Dear Editor,
The most frequent complications of arteriovenous fistula (AVF) type subcutaneous vascular accesses are infections, thrombosis and complications due to low flow, such as steal syndrome and stenosis, both intrinsic to anastomoses and venous return. An infrequent complication, but one that is difficult to treat, is calciphylaxis. It affects small peripheral arteries, causing very painful skin necrosis.1-9 The case that we present below is unusual because, although it presents some similarities with calciphylaxis, it differs in pathogenesis, treatment and resolution, since it is a surgical complication in a patient with a very calcified arterial bed.
The case is a 75 year old man, with a history of stage 5 chronic renal failure of unknown origin, who has been on haemodialysis for 7 years. Other history data of interest: chronic obstructive pulmonary disease, ischaemic stroke without sequelae, high blood pressure, former smoker, chronic atrial fibrillation anticoagulated with acenocoumarol, hypercholesterolemia, erosive duodenitis, appendectomy, several episodes of hyperpotassaemia, intermittent claudication, and femoropopliteal revascularization.
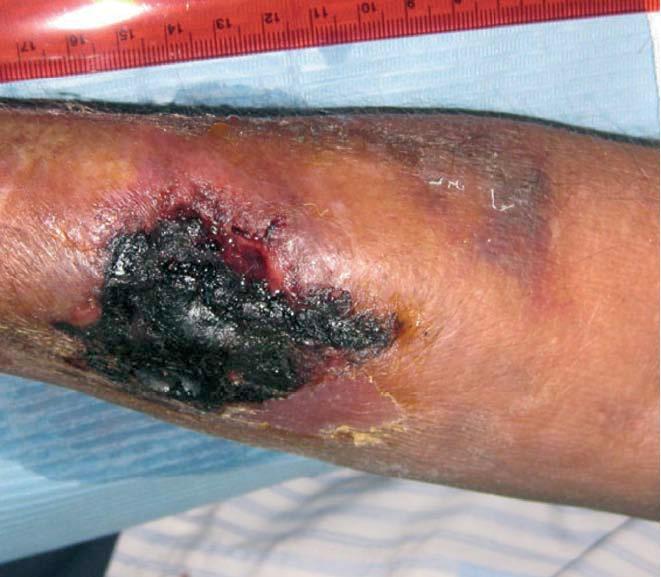
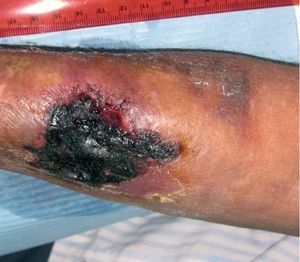
Regarding vascular access, haemodialysis was started through a right jugular tunnelised catheter, subsequently a humero-cephalic arteriovenous fistula (AVF) was performed in the left arm, but it did not function. Subsequently a radio-cephalic AVF was performed without problems in the right arm, and the catheter was removed. It functioned without any problems from the beginning, but progressively, during 2008, a very high recirculation index was detected (44.3%), with the consequent infra-dialysis. After consultation with the vascular surgery department, it was decided to carry out a reconstruction at a more proximal site, since the artery was very calcified. After surgery, there was a significant improvement of recirculation values, as well as analytical values corresponding to urea kinetics (KtV). On the 7th of May 2009, this vascular access suffered thrombosis; therefore a left jugular tunnelised catheter was implanted. Subsequently, on 18th August 2009, a new, more proximal, radio-cephalic AVF was performed in the right arm. A surgical complication developed, an expanding haematoma which affected the whole forearm. Progressively, the patient suffered pain and coldness of the right hand, with decreased pulses, compatible with steal syndrome. As to the antebrachial haematoma, its size did not decrease, and an ever greater area of tissue necrosis developed in the region of the surgical wound, reaching a size of 4 cm in length by 4 cm in width, with underlying granulation tissue surrounding the scab, as shown in Figure 1. In view of this situation, an arterial echo Doppler of the right upper limb was performed and a functioning AVF detected, with arterial steal, and a non-encapsulated haematoma. Pain increased, as also coldness and hand functional impotence, so we ligated the AVF on the 10th of September 2009. After intervention the symptoms of steal syndrome disappeared, the necrotic scab became detached and the antebrachial haematoma began reabsorption. For 2 months we proceeded to dress the underlying wound beneath the necrotic scab, until complete healing was achieved. Since then, the patient has been asymptomatic, and it was decided to maintain the left jugular tunnelised catheter as a permanent vascular access in view of the failed attempts to obtain other subcutaneous accesses.
Differential diagnosis with calciphylaxis is necessary, since the patient’s risk factors predisposed to this disorder, and the skin lesion had certain similarities. However, since the cause-effect relation with surgery was evident, and hand ischemia caused by the steal syndrome caused the patient intense pain and functional impotence, we opted for AVF ligature. It led to the complete recovery of hand ischemia and the skin necrosis, after opportunely applying dressings, with no sequelae. If the case had not resolved, it would have been necessary to perform a biopsy to rule out calciphylaxis. There are no similar cases described in the scientific literature, the most similar disorders are pressure ulcers, caused by external pressure in bedridden patients or patients with reduced mobility.10-15 Pressure in our case was caused from the subcutaneous compartment due to a space impingement on the surgical wound area caused by the expanding haematoma, which, together with defective vascularisation due to severe arterial calcification, caused skin necrosis.
Figure 1. Skin necrosis