Acute post-infectious glomerulonephritis (APGN) is primarily a disease found in infants that occurs following infection of the respiratory tract or impetigo.1,2
This disease is uncommon in older patients, but aging has become an important risk factor. Four decades ago, only 4%-6% of adults with APGN were older than 65 years of age, compared to 34% in recent reports.3
Comorbidities such as decreased renal function, diabetes mellitus, arterial hypertension, hyperlipidaemia, cardiovascular disease, and neoplasia contribute to the modification of the clinical presentation and natural progression of this condition. APGN is present in 3%-6% of biopsies, and is often an unexpected finding. Renal function is recovered within 3-4 weeks in 95% of cases, although this rate is much less predictable in the elderly.1,3,4
The treatment of APGN is based on antibiotics, diuretics, hypotensive drugs, and occasionally haemodialysis.2,5
We present four cases of patients older than 55 years with acute renal failure and nephritic syndrome, three of which were preceded by a respiratory infection and substantially elevated creatinine levels, and the fourth of which had nephritic/nephrotic syndrome with no prior infection and conserved renal function.
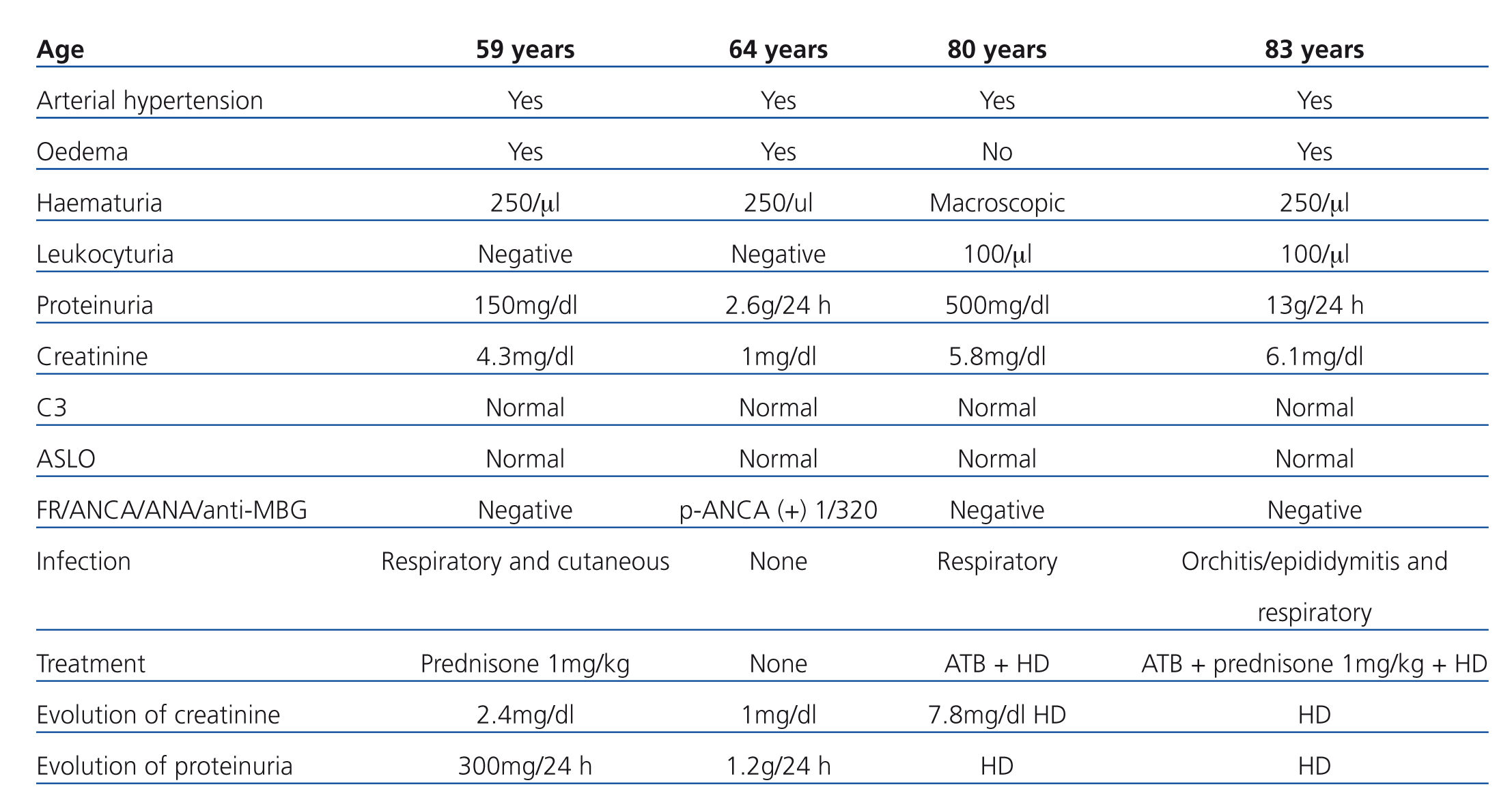
Case A: A 59-year-old male with chronic kidney disease (CKD) and rheumatoid arthritis, hospitalised due to nephritic syndrome in the context of a cutaneous infection by methicillin-resistant S. aureus (MRSA) and a respiratory infection. Specific antibiotic treatment was administered with no improvements in clinical or laboratory parameters.
Case B: A 64-year-old male with no prior symptoms, hospitalised due to nephritic syndrome with normal renal function. During hospital stay, treatment was administered with diuretics, which improved the symptoms, although successive consultations revealed persistent microhaematuria and nephrotic-range proteinuria with p-ANCA (+).
Case C: An 80-year-old male with CKD, hospitalised due to macroscopic haematuria and severe deterioration in renal function with a very recent history of respiratory infection. Antibiotic treatment was administered with improved respiratory symptoms, but worsening renal function.
Case D: An 83-year-old male, hospitalised due to nephritic/nephrotic syndrome in the context of epididymitis and respiratory infection several days after a transurethral resection. The patient progressed poorly under treatment with antibiotics and diuretics.
All patients underwent complementary testing to determine the microbiological aetiology of the infections, with MRSA found in only one case. Given the persistent deterioration of renal function despite treatment with antibiotics and diuretics, a renal biopsy was taken.
All four biopsies led to a diagnosis of APGN.
In case B, the patient without deteriorated renal function, the same diagnosis was reached but in the recovery phase. In the other three cases, corticosteroid treatment was started with a positive response in one patient, case A.
However, in cases C and D, the patients failed to recover renal function and remained on a programme of periodical haemodialysis; one of these patients still retains residual diuresis after 8 months on haemodialysis.
To conclude, in the presence of nephritic syndrome, one differential diagnosis that must not be forgotten is APGN, despite the fact that this pathology is uncommon in the adult-senile population. We must keep in mind the personal history of these patients and any predisposing factors that would compromise the immune system, since it has been reported that these factors affect the susceptibility of a given patient to developing this pathology.3,6
Severe renal deterioration is the first form of presentation of this condition and is associated with older age, implying poor prognosis and patient evolution. As such, it is of vital importance to keep this differential diagnosis in mind when treating senile patients.
Conflicts of interest
The authors have no conflicts of interest to declare.
Table 1. Clinical and laboratory values