INTRODUCTION
Margarita Rufino et al’s1 excellent original article “Patients treated with plasmapheresis: a case review from University Hospital of the Canary Islands” has also been published in this very issue of Nefrología, reviewing a nephrology department’s experience using this technique. In the Introduction, the authors highlight that plasmapheresis has become a sub-specialty within nephrology given nephrologists’ command in using blood cleansing techniques, which is an opinion that we completely agree with. In this Editorial Comment we would like to explain why therapeutic apheresis (TA) should be integrated in our department. However, before indicating such reasons, we would like to highlight the importance that this therapeutic method currently has.
WHY IS THERAPEUTIC APHERESIS IMPORTANT AT PRESENT?
In 1982, the American Society for Apheresis (ASFA) was founded, with a series of objectives, such as controlling the TA indications and the cost-benefit ratio for the different apheresis procedures. To that end, the Journal of Clinical Apheresis was published. Furthermore, the International Society for Apheresis also created its own journal Therapeutic Apheresis, both published quarterly.
One of the best contributions that these organisations have made to TA, especially the American Association of Blood Banks (AABB) and the ASFA, was to create the guidelines for plasmapheresis use, classifying its indications into four categories (I-IV) in accordance with its effectiveness. These categories are updated every three years. In 2010, the ASFA presented its 5th Edition, with a special issue.2
In the last decade, various official TA work groups have been created in various countries, with the aim of registering and controlling apheresis indications and results, i.e. Canada,3 Switzerland,4 Japan,5 and Italy.6 In 2004, a therapeutic apheresis work group (GTAF) was founded within the Spanish Society of Nephrology (S.E.N.). It is still running, and thanks to the board of directors’ support and enthusiasm, more and more professionals are becoming members. Recently, a GTAF has been created in Argentina, which forms part of the Argentinean Society of Nephrology (S.A.N.), closely associated with the S.E.N.
ARGUMENTS FOR INTEGRATING THERAPEUTIC APHERESIS IN NEPHROLOGY
There are numerous reasons why TA should be integrated in nephrology. The basics are described below:
1. Definition. TA’s purpose is to eliminate molecules and immunocomplexes that determine an illness from the bloodstream using different blood cleansing procedures (BCP). Haemodialysis (HD) is the main BCP. Its objective is to eliminate light and medium weight molecules resulting from renal failure. The remaining BCP included in TA are used more or less selectively for various illnesses depending on the molecular characteristics or the immunocomplexes that are to be cleansed.
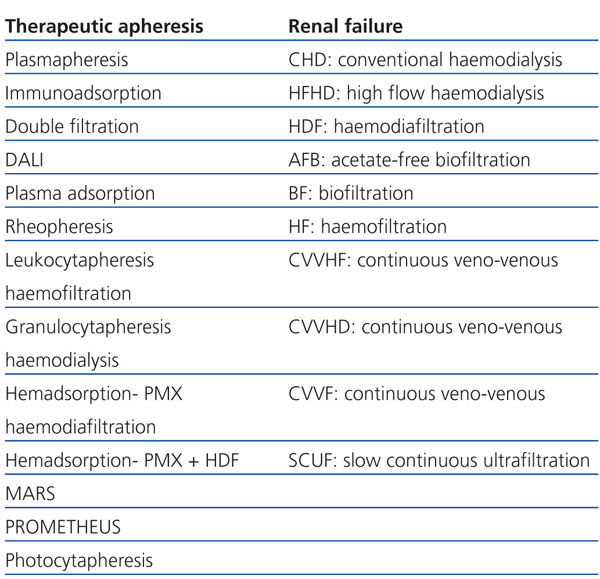
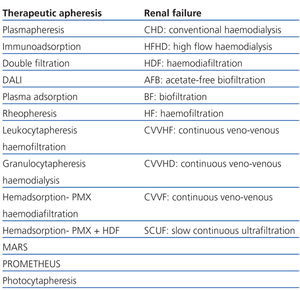
2. Blood cleansing procedures. There are numerous BCP; TA is currently used for more than 80 different illnesses, corresponding to most medical specialities. All BCP use extracorporeal circulation (ECC), which is best understood by trained nephrologists. As shown in Table 1, we divided the 23 BCP into two groups: the first group shows the procedures that are used for TA in accordance with indications in ASFA’s categories I, II and P2. The procedures indicated for chronic and acute renal failure are in the second group. For both groups, the patients’ treatment may be acute or chronic, such as HD or LDL-apheresis. No other specialty is able to provide such variety in treatment.
3. ECC All BCP included in the TA require an ECC, similar to that used in HD. The following is therefore needed: a) vascular access to provide an average blood flow of 100±20ml/min, which could be performed using vascular accesses similar to those used for HD, such as arteriovenous fistulae (AV) or central, temporary, or permanent catheters. There are BCP such as leukocytapheresis or granulocytapheresis which can be performed via the peripheral vein, and which need a blood flow of 50-60ml/min; b) anticoagulation during the apheresis process similar to HD, generally with heparin, although citrate is also used, and c) different lines, filters and monitors used for therapeutic apheresis, similar to the ones used for HD.
4. Knowledge of ECC and its complications. Being familiar with ECC techniques is essential, and only nephrology professionals are. They know the initial, maintenance and end manoeuvres for these extracorporeal procedures, and their complications. We must take into account that most complications are reversible, and such reversibility mainly depends on how early the disorder is diagnosed and treated, and therefore, on the professionals’ experience. It is essential to have this knowledge, not only for the patient’s safety but also from the financial point of view, considering that these techniques are costly.
5. Chronic programme maintenance. TA is mainly indicated as an acute treatment, but there are a series of disorders that should be treated regularly, either restrictively, as is the case for inflammatory bowel diseases with leukocyte apheresis or granulocytapheresis, every week for 5-8 weeks, or in senile macular degeneration, in which rheopheresis is performed two sessions a month, for 5-6 months. Furthermore, an unlimited chronic TA programme could be established, as is the case for the homozygous and heterozygous familiar hypercholesterolemia and for some neurological diseases, which is similar to the HD programme.
THERAPEUTIC APHERESIS AND NEPHROLOGY IN SPAIN
TA has been incorporated by nephrology and supported by the S.E.N for many decades. Over the past 30 years, this therapeutic method has been developed interruptedly, using various BCP, proving that it is part of nephrology. Proof of such claim are some of the following scientific activities that have been established in recent years:
1. Forming the GTAF integrated in the S.E.N. since 2004.
2. Spanish Second Symposium on Therapeutic Apheresis, held in the nephrology department of the Hospital de Logroño, on 11 and 12 February 2010.
3. Conferences on TA.
World Congress of Nephrology, Milan, Italy, 22-26 May 2009.
16th Argentinean Society of Nephrology Conference. Paraná City, Mar del Plata, Argentina 15 September 2009.
21th Nephrology Winter Meeting. Candanchú, Spain, 7-11 April 2010.
31st Spanish Conference of the Spanish Society of Internal Medicine (SEMI). Oviedo, Spain 18 November 2010.
Northern Nephrology Societies’ meeting. Pamplona, Spain 30 November 2010.
4th Spanish Conference on Obesity and Cardio-Metabolic Risk Factors. Madrid, Spain. 4 February 2011.
National Conference on Therapeutic Apheresis in Argentina. Paraná City, Santa Fe and Rosario, Argentina, 18 and 19 March 2011.
Annual Congress of the Spanish Society of Dialysis and Transplantation (SEDYT). Granada, Spain. 11-13 May 2011.
4. Healthcare activities
In Spain, there are numerous nephrology departments that currently have a more or less active TA programme. The following should be highlighted:
Torrecárdenas Hospital Complex, Almería, Spain.
San Carlos Clinical Hospital, Madrid, Spain.
University Hospital of the Canary Islands whose experience is reflected in this issue’s Editorial.
Gregorio Marañón University General Hospital, Madrid, Spain.
Throughout our long 29-year experience with TA, we have performed 10 050 sessions on 1157 patients, with different apheresis procedures such as plasmapheresis, immunoadsorption, direct adsorption of lipoproteins (DALI), double filtration, rheopheresis, leukocytapheresis, granulocytapheresis, hemadsorption-Pmx, molecular adsorbents recirculating system (MARS), and Prometheus for 73 different disorders across different medical specialities. The results have been excellent, with a very good tolerance and minimum complications. Treatment has been either acute or chronic, over programmed time periods.
OBJECTIVES OF THERAPEUTIC APHERESIS INTEGRATED IN NEPHROLOGY
The following objectives can be achieved by the GTAF:
1. Create a national register which features the disorders treated with the different apheresis procedures in agreement with four ASFA categories.
2. Regularly publish the results from this register so that they can serve as a control and guide in Spain.
3. Offer to conduct multicentre studies related to different techniques and clinical studies.
4. With S.E.N.’s support, promote this new work group as much as possible, through different communications and presentations, to inform and arouse interest in nephrology departments.
5. Inform health departments in the different Spanish regions and the main hospitals’ managers, to ensure that TA is recognised as an effective therapeutic method, and to request financial support so that TA can be performed without any difficulties.
REFERENCES
Reference Journals: Therapeutic Apheresis and Dialysis and Journal of Clinical Apheresis.
Most Spanish nephrologists have the book Aferesis Terapéutica7 which describes the basis, indications, procedures and TA management in a simplified way. It can be a great help for nephrologists that are interested in becoming familiar with this therapeutic method.
The S.E.N. Grupo Editorial Nefrología will publish the Manual de la Aferesis Terapéutica Basado en la Evidencia which we have written based on the Guidelines on theUse of Therapeutic Apheresis in Clinical Practice-Evidence-Based Approach from the Apheresis Applications Committee of the American Society for Apheresis2 and our own experience. We believe that it will be extremely useful and serve as a continual aid in TA clinical practice.
COMMENTS
Our opinion is that the arguments shown are solid enough to support that TA should undoubtedly belong to nephrology. Nobody would be able to perform this technique like nephrology doctors and staff.
Table 1. Blood cleansing procedures applied to therapeutic apheresis