To the Editor,
Bullous or ampullary epidermolysis is defined1 as a group of rare inherited skin diseases characterised by a tendency of the skin and mucous membranes to separate from the underlying tissues after minimal trauma; it is transmitted as both dominant and recessive factors and is caused by COL7A12 gene mutations: The different varieties can be grouped into three main1,3 types: epidermolysis bullosa simplex of dominant autosomal inheritance, junctional epidermolysis bullosa of autosomal recessive inheritance and dystrophic or dermolytic epidermolysis bullosa. Furthermore, the latter includes three forms: dominant, mild recessive, and severe recessive or Hallopeau-Siemens.
Hallopeau-Siemens dystrophic epidermolysis bullosa is the most widely severe form4,5. It begins at birth with blistering of skin and mucous membranes. Blisters and vesicles heal forming atrophic scars. Extracutaneous4 manifestations include: dystrophy or absence of nails, sparse head hair or alopecia, excessive dental caries, microstomia, mouth ulcers, lingual tip fixation to the floor of the oral cavity, pseudosyndactylia, syndactylia and deformities of hands and feet. Furthermore the surface epithelium of the respiratory tract, gastrointestinal tract and ocular system are affected by blistering. These patients usually suffer from anaemia, malnutrition and stunting. One of the major complications of the disease is the development of chronic terminal kidney disease3, which causes early death and with the main complication of establishing an appropriate access route for dialysis.
CASE REPORT
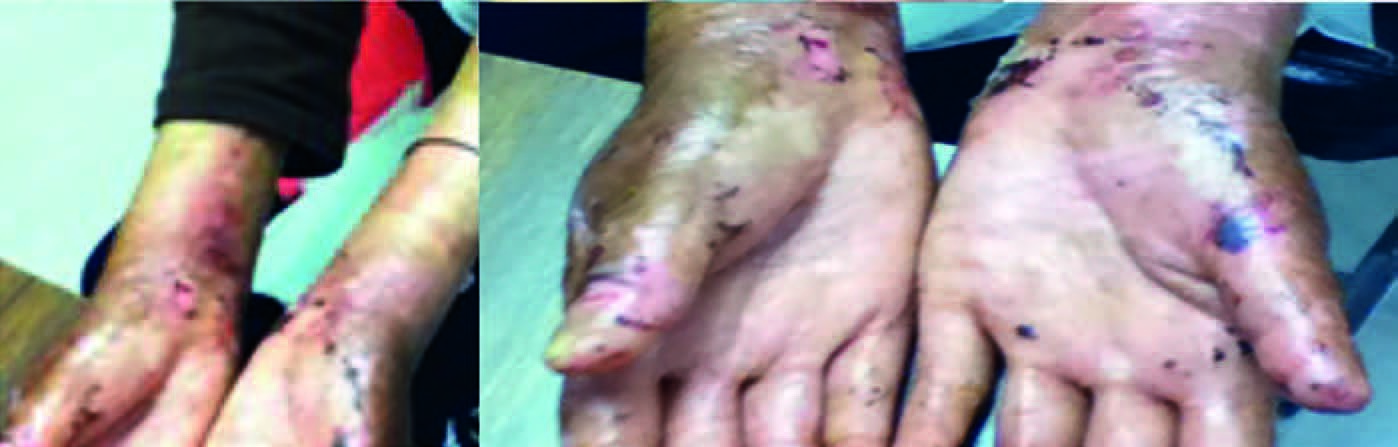
A 31-year-old female patient was referred to dermatology for evaluation of renal function after having been diagnosed with epidermolysis bullosa at birth and dysphagia for solid food that did not require endoscopic treatment. The endocrinology department ruled out associated hypothyroidism and suprarenal insufficiency. No previous diagnosis of chronic kidney disease in the last year, she was referred due to azotaemia. On admission: weight 45kg, height 1.55m, cutaneous pallor +, partial alopecia, a few scattered haematic crusts in the oral cavity, microstomia with lingual fixation to floor of oral cavity, generalised erythema, dermabrasion areas with blistering that did not affect the cervical region, deformities of both hands and bilateral scars and erythema (Figure 1).
Relevant laboratory abnormalities: haemoglobin 9.1g/dl, K 7.2mmol/l, urea 345mg/dl, creatinine 9.5 mg/dl, albumin 2g/dl; Urinalysis (GUE) urinary density (UD) 1009, pH 5.5, proteins +, erythrocytes 150 cells/ul; arterial blood gases: pH 7.21, PCO2 27, PO2 92%, 92% Sat, HCO3 7.6; 24h proteinuria 1.8g/day; urine volume: 1500cc; right kidney ultrasound 7.5 x 2.5cm and left kidney 7.1 x 2.6cm, loss of corticomedullary ratio. Electrocardiogram symmetrical peaked T waves and isolated PVCs in all precordial leads. We decided to place an indwelling tunnelled catheter due to the increased risk of infection with the Tenckhoff catheter.
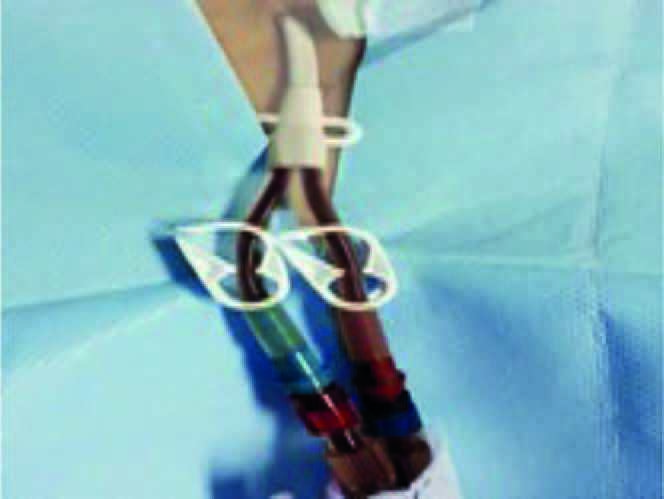
Subsequent to cardiac monitoring, monitoring of non-invasive blood pressure and pulse oximetry, intravenous sedation and analgesia was administered. Right jugular region and the exit site were identified with minimal epithelial damage, and the catheter was tunnelled placing a Permacath catheter, its position was checked by means of a portable chest X-ray. Adequate arterial and venous return was achieved, and the skin (Figure 2) was sutured. Haemodialysis was started with symptom remission, patient was discharged due to clinical improvement and enrolled in the chronic haemodialysis programme.
DISCUSSION
Epidermolysis bullosa is an autosomal recessive hereditary skin disease that involves all organs from birth. Chronic kidney disease is the second leading cause of death3 in these patients after squamous cell carcinoma; it is relevant to mention that many patients die due to associated dilated cardiomyopathy6. Kidney disease is usually due to the development of secondary amyloidosis, IgA nephropathy, post infectious glomerulonephritis, and obstructive uropathy3,7. Other factors contributing to the development of chronic kidney disease include: dehydration, dysphagia, vomiting and hypoalbuminaemia8,9.
When developing chronic kidney disease, access to dialysis therapy is considered a big issue. Skin lesions and the tendency to become infected limit the use of peritoneal dialysis as an option. Another limitation to performance of an arteriovenous fistula is the development of skin lesions and local contractions, which prevent the placement of vascular catheters7. Therefore, placement of a tunnelled haemodialysis catheter in a central vein is, at present, considered the best option10.
Conflicts of interest
The authors declare that they have no conflicts of interest related to the contents of this article.
Figure 1. Epidermolysis bullosa dermatological lesions seen on patient with chronic kidney disease on admittance.
Figure 2. Permacath catheter permeability following corroborated procedure in urgent haemodialysis.