL cholesterol decreasedNo differences in adverse effects |
| Ishani, 2008Multinational | 3.493 women67 Y | 3CrCl 45–59ml/min | BMD (g/cm2)Femoral neck, lumbar and hip | Raloxifen 60 or 120mg/day | Placebo | 36m | Elemental calcium 500mg/dayVitamin D 400–600IU | Increase of BMD in hip and spine (the degree of increase in hip BMD is greater in those with mild to moderate CKD)Reduces the risk of vertebral fracture in CKDSimilar adverse effects between groups (independent of renal function) |
| 1.480 women 67 Y | 3–5ClCr <45ml/minCa and P normalPTH: 33.9pg/ml | |||||||
| Teriparatide vs placebo | ||||||||
| Müller, 2007, EE.UU. | 648 PM women | 2–3aClCr (C-G) 50–79ml/min | BMD (g/cm2)Femoral neck and lumbar | a) Teriparatide 20μg/dayb) Teriparatide 40μg/dayc) Teriparatide 20 or 40μg/day | Placebo | 21m | Elemental calcium 1.000mg/dayVitamin D 400–1.200IU | Increase in BMD of the lumbar spine and femoral neck (although higher in the lumbar spine) and no influence of the GFR on the resultsReduces the risk of vertebral fractures (GFR 50–79ml/min 4% vs 18%; p<0.01; GFR 30–49ml/min 6% vs 24%; p=0.05) and non-vertebral fractures (GFR 50–79ml/min 3% vs 7%; p<0.01; FG 30–490% vs 0%)It was associated with an increase in uric acid, especially at doses of 40μg and in patients with moderate impairment of renal function |
| 83 PM women | 3a-3bClCr (C-G) 30–49ml/minCa and P normalPTH normal | |||||||
| Denosumab vs placebo | ||||||||
| Jamal, 2011Multinational | 2.817 women75 Y | 3ClCr (C-G) 30–59ml/minCa 9.8mg/dlNormal PVit D 63mmol/lNormal PTH | BMD (g/cm2)Femoral neck, lumbar and hip (T-score) | Denosumab 60μg/6m | Placebo | 36m | Non reported | Increase in BMD regardless of renal functionIn stage 3 CKD it is effective in reducing the risk of vertebral fractures (38 vs 92) (OR 0.38, 95% CI: 0.26–0.59) with no increase in adverse effectsIn CKD stage 4, there were no reduction in vertebral fractures (1 vs 3, OR 0.31, 95% CI: 0.02–5.08) and non-vertebral fractures (1 vs 2, OR 0.51, 95% CI: 0.04–7.26) but low statistical power due to the low sample size.No difference in adverse effects between groups and they were independent of renal function |
| 73 women80 Y | 4ClCr (C-G) 15–29ml/minCa 9.9mg/dlP normalVD 61.8mmol/lNormal PTH | |||||||
Adapted from KDIGO 2017.10
Denosumab (DMab) is a monoclonal antibody that acts by blocking the ligand receptor of nuclear factor kappa-B (RANKL) and as a consequence inhibits osteoclastogenesis101,102 (Table 4). DMab is useful in the prevention of vertebral, non-vertebral and hip fractures in the general population.101,103,104 The metabolism or excretion of DMab does not depend on renal function and it does not appear to alter renal function, so there are neither dosage adjustments needed nor use restrictions in patients with CKD and/or decreased GFR.14,105 DMab has rarely been associated with atypical fractures. The effect of the drug ends upon cessation of its administration.14
In the post hoc analysis of osteoporotic women with CKD stage 3 (n=2817) and 4 (n=73) treated with DMab, it has been shown that after 36 months, as compared with placebo, there was an increase in BMD and reduction of the risk of fracture, independently of renal function and without an effect on serum creatinine and no increase in adverse effects105 (Table 4). However, some studies have shown that DMab may induce hypocalcemia, especially in patients with CKD and in hemodialysis patients with underlying high bone turnover.106–109 This potential effect is important and occasionally severe,110,111 especially during the first and second weeks of treatment, with special attention being paid to patients at risk or who are receiving concomitantly cinacalcet112 (also possible with etelcalcetide). If DMab is considered indicated by the presence of a high risk of fracture, the patient should be informed of the symptoms of hypocalcemia, monitor plasma calcium more frequently and perform a more intense, temporary replacement of calcium and vitamin D (native and/or calcitriol).106,107
Rebound hypercalcemia have also been described after long periods of treatment with DMab; this is attributed to an increase in osteoclastic activity after its suppression, but also to the previous administration of calcium-vitamin-D.108 The administration of DMab does not seem to affect the progression of aortic calcification and cardiovascular events, as compared with placebo, with occasional exceptions.113,114 In hemodialysis patients treated with DMab a relatively safe treatment of hypocalcemia is to modify calcium in the dialysis bath (usual 3mEq/l [1.5mmol/l],110 since each session would produce a positive calcium balance. Despite the concomitant administration of vitamin D, DMab may produce a reversible increase in intact PTH with values greater than 1000pg/ml.110 In any case, after the interruption of the treatment there may be a rapid bone loss so a sequential therapy with another drug should be evaluated to sustain the benefit obtained in the BMD.14,18
Several studies have shown beneficial effects of DMab in dialysis patients. In a prospective pilot study of 12 patients, all of them with PTH >1000pg/ml, T-score <−1.0 and bone pain, not candidates for surgery, Chen et al.115 described the effects of DMab (off-label), calcitriol, phosphate binders and a calcium bath adjusted according to the biochemical data. After 6 months of treatment the BMD increased in the femoral neck and in the lumbar spine and there was a reduction in pain. In the first month, the majority of patients experienced an increase in intact PTH that rapidly decreased at the end of the study after increasing the dose of calcitriol (1702±182 to 519±127pg/ml).115 A longer retrospective experience110 describes 12 hemodialysis patients with osteoporosis who received DMab at usual doses. After 24 months of follow-up, they also observed improvement in bone metabolism parameters and T-score, although the latest was only measured by phalangeal ultrasound.
In summary, according to the current knowledge, antiresorptive agents such as bisphosphonates or DMab could be used in patients with different stages of CKD (especially CKD 1–3) at least if they have fragility fractures and/or high risk of fracture2,116 This is similar to what is being done in the general population. Bone biopsy may not be necessary if after the individualized evaluation the presence of an ABD is considered unlikely. Bisphosphonates may be indicated in these patients, especially if they have high bone turnover parameters62 (significant elevation of serum levels of PTH and alkaline phosphatases). It may be convenient to space the doses and/or limit the duration of treatment.62,117 The use of DMab could be extended to more advanced stages of CKD (stages 4 or even 5), with special control of the serum calcium concentration. Clinical trials (i.e., with DMab or alendronate in advanced CKD and dialysis [NCT01464931, NCT02792413, NCT02440581]) could provide relevant information in the upcoming years. Until then, a valid option is to adopt diagnostic-therapeutic algorithms based on fracture risk and not to wait for absolute evidence.4,116,118
Anabolic drugs for the treatment of osteoporosisTeriparatideTeriparatide (Table 4) is approved as an osteoforming (anabolic) therapy for postmenopausal and steroid induced OP, and in men with high risk of fracture (e.g., two or more vertebral fractures).14,19,119 Teriparatide induces an intermittent exposure to PTH which increases bone formation particularly in trabecular bone. An important limitation is the high cost (the most expensive alternative) and after removing teriparatide there is gradual decrease in bone mass which can be mitigated by continuing the therapy with a bisphosphonate.13,120 Another limitation is that it cannot be administered for periods longer than 24 months (Table 4).
Compared to placebo, teriparatide produces a significant increase in BMD of the lumbar spine and femoral neck and there is no evidence that this increase in BMD is modified by CKD121 (Table 6). Although its use is restricted in moderate CKD and contraindicated in severe CKD, in a recent post hoc analysis in Japanese women with OP, CKD stages 4–5 and high risk of fracture (82% had a previous fracture), it was observed that subcutaneous teriparatide 20μg/day during 24 months appeared to be effective (increasing BMD and biomarkers).122 It should be emphasized that in some cases with ABD the use of teriparatide resulted in an increase in bone turnover in patients with ABD confirmed by bone biopsy.52,123,124 So far there is no experience with abaloparatide or the human recombinant PTH Natpara® in patients with CKD.125 In Japanese patients on hemodialysis with hypoparathyroidism and low BMD the use of 56.5μg of teriparatide once a week resulted in an increase in lumbar BMD, although 10/22 patients had to abandon treatment due to side effects.126
It should be taken into consideration that in patients on dialysis with decreased PTH (<2 times the upper limit of normality, and especially if they have a history of fracture) there is a possibility of decreasing calcium in the dialysis fluid to stimulate endogenous PTH production and improve bone remodeling.4,52 Finally, it should be noted that a clinical trial an ongoing clinical trial in patients with OP on dialysis assigned to the arm of low bone turnover a teriparatide–cinacalcet combination (NCT02440581), perhaps to stimulate the endogenous production of PTH by the hypocalcemia induced by cinacalcet.
RomosozumabRomosozumab (RMab) (Table 4) is a humanized monoclonal antibody against sclerostin, an inhibitor of the Wnt pathway a key signaling system responsible for bone formation. The sclerostin produced by the osteocytes binds to the proteins LRP (4-5-6), the ligand receptors of the Wnt pathway. RMab neutralizes the effect of sclerostin resulting in enhanced Wnt activity which stimulates bone formation and inhibits bone resorption (unlike classical osteoanabolic agents).127,128 Clinical studies have shown that RMab produces a significant improvement of spine and hip BMD.127,129,130 A recent study in postmenopausal women with a very high risk of fracture showed that sequential treatment with monthly RMab during 12 months followed by weekly alendronate resulted in a lower risk of fracture than weekly treatment with alendronate alone.130 However, a greater number of some cardiovascular events were attributed to the RMab group during the first year of treatment (2.5% vs 1.9%, respectively), although there were no differences between RMab and placebo.128–130 For this reason, the FDA has held its commercialization pending new studies and reanalyses. The role of this drug in patients with CKD is not sufficiently known to advise its use.131
Other treatmentsEstrogens and raloxifeneHypoestrogenism (or estrogen deficiency) is a well-known cause of OP. Both adequate estrogen therapy and the use of selective modulators of selective estrogen receptor modulators (SERM) have been shown to improve postmenopausal OP.19 Early menopause (or premature hypogonadism) is more frequent in women with CKD,132 so these patients represent a particularly high-risk population to develop postmenopausal OP.
Raloxifene is a SERM without the carcinogenic risk of classical estrogen therapy (it is even described as a protector of breast cancer) and it is an alternative therapy in postmenopausal OP.133–135 Raloxifene improves BMD and decrease the risk of vertebral fractures but not hip fractures.133,136 In a post hoc analysis the same effect was observed on vertebral fractures in women with creatinine clearance >20ml/min. Other studies with few patients have reported that raloxifene increases BMD and reduces the loss of bone mass in the spine, hip, and radius and reduces the risk of vertebral fracture in patients with CKD (Table 6).135,137
It is important to consider that raloxifene could play an interesting role in sequential therapies for women with OP.14,15 The most frequent side effects are hot flashes and cramps; venous thrombosis is the most important adverse effect. Therefore, it should not be used in patients with climacteric symptoms or risk of thromboembolism. There is no experience with bazedoxifene, a third generation SERM, in patients with CKD.
Cinacalcet and parathyroidectomyBesides the beneficial effect of cinacalcet on ROD,138 a pre-specified secondary analysis of the EVOLVE study evaluated the appearance of clinical fractures in dialysis patients with secondary hyperparathyroidism.7 After several statistical adjustments, the relative risk of fracture was slightly lower with cinacalcet (0.83, IC 95%: 0.72–0.98) and, using another prespecified analysis (lag-censoring analysis), the relative risk of fracture with cinacalcet was 0.72 (0.58–0.90).7 Cinacalcet is not effective in treating the decrease in BMD in primary hyperparathyroidism.
If cinacalcet would represent the theoretical possibility of “chemical parathyroidectomy”, it has also been described that surgical parathyroidectomy decreases bone turnover, improves BMD and reduces the risk of fracture in patients on dialysis,4,139,140 but in these studies there are numerous biases in the surgical indication and the intervention is not free of risks.141
CalciliticsThere are still no calcium-sensor-receptor inhibitors in the market (unlike agonists such as cinacalcet).142 In the future, these drugs could represent an indirect way to increase the endogenous production of PTH in patients with ABD.
OthersHyponatremia and metabolic acidosis are associated with OP, so it would be advisable to avoid them. Different experimental studies and preliminary clinical data have shown controversial and variable bone effects after inhibition of the renin–angiotensin system or with the use of other drugs of interest among nephrologist such as beta-blockers, diuretics, statins, oral antidiabetics, immunosuppressants or omeprazole.143
ConclusionIn the publication of the first part of this review1 it was mentioned that the new guidelines suggest, with some ambiguity, to assess the risk of fracture (e.g., BMD) whenever this evaluation could affect therapeutic decisions. Although the effect of different drugs on BMD in the general population cannot be equated in terms of efficacy to patients with CKD, in this second part of the review on OP in CKD we have emphasized that in recent years there are results suggesting that the drugs used to manage OP in the general population could be used in CKD after an individualized analysis of risk/benefit of these patients.
Consequently, in patients with CKD stages 1–3, without evident (significant) biochemical alterations, the prevention of fractures should not differ from the protocols for the general population. It is recommended an adequate content of calcium in the diet and the use of vitamin D (e.g., cholecalciferol, calcifediol), according to the levels of calcidiol. Antiresorptive agents (bisphosphonates or DMab) could be used safely and effectively without the mandatory need of bone biopsy. Antiresorptive agents could also be used in selected patients with more advanced stages of CKD (Table 5) or at least in patients with previous clinical or morphometric fractures (a clinical proof of bone fragility) and/or very high risk of fracture, provided that the presence of ABD is considered unlikely (Table 5). DMab, which is not eliminated by the kidneys, would be a safe alternative in overt CKD but its use requires an adequate control of the serum calcium level and repletion of vitamin D. Teriparatide would be safe and potentially effective for a maximum of 24 months in parathyroidectomized patients and/or with high suspicion of ABD. Finally, raloxifene could be considered in postmenopausal patients with CKD that show low risk of thromboembolism or major climacteric symptoms. The treatment with estrogens should be limited to early menopause, for a limited time and with indication by a gynecologist. However, there is no doubt that there is a need to include patients with CKD (with and without CKD-MBD) in future clinical trials. This will help to determine if the use of these treatments can be widely extended to CKD, given that the majority of studies carried out so far have not been consistent, there are important biases and they have a low degree of evidence.67,85,116,144
FundingThis work has not had specific financial support.
Conflicts of interestNone for this review.
This review includes authors who belong to the RedinRen National Network (RD06/0016/0001 and RD12/0021/0033), the Spanish National Biobank Network (RD09/0076/00064) and the Catalan Research Group AGAUR (2009 SGR-1116), as well as collaborators of the Iñigo Alvarez de Toledo Foundation (FRIAT). We would also like to thank Dr. Lucia Bailone for her outstanding contribution to the preparation of this article and Mr. Ricardo Pellejero for his important work in bibliographical assistance.
Please cite this article as: Bover J, Ureña-Torres P, Laiz Alonso AM, Torregrosa J-V, Rodríguez-García M, Castro-Alonso C, et al. Osteoporosis, densidad mineral ósea y complejo CKD-MBD (II): implicaciones terapéuticas. Nefrologia. 2019;39:227–242.