To the Editor:
Multiple myeloma (MM) is a clonal proliferation of plasma cells that leads to excessive production of a certain type of immunoglobulin or a fraction thereof. In 12-20% of patients, acute renal failure (ARF) occurs, mainly due to cast nephropathy (myeloma kidney) due to tubular damage. Survival depends on the recovery of renal function.
We present the case of a 63-year-old female, without relevant medical history, who was admitted with ARF secondary to MM (kappa light chain cast [LCC]) and remains dependent on renal replacement therapy (RRT) from diagnosis. Online haemodiafiltration was performed four times a week, in sessions lasting 240 minutes, maintaining residual diuresis (RD: 1000 cc/24 h) and serum creatinine levels around 5mg/dl.
The aim of MM treatment is to reduce the production of LCC with chemotherapy and corticosteroids and/or autologous bone marrow transplantation. Coadjuvant treatment includes various techniques of extracorporeal clearance.
There are currently two types of RRT used as MM coadjuvant treatment: high cut-off haemodialysis (HCO) and haemodiafiltration with regeneration of ultrafiltrate (SUPRA-HFR). There are HCO studies in which these types of patients have a sustained rate of LCC reduction and recovery of renal function.1 However, in another study in 6 patients, a higher rate of LCC reduction was not associated with the recovery of renal function.2 SUPRA-HFR has recently been proposed for the removal of LCC in these types of patients.3,4
In our case, after obtaining LCC determinations and response to haematologic treatment, we decided to start SUPRA-HFR, three days a week, in 240 minute sessions.
We designed the following study to test the adsorption in resin of the LCC cartridge (kappa and lambda), of albumin and of beta-2-microglobulin with this haemodialysis technique, so that it may contribute to the removal of LCC, but without losing albumin. For this, we obtained blood samples every week pre-and post-haemodialysis and plasma water samples at minute 5 and 235 from the start of the technique, both pre- and post-cartridge.
The kappa LCC levels in serum were 105.19mg/l before the first session of SUPRA-HFR, and six weeks after the aforementioned treatment they were 61.18mg/l. The rates of reduction of each parameter both in blood and in plasma water are shown in the following two tables.
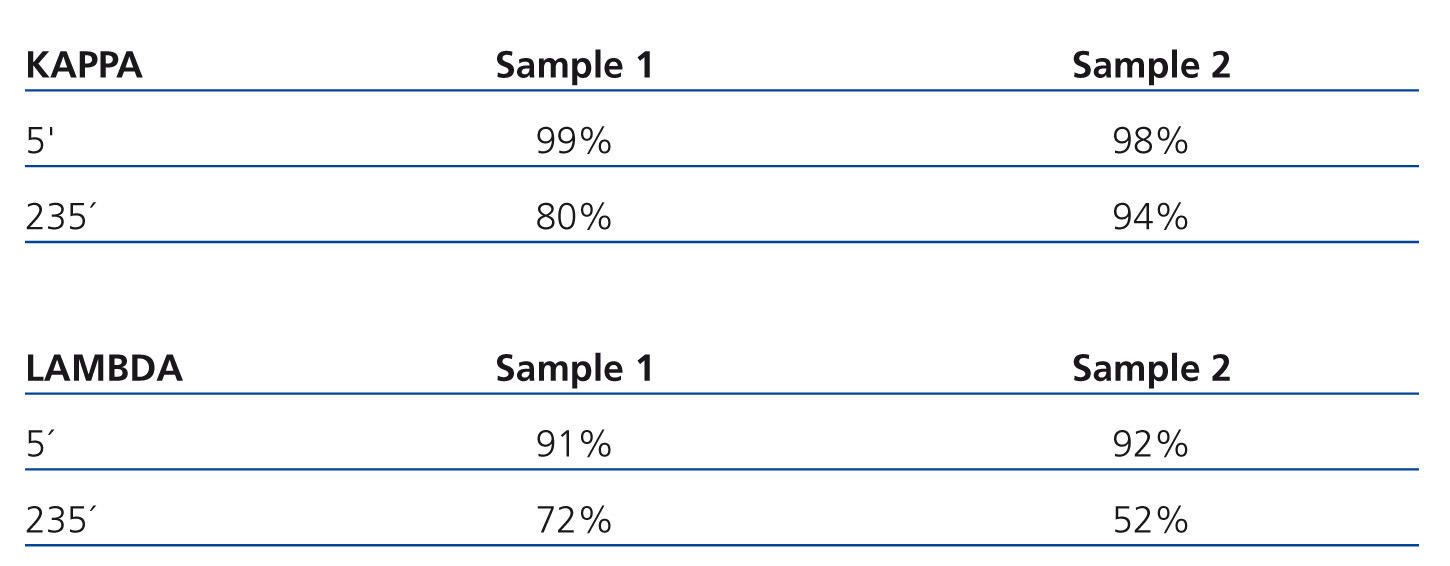
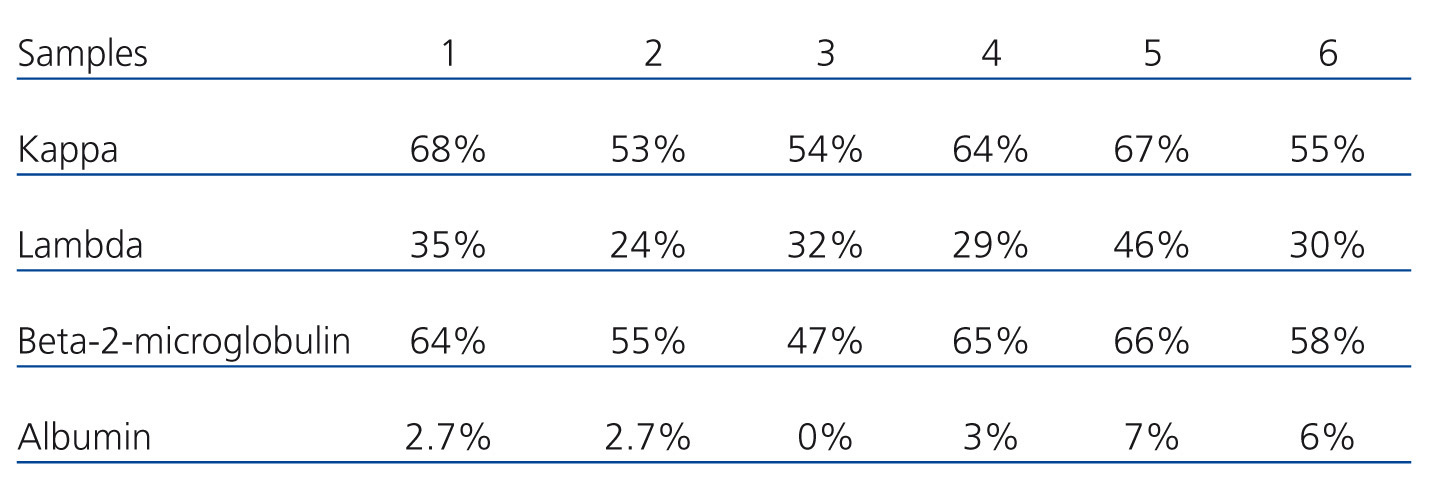
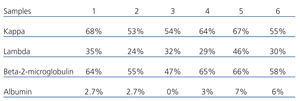
The results obtained show a mean blood reduction rate of 60% of kappa LCC, 32% of LCC lambda, 59% of beta-2-microglobulin and 3.5 % of albumin (Table 1). In plasma water, the rate of LCC reduction was much higher, both at the start and at the end of treatment: 98-99% of kappa LCC at the start and 80-94% at the end, in the first week of treatment (Table 2).
In spite of these results, the patient has not recovered renal function and she remains dependent on RRT, with blood creatinine of 7mg/dl and RD. She is awaiting an autologous bone marrow transplant.
With the results obtained, we can conclude that total saturation of resin does not occur, with a good rate of reduction of LCC being maintained (60% mean reduction of kappa LCC in serum), without the loss of albumin. Therefore, SUPRA-HFR is effective in the reduction of LCC as a coadjuvant treatment of MM.
Conflicts of interest
The authors declare that they have no conflicts of interest related to the contents of this article.
Table 1. Reduction rates in blood
Table 2. Reduction rates in plasma water