To the Editor:
Hyperkalaemia is one of the most severe electrolyte disorders, especially in patients with chronic kidney disease (CKD) who are incapable of efficient renal potassium excretion.1-4
High potassium levels lead to changes in transmembrane potential of the cells of skeletal and cardiac muscles, the organs which are most clinically affected.1-4
In patients with pacemakers, hyperkalaemia can cause dysfunction of the device and therefore the patient’s life may be at risk.4,5
We report the case of a pacemaker malfunction due to hyperkalaemia in a patient with multiple risk factors for developing the aforementioned electrolyte disorder.
CASE REPORT
A 72-year-old female who came to the haemodialysis centre, after the long weekend interdialytic period, complaining of generalised muscle weakness, to the point that it prevented her from walking.
She had stage V CKD and had been on periodic haemodialysis for four years. She had a single chamber pacemaker due to chronic atrial fibrillation with symptomatic bradycardia (repeated syncope). Other history findings included type 2 diabetes mellitus treated with oral anti-diabetic medication, and high blood pressure. Her regular medication included omeprazole, amiodarone and aspirin (none of which affected on potassium homeostasis). Her adherence to medical treatment was poor and she often consumed unsuitable foods. Physical examination was unremarkable except for the aforementioned muscle weakness. The constants were correct and the patient was normoglycaemic. The electrocardiogram (ECG) showed a pacemaker rate, without any other abnormalities. The urgent analysis revealed potassium levels of 8.2mEq/l. While waiting for the haemodialysis session, she began conventional treatment for hyperkalaemia, with calcium gluconate, intravenous salbutamol and an infusion of insulin and glucose being administered.
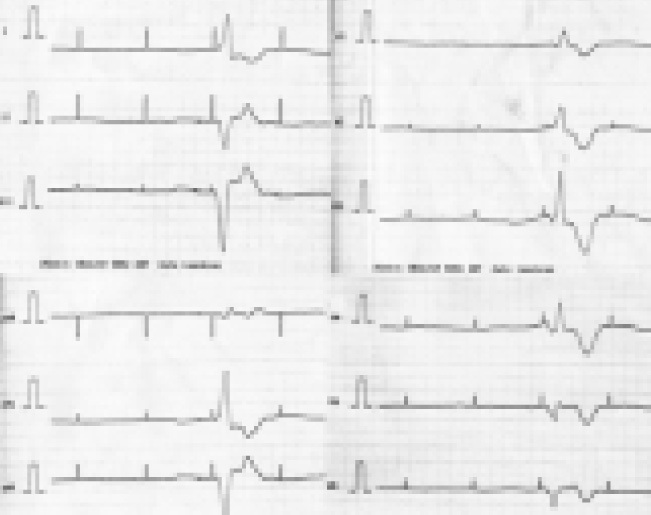
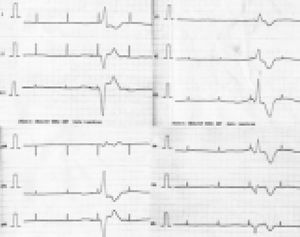
Minutes after beginning this treatment, the patient experienced a sudden decrease in her level of consciousness, with undetectable blood pressure and signs of peripheral hypoperfusion. At that moment, the ECG showed failure of ventricular capture (Figure 1). Urgent haemodialysis was performed, with both symptoms and electrocardiographic abnormalities being quickly and completely reversed.
DISCUSSION
Severe hyperkalaemia is a common problem in patients with advanced CKD.1 It may affect 5%-10% of patients on chronic haemodialysis monthly. It may also require urgent haemodialysis in up to 24% of patients with end-stage CKD and it has a significant mortality rate.1
Potential causes of hyperkalaemia in patients such as ours are multifactorial and may include, in addition to CKD, metabolic acidosis, hyporeninemic hypoaldosteronism (common in diabetics), defects of cell Na+/K+-ATPase and poor diet1-3 (recognised by our patient).
In patients with cardiac pacemakers, hyperkalaemia can cause various types of dysfunction of the device, with very serious consequences.4,5 In our case, there was a failure of ventricular capture. In this situation, excess of extracellular potassium increases the resting potential of the myocardial cell membrane.4 If this potential exceeds the energy emitted by the pacemaker according to its programming, cardiac muscle cell depolarisation is inhibited. This situation is recognised in the ECG by the absence of depolarisation after the spicules. The clinical manifestation, which is clearly serious, is asystole.4,5
In conclusion, the presence of a cardiac pacemaker does not always protect the myocardium from the deleterious effects of hyperkalaemia. Moreover, the device requires a normal electrolyte balance for proper operation. Therefore, heart rate monitoring, which is essential for all symptomatic hyperkalaemia, should not be overlooked in patients with pacemakers. Likewise, the presence of a pacemaker must not be a decisive factor when urgent haemodialysis is indicated for severe hyperkalaemia.
Conflicts of interest
The authors declare that they have no conflicts of interest related to the contents of this article.
Figure 1. 12-lead electrocardiogram showing the failure of capture (absence of QRS complexes after the first, second and fourth spicules)