Peritoneal dialysis (PD) is a method of renal replacement therapy (RRT) used for more than 50 years. It uses the peritoneal membrane to remove solutes, nitrogenous waste products and ultrafiltration.1 It is considered an easy-to-use therapy, without many complications. Its use is well suited for most patients and some authors consider that PD is the method of choice in the pediatric population.2
PD allows autonomy, flexibility and a better quality of life as compared to hemodialysis (HD).1 Mendes-Durán states that it is used in some countries such as Mexico by more than 56% of patients that need RRT.3 Patients with chronic kidney disease (CKD) have a high prevalence of comorbidities, poor health-related quality of life, and functional dependence.4
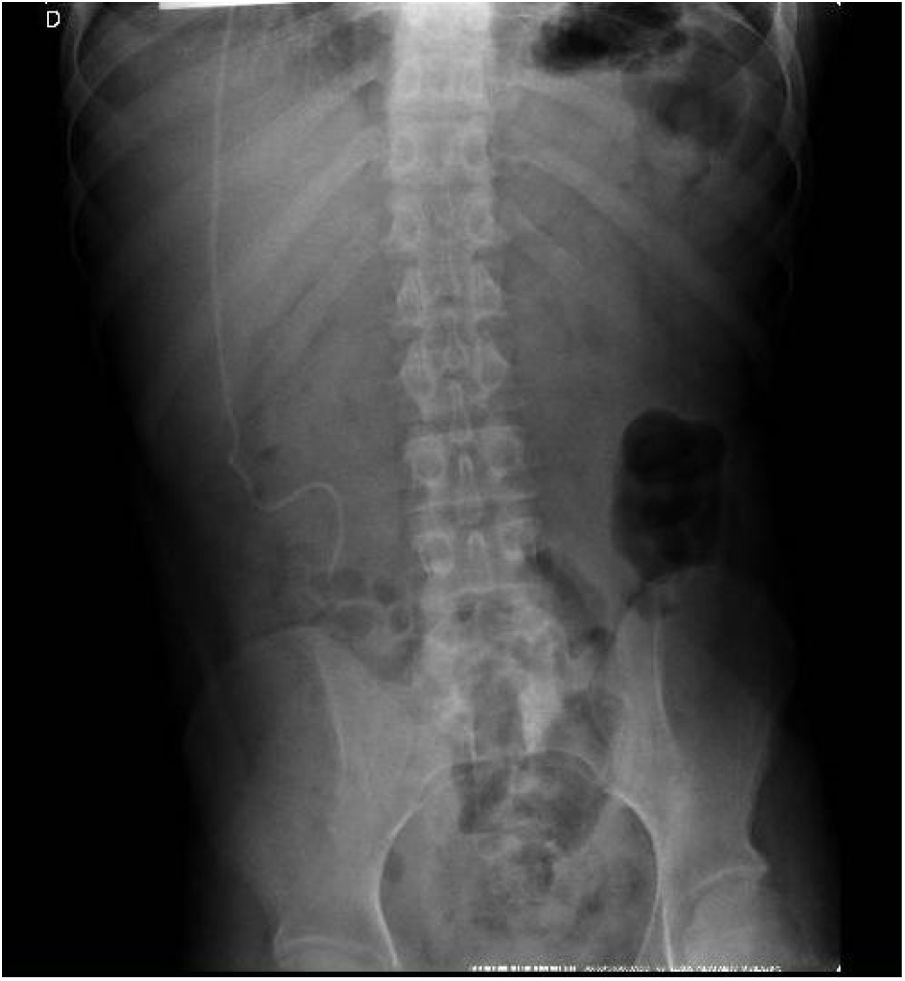
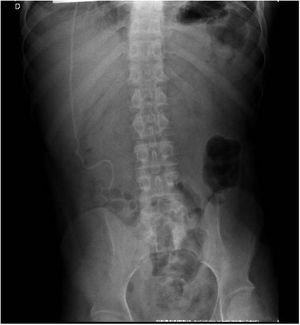
We report the experience of a 20-year-old patient, with myelomeningocele and hydrocephalus at birth, who underwent surgery for implantation of ventriculoperitoneal shunt (DVP) (Fig. 1). He presented with neurogenic bladder and bilateral hydronephrosis, multiple episodes of urinary tract infection, and urethral stricture due to prolonged use of an indwelling urinary catheter. He finally developed CKD and started RRT (hemodialysis) at the age of 15.
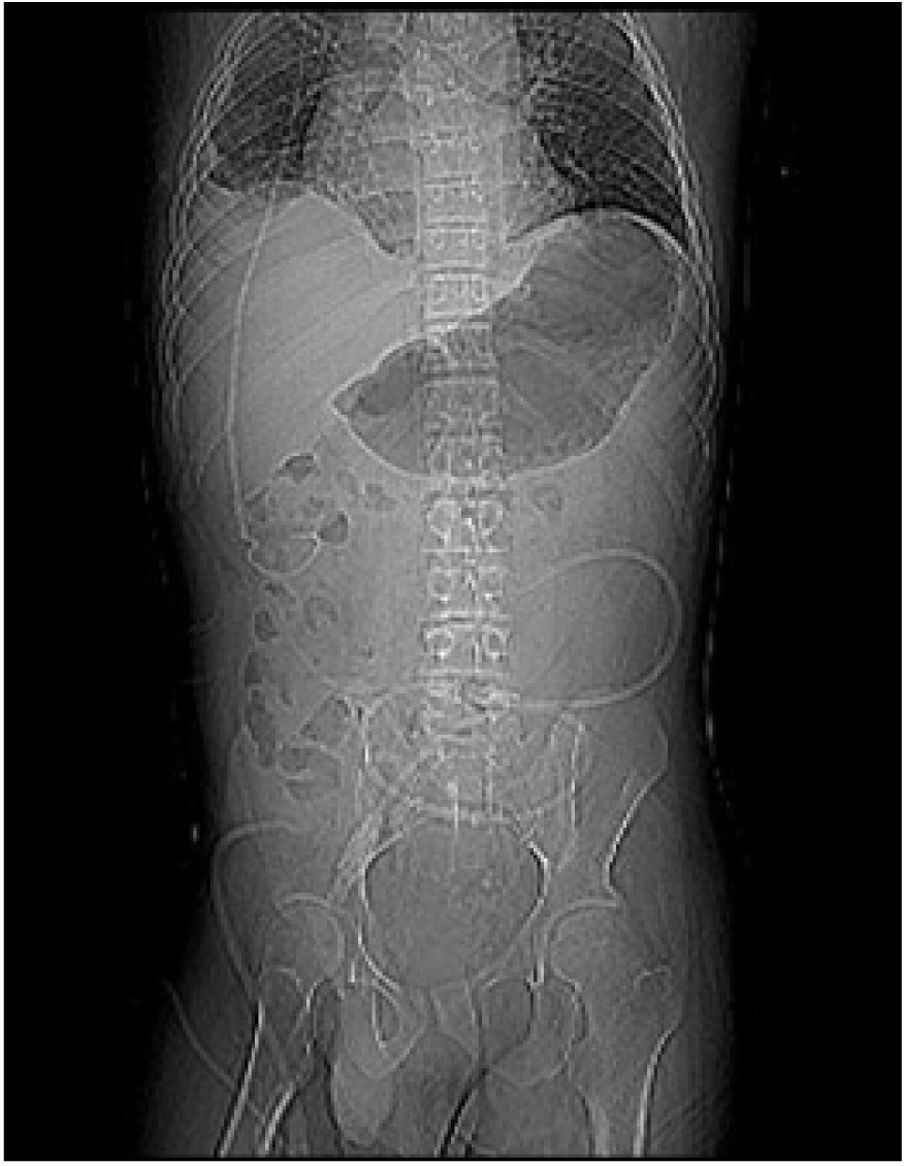
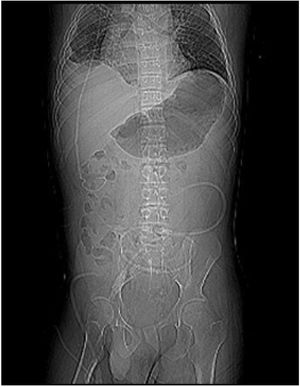
For 4 years, he had several arteriovenous fistulas and short and long-term vascular catheter implants resulting in central vein thrombosis and stenosis. The patient underwent bladder enlargement (Mitrofanoff) and external urinary diversion for subsequent kidney transplantation. The patient evolved with failure of vascular access for HD and a Tenckhoff catheter was inserted (Fig. 2) and PD started, a procedure did not have infectious/neurological complications for 6 months.
The DP is important for the survival of patients with CKD and difficulty of vascular access, especially as a bridge to the kidney transplant,5 but is still it is not frequently used as a first option, which may be attributed to the lack of information and difficulty access. Socioeconomic conditions may also influence the decision to start HD.6
There is some consensus on the absolute contraindications to PD, such as the presence of multiple adhesions, previous abdominal surgeries, hernias, infections, and local neoplastic processes.2 The presence of abdominal devices generated discussions about the effectiveness and safety of PD. According to Dolan et al. in United States, up to 2000, the prevalence of patients with hydrocephalus and a DVP drainage valve using PD was one in every 150 children.7 In the case of adults, only few rare cases have been described so far.
The first cases published in 1989 were patients with a ventriculoperitoneal shunt on PD. They were 2 children with spina bifida and CKD that were started on PD and remained until receiving renal graft without evidences of infectious or neurological complications.8 Grunberg and Anabella Rebori reported the experience in Uruguay with 9 children with ventriculoperitoneal shunts on PD; in this group, 2 patients had recurrent peritonitis and were changed to HD, they had no evidence of ventricular valve dysfunction or associated neurological infection.9
It is suggested that the rate of peritonitis and ascending infection of the central nervous system is considerably low, and should not be an obstacle to the indication of PD if RRT is required. The incidence rates of peritonitis correspond to one episode every 19.6 months, which is similar to that of the pediatric population without a ventricular catheter. Dolan et al. postulate that, as it is a serious infection with a high potential for mortality, there should be a frequent search for an infectious process in the cerebrospinal fluid (CSF).7
Despite the number of reported cases, it has not been defined whether the presence of long-term DVP could interfere with the surgical technique of Tenckhoff catheter insertion, or more specifically if the functionality of the peritoneal cavity could alter the physiology of the peritoneum; such a theory is not yet proven. The consensus is that since it is a unidirectional valve with an antireflux mechanism, the risk of back flow of the dialysate to the ventricles is small.9
There is no consensus among the authors about whether there is benefit obtained from the migration of the site of ventricular bypass at the same time of the surgical insertion of the peritoneal catheter. Abo et al. suggest that in patients whose shunt is made when the patients is already on PD, the technique should be reviewed, opting for ventriculo-atrial shunt.10
Our PD experience with DVP is that it is safe, efficient, without procedure associated infections. Since the period of time of observation has been relatively short, it is not possible to determine whether with a longer period of DVP there would be an increased risk of alterations in the physiology of the peritoneal membrane, and consequently a failure in clearance. We conclude that this modality of RRT was performed successfully and objective studies that support its safety in the adult population are still lacking.
We are grateful for the support received from the professors and health personnel of the Peritoneal Dialysis Unit of the Professor Edgard Santos University Hospital.
Please cite this article as: Silva Novaes GR, Gutiérrez-Peredo GB, Montaño-Castellón I, Gutiérrez-Peredo AJ, Labanca Júnior MN, Mattos Brandão O, et al. Diálisis peritoneal en paciente adulto con mielomeningocele y derivación ventriculoperitoneal. Nefrologia. 2022;41:708–710.