To the Editor,
Haemorrhagic fever with renal syndrome (HFRS) is a clinical condition secondary to infection with a hantavirus (Hantaan, Seoul, No Name, Andes virus, Puumala and Dobrava); the latter two varieties are endemic in rural areas of Eastern Europe, and of the two, infection with the Puumula virus has a better long-term prognosis.1
Rodents are the natural carriers of hantavirus, which is transmitted to humans when they come into direct contact with rodent secretions (urine, faeces and saliva).
The natural evolution of the disease entails 4 successive phases following an incubation period of about 3 weeks. The first phase is characterised by fever, followed by a phase with shock and oliguria; patients who survive this phase enter a phase with polyuria, which in turn is followed by a convalescence period of variable duration.
Thrombocytopoenia is common and may produce haemorrhages at any location.
Renal symptoms include proteinuria, haematuria and decreased glomerular filtration rate. Direct vascular endothelial lesions and tubulo-interstitial nephritis mediated by cytokines have been proposed as the underlying physiopathological cause.2
Diagnosis is based on a strong clinical suspicion, and confirmed by specific serological methods.3 Kidney biopsy is not necessary.4 A renal ultrasound can show the increase in kidney size and in resistance indices. Perirenal fluid collection is also a common finding (in addition to pleural or pericardial effusion or ascites). No vaccine or specific treatment exists; supportive therapy is of vital importance. One double-blind study showed decreased mortality given early treatment with ribavirin.5
Below, we describe our hospital’s experience with a case of HFRS secondary to infection with the Puumala virus.
The patient was a male aged 18 years with no relevant prior history who came to the Emergency Department due to fever, muscle aches and a frontal headache evolving over 3 days with no improvement following his doctor’s prescription of amoxicillin-clavulanic acid and paracetamol. Two weeks before, he had been hiking in a rural area of Slovenia.
The physical examination found a fever of 39.2ºC, normal blood pressure, no adenopathy, and diffuse pain upon abdominal palpation. The Emergency Department laboratory blood test found 10 010 leukocytes/mm3 with no eosinophilia; thrombocytopoenia of 32 000/mm3 with no platelet additives; haemoglobin: 18; haematocrit: 48%; creatinine: 1.35mg/dl; urea: 47mg/dl; lactate dehydrogenase (LDH): 324U/l. All other blood tests were normal.
Microhaematuria was present.
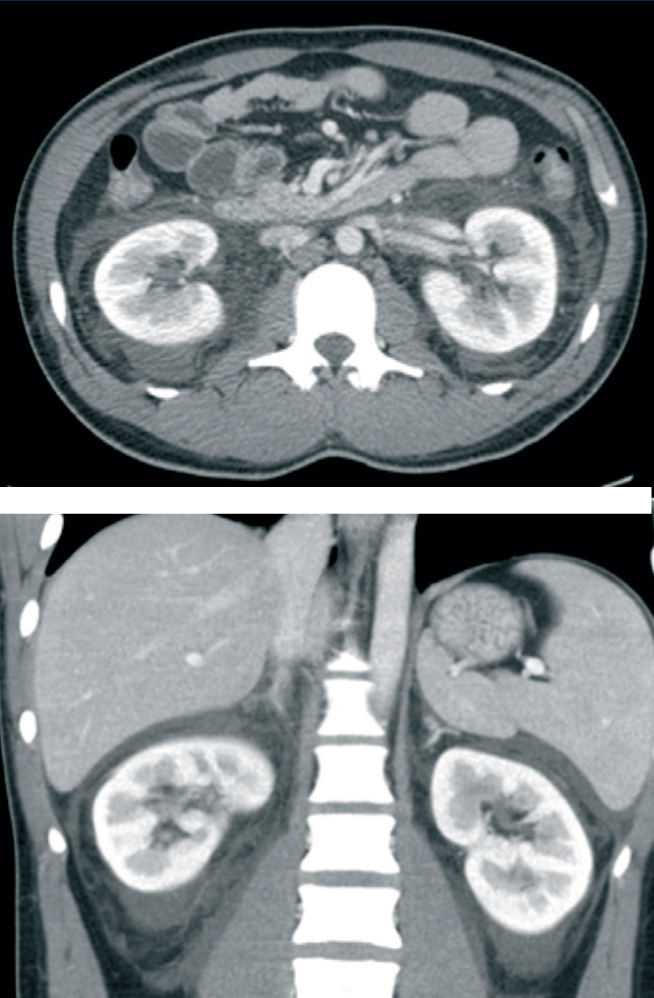
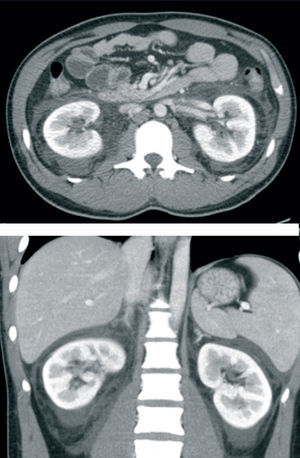
Thoracic and abdominal radiographies were normal. The abdominal ultrasound and the abdominal and pelvic CT showed morphologically normal kidneys with no ureteral dilation, with perirenal and pelvic free liquid. (Figure 1)
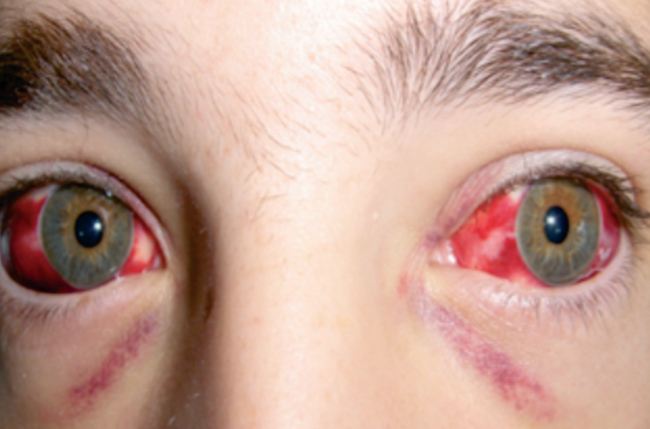
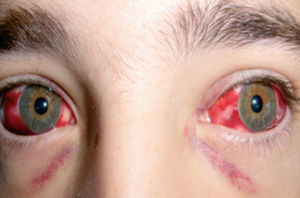
The patient was admitted for observation, which is why he was initially given empirical antibiotic treatment with ceftriaxone and levofloxacin after the samples were extracted. The day after admission, he suffered a conjunctival haemorrhage (Figure 2), tendency toward oliguria, the appearance of oedemas, and decreased renal function; his creatinine level was 2.7mg/dl. As a hantavirus infection was suspected, we opted for antiviral treatment with ribavirin (500mg/i.v. every 8 hours). The same day, 8 hours later, he suffered an episode of dyspnoea and tachypnoea with desaturation (89%) and hypoxia (pO2: 63), and the decision was made to send him to the Intensive Care Unit. On the fourth day after admission, the patient presented epistaxis that subsided with anterior nasal packing. The oliguria became more pronounced, oedemas increased and the renal function worsened with creatinine levels of 5.6mg/dl. We then decided to start haemodialysis by means of a temporary catheter in the right femoral vein. After 4 session of haemodialysis, we observed improvements in urinary volume and renal function. The immunological study (antinuclear antibodies, anti-neutrophil cytoplasmic antobodies, anti-DNA, anti-GBM antibodies, complementary components, immunoglobulins, protein electrophoresis, cryoglobulin, circulating immune complexes) and serology study for hepatitis B and C, HIV, Epstein-Barr virus, cytomegalovirus, leptospira, parvovirus B19 and toxoplasms were negative or normal. On day 7, the laboratory reported IgG (+) 1/512 for Puumala virus, and antibiotic treatment was consequently discontinued.
On day 13, the patient was discharged after completing the antiviral treatment, showing recovered renal function and a creatinine level of 1.25. At follow-up 5 weeks later, his renal function was completely normal (creatinine: 0.69, estimated glomerular filtration rate >60).
Figure 1. Abdominal and pelvic computed tomography
Figure 2. Conjunctival haemorrhage appearing the day after patient was admitted