Atrial fibrillation is the most frequent chronic arrhythmia in patients with chronic kidney disease. Oral anticoagulation with vitamin K antagonists and now direct oral anticoagulants have been and are the fundamental pillars for the prevention of thromboembolic events. However, there are no randomized clinical trials on the risk-benefit profile of oral anticoagulation in patients with chronic kidney disease stage 5 on peritoneal dialysis and there is little evidence in the literature in this population.
The objective of our study was to know the prevalence, treatment and professionals involved in the management of atrial fibrillation in peritoneal dialysis patients. For this purpose, we performed a descriptive analysis through a survey sent to different peritoneal dialysis units in Spain. A total of 1,403 patients on peritoneal dialysis were included in the study, of whom 186 (13.2%) had non-valvular atrial fibrillation. In addition, the assessment of the scores of thromboembolic and bleeding risks for the indication of oral anticoagulation was mainly carried out by the cardiologist (60% of the units), as well as its prescription (cardiologist 47% or in consensus with the nephrologist 43%).
In summary, patients on peritoneal dialysis have a remarkable prevalence of non-valvular atrial fibrillation. Patients frequently receive oral anticoagulation with vitamin K antagonists, as well as direct oral anticoagulants. The data obtained regarding the scores used for the assessment of thromboembolic and bleeding risk, treatment and involvement by Nephrology indicates that there is a need for training and involvement of the nephrologist in this pathology.
La fibrilación auricular es la arritmia crónica más frecuente en pacientes con enfermedad renal crónica. La anticoagulación oral con antagonistas de la vitamina K y actualmente los anticoagulantes orales de acción directa han sido y son el pilar fundamental para la prevención de eventos tromboembólicos. Sin embargo, no existen ensayos clínicos aleatorizados de su perfil riesgo-beneficio en pacientes con enfermedad renal crónica estadio 5 en diálisis peritoneal y son pocas evidencias en la literatura en esta población. El objetivo del estudio fue conocer la prevalencia, tratamiento y profesionales implicados en el manejo de la fibrilación auricular en diálisis peritoneal en nuestro entorno mediante el análisis descriptivo de una encuesta enviada a diferentes unidades de diálisis peritoneal de España. Se incluyeron en el estudio 1403 pacientes en programa de diálisis peritoneal, de los cuales 186 (13,2%) presentaban fibrilación auricular no valvular. Además, observamos que la valoración de los scores para el inicio del tratamiento anticoagulante la realizaba mayoritariamente el cardiólogo (60% de los centros), así como la prescripción de anticoagulación (cardiólogo 47% o conjuntamente con nefrólogo 43%).
En conclusión, los pacientes en diálisis peritoneal presentan una notable prevalencia de fibrilación auricular no valvular. Reciben frecuentemente anticoagulación oral con antagonistas de la vitamina K, así como con anticoagulantes orales de acción directa. Los datos obtenidos respecto a las escalas utilizadas para la valoración de riesgo tromboembólico y de sangrado, tratamiento e implicación por parte de Nefrología indica que existe una necesidad de formación e implicación del nefrólogo en esta patología.
Atrial fibrillation (AF) is the most frequent chronic arrhythmia in the general population; it is more prevalent in patients with chronic kidney disease (CKD),1 and is associated with an increased risk of stroke and thromboembolic events.2,3 Its prevalence ranges from 16 to 21% in subjects with CKD not on dialysis and from 15 to 40% in patients on hemodialysis (HD).4 Both pathologies, CKD and AF, are risk factors for the development of stroke. The synergistic effect of both entities may generate serious problems related to the risk-benefit profile involving bleeding and thrombotic risk associated with oral anticoagulation (OAC).1
OAC with vitamin K antagonists (VKA) has been the mainstay of treatment for the prevention of thromboembolic events in AF until recent years. Currently, the use of direct-acting oral anticoagulants (DOACs) have been introduced into clinical practice, demonstrating equal or greater efficacy in the prevention of thromboembolic events with a reduced risk bleeding in this population.5 However, there are no randomized clinical trials evaluating the efficacy and safety of OAC in CKD patients with an estimated creatinine clearance <30 mL/min, either with VKA or with DOACs, which makes it difficult to assess the risk-benefit profile of OAC in patients with advanced CKD or end-stage renal disease (ESRD) on renal replacement therapy.
In patients on regular HD, numerous studies with large databases have analyzed the prevalence, the risk of AF-related morbidity and mortality, and the risk-benefit of anticoagulation therapy.6–13 The association between AF and the risk of thromboembolic events in these patients is a matter of debate, as it is the benefit of OAC. A recent meta-analysis of observational studies questioned the usefulness of OAC in subjects with CKD on dialysis (mostly on HD),14 however the presence of AF in HD patients is associated with an increase in morbidity and mortality.15
In contrast, there are few studies that analyze the prevalence, incidence, prognosis and risk-benefit profile of OAC of AF in peritoneal dialysis (PD). Data from the United States Renal Data System (USRDS) show a prevalence of AF in PD of 23.3%.16 Furthermore, only 28% of patients received OAC (25.1% with warfarin).16 Evidence of the risk of thromboembolic events and the risk-benefit of OAC in these subjects is scarce. In PD, the data are contradictory. There are studies that describe a lower risk of intracranial hemorrhage, bleeding and thromboembolic events in patients on PD as compared to HD.17 However, another study shows that in patients with ESRD on PD the presence of AF is associated with an increased risk of ischemic stroke and mortality as compared to those without AF.18 Likewise, the benefit of VKA has been questioned by some authors,19 but not all in this population.20
Therefore, given the scarce evidence on the global prevalence, thromboembolic risk and risk-benefit profile of OAC in AF on PD, especially in the European population, we were interested to know the prevalence of AF on PD in our setting, as well as the treatments (anticoagulant/antiplatelet) received by these patients for the prevention of thromboembolic events.
The main objective of our study was to identify the prevalence of AF in patients on PD, and to find out who performs the assessment, prescription and management of anticoagulation therapy in these subjects.
MethodsThis is an observational, multicenter, cross-sectional and retrospective study. The aim was to analyze the clinical characteristics and therapeutic management of AF in patients over 18 years of age undergoing renal replacement therapy with PD.
Data were collected by conducting a survey using a Google questionnaire to 30 PD units in our country. The questions to be answered by each investigator are shown in Appendix Annex 1, mainly: the prevalence of nonvalvular atrial fibrillation (NVAF) in their PD patients, thromboembolic/stroke and bleeding risk scores used, anticoagulant/antiplatelet treatment prescribed, and professionals responsible for of management of this complication.
The study was carried out during the months of April-May 2020 and included 1,403 prevalent patients belonging to 30 PD units from different hospitals in our country. The study included prevalent patients in PD program for at least one month. Those receiving PD treatment due to cardiorenal syndrome that did not need replacement therapy were excluded.
A descriptive analysis of patient characteristics was performed, the categorical variables are shown as percentages. All continuous variables had a nonparametric distribution (Shapiro–Wilk test) and were shown as median and interquartile range (IQR).
ResultsOut of the 1,403 patients analyzed, 186 had NVAF. Mean 13.2%, median 11.7%, IQR 6.1–19.4 (Fig. 1). In the analysis of the prevalence of NVAF according to the number of patients per center (tertiles: <25, 25–55 or >55), no significant differences were detected. The median prevalence and IQR was 11.7 (9.5–13.3) in centers with less than 25 patients, 6.9 (3.2–21.7) in centers with 25–55 patients and 13.2 (6.3–20) in centers with more than 55 subjects (p = 0.791 analysis of variance [ANOVA] test). Also, there were no significant differences in prevalence according to geographical areas or autonomous regions (p = 0.71, ANOVA test).
Survey results: 1a Who performs the scoring to initiate anticoagulation therapy; 1b Who prescribes anticoagulation therapy; 1c Do you know what is the” time in therapeutic range”; 1d What score do you use to assess the bleeding risk; 1e What DOACs regimen do you use most frequently for NVAF treatment; and 1f Do you know about the technique of percutaneous left atrial appendage closure?
DOACS, direct-acting oral anticoagulants; NVAF, nonvalvular atrial fibrillation.
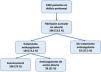
Regarding treatment, 72.5% of the 186 patients with NVAF were receiving OACs (n = 134), of whom 106 (79%) were receiving acenocoumarol and 28 (21%) DOACs. Among the 134 receiving OAC, 41 subjects (21.5%) were treated simultaneously with antiplatelet therapy. A 6% (n = 11) were not taking neither antiplatelet or anticoagulant therapy (Fig. 2).
Distribution of OAC treatment among patients with NVAF. Of the 186 patients with NVAF, 72% were receiving anticoagulation therapy, 72% acenocoumarol and 21% direct-acting oral anticoagulants. Among the 134 who were on OAC therapy, 41 patients (21.5%) were simultaneously receiving antiplatelet therapy. Eleven patients (6%) were not receiving antiplatelet/anticoagulation therapy.
NVAF: non-valvular atrial fibrillation.
Regarding the use of the CHADS2 or CHADS2-VASc scores to calculate the risk of stroke/thromboembolism, 57% of the responders answered that they used them.
However, the evaluation of the score to indicate OAC was performed by the cardiologist in 60% of cases, by the nephrologist in 3%, and jointly in 37% of cases (Table 1 and Fig. 1a). Although, when asked who prescribed OAC, 47% responded that the cardiologist, in 43% it was a shared cardiologist/nephrologist decision and in 10% it was a decision of the nephrologist (Table 1 and Fig. 1b).
Results of the questionnaire answered by the 30 centers.
| Survey questions | Number | Percentage |
|---|---|---|
| Do you use the CHADS score2 or CHA2 DS2 -VASc to estimate the risk of stroke/thromboembolism in your patients with NVAF? | ||
| Yes | 17 | 56,7% |
| No | 13 | 43,3% |
| In your center, who makes the assessment of these scores to initiate anticoagulant treatment? | ||
| Cardiologist | 18 | 60% |
| Nephrologist | 1 | 3,3% |
| Both | 11 | 36,6% |
| In your center, who prescribes the treatment? | ||
| Cardiologist | 14 | 46,7% |
| Nephrologist | 3 | 10% |
| Both | 13 | 43,3% |
| Which of the following scores do you use to assess the risk of bleeding with vitamin K antagonist therapy? | ||
| HAS-BLED | 17 | 56,7% |
| None | 13 | 43,3% |
| Do you know what is “time in therapeutic range” of anticoagulants? | ||
| Yes, I calculate it. | 9 | 30% |
| Yes, but I don't calculate or ask for it. | 16 | 53,3% |
| No | 5 | 16,7% |
| Treatment of AF on PD | ||
| Antiplatelet agents. | 41 | 21,5% |
| Anticoagulation | 134 | 72,6% |
| Untreated | 11 | 6% |
| Patients on VKA. | 106 | 79% |
| Patients with DOACs. | 28 | 21% |
| Apixaban | 24 | 86% |
| Edoxaban | 2 | 7% |
| Dabigatran | 2 | 7% |
| Rivaroxaban | 0 | 0 |
| Which DOAC regimen do you use most frequently? | ||
| Does not use DOAC | 17 | 57% |
| Apixaban 2.5 mg every 12 h. | 9 | 30% |
| Apixaban 5 mg every 12 h. | 1 | 3,3% |
| Edoxaban 30 mg every 24 h. | 2 | 6,6% |
| Dabigatran 150 mg every 12 h. | 1 | 3,3% |
| Are you familiar with the percutaneousleft atrialappendage closure technique? | ||
| Yes | 27 | 90% |
| No | 3 | 10% |
| How many of your patients have undergone percutaneousleft atrialappendage closure? | 17 | 9,13% |
AF, atrial fibrillation; NVAF, nonvalvular atrial fibrillation; VKA, vitamin K antagonists; PD, peritoneal dialysis; DOAC, direct-acting oral anticoagulants; NVAF, nonvalvular atrial fibrillation.
Regarding anticoagulation with VKA, 83% knew what was the time in therapeutic range (TTR), 17% did not know it, but only 30% knew it and was aware of the results (Table 1 and Fig. 1c). Regarding bleeding risk scores, 57% used the HAS-BLED and the rest did not use any (Table 1 and Fig. 1d).
As for the DOACs prescribed, 86% received apixaban, 7% dabigatran, and 7% edoxaban (Table 1). The most frequently used dose was apixaban 2.5 mg/12 h (Table 1 and Fig. 1e).
Regarding percutaneous left atrial appendage closure as an alternative to OAC, 90% of the nephrologists surveyed were aware of the technique, but it had only been performed in 17 patients (9%) with NVAF (Table 1 and Fig. 1f).
In the Appendix, Annex 1 shows the questions asked in the survey and the results of the questionnaire are shown in Table 1 and Fig. 1(a–f). Table 2 shows the prevalence of AF in patients on PD by autonomous community and hospital.
Prevalence of patients with AF on PD by hospital.
| n total | Number of patients with AF | Percentage of patients with AF | |
|---|---|---|---|
| Prevalence of AF in total PD, mean (SD), % | 1.403 | 186 | 13,2% |
| Prevalence of AF in PD by autonomy and hospital. | |||
|---|---|---|---|
| Hospitals | n total | Number of patients with AF | Percentage of patients with AF |
| Valencian Community | 308 | 15,2% | |
| Hospital Clínico Universitario de Valencia | 80 | 19 | 23,8% |
| Hospital Dr. Peset de Valencia | 47 | 11 | 23,4% |
| Hospital General Universitario Valencia | 37 | 1 | 2,7% |
| Hospital Universitario de Torrevieja | 21 | 7 | 33,3% |
| Hospital Lluis Alcanys de Xativa | 26 | 5 | 19,2% |
| Hospital de Gandía | 15 | 2 | 13,3% |
| Hospital General de Elda | 17 | 2 | 11,8% |
| HGU Alicante | 17 | 2 | 11,8% |
| Hospital de Manises | 21 | 2 | 9,5% |
| Hospital Universitario de la Ribera | 27 | 1 | 3,7% |
| Community of Madrid | 214 | 14,3% | |
| Hospital Puerta de Hierro de Madrid | 35 | 9 | 25,7% |
| Hospital Universitario La Paz of Madrid | 55 | 17 | 29,4% |
| Hospital General Universitario Gregorio Marañon | 21 | 2 | 9,5% |
| Doce de Octubre Hospital, Madrid | 43 | 3 | 7% |
| Catalonia | 320 | 13,2% | |
| Hospital Clínic de Barcelona. | 64 | 12 | 18,8% |
| Hospital del Mar de Barcelona | 30 | 9 | 30% |
| Hospital Moisès Broggi de Sant Joan Despí | 17 | 2 | 11,8% |
| Hospital Universitario de Bellvitge | 62 | 4 | 6,5% |
| H. de Terrassa | 32 | 2 | 6,3% |
| H. Josep Trueta of Girona | 83 | 5 | 6% |
| University Hospital Joan XXIII of Tarragona | 32 | 0 | 0% |
| Murcia | 113 | 5,6% | |
| H. Virgen de la Arrixaca | 71 | 8 | 11,3% |
| Hospital General Santa Lucía | 42 | 0 | 0% |
| Balearic Islands | 59 | 25,4% | |
| Hospital Universitario Son de Espases | 59 | 15 | 25,4% |
| Castilla la Mancha | 56 | 5,4% | |
| Complejo Universitario de Albacete | 56 | 3 | 5,4% |
| Basque Country | 48 | 4,2% | |
| Hospital de Basurto | 48 | 2 | 4,2% |
| Asturias | 120 | 12,5% | |
| Central University Hospital of Asturias | 120 | 15 | 12,5% |
| Andalucía | 50 | 20% | |
| Hospital Virgen de la Macarena in Seville | 50 | 10 | 20% |
AF, atrial fibrillation; PD, peritoneal dialysis; SD, standard deviation.
The main finding in the present study was the remarkable prevalence of AF in patients on PD in Spain, a 13.2%. The USRDS data showed a prevalence of 23.3%16 To our knowledge, after the exhaustive literature review, we were unable to find additional studies on the prevalence of NVAF in PD. In our analysis we have obtained a lower overall prevalence, but similar in centers with a higher volume of patients on PD. This could be related to a selection bias in centers with fewer patients (younger subjects or those with fewer comorbidities). This situation highlights the need to generate registries of these subjects in Spain to better understand the prevalence, prognosis and management of this complication, which is common in our PD population.
When analyzing the data obtained from the stroke/thromboembolism risk scores in AF, the CHADS2 or CHA2DS2-VASc were the only ones used to calculate stroke risk. It is striking that, despite the high risk of stroke in these patients, only slightly more than half of the centers use this tool.
It was mainly the cardiologist who indicated the OAC, although the percentage of prescriptions of OAC shared between the nephrologist and the cardiologist was relevant.
Similarly, there was unanimity in the use of HAS-BLED as a score to assess the risk of bleeding with VKA, although it was only calculated in slightly more than half of the centers. Likewise, most hospitals were aware of the existence of the TTR with acenocoumarol or warfarin treatment, although they did not use it, which is relevant given the difficulty of achieving an optimal TTR in this population and its clinical implications.1 In fact, in the study by Phan et al.,19 the mean TTR was 48% and only 10% achieved an optimal TTR > 70%.
Regarding the use of OAC, our results show a high percentage of anticoagulated patients, much higher than the reported by American and Asian studies showing percentages of treatment with OAC between 9% and 28%.16,17,19,20 In addition, these studies also report a greater use of antiplatelet agents as compared to our patients. Similarly, in relation to the prescription of DOACs, Hu et al.16 prescribed apixaban more frequently, although only in 3.4% of their patients, whereas in our analysis DOACs was used in 21% in subjects with OAC.
These results highlight the discrepancies between countries in the perception of the risk-benefit of OAC in dialysis patients in general, and especially in PD. This differences are due, in part, to the discrepant results published18–20 and to the lack of clinical evidence to made recommendations with an acceptable level of evidence. In our study, the assessment of thromboembolic and bleeding risk was mainly made by the cardiologist, who followed the indications of the guidelines for the general population, which could explain the high prescription of OAC in our setting.
Percutaneous left atrial appendage closure as an alternative to OAC for patients with NVAF and high bleeding risk is known to nephrologists (only 3 units were unaware of this procedure). Of the 186 patients with AF on PD, 9% had been treated using this technique. Percutaneous left atrial appendage clossure is a valid alternative to OAC, especially in subjects at high risk of bleeding, such as those with ESRD. The study by Osmancik et al.21 shows that percutaneous left atrial appendage closure is not an inferior technique to OAC in preventing AF-related strokes.21 Studies in dialysis patients suggest that this technique is a valid alternative to OAC also in this population,22–24 although specific studies in people on PD are lacking.
The new guidelines on the diagnosis and management of AF (European Association for Cardio-Thoracic Surgery [EACTS])25 emphasize the lack of studies, controversies, and paucity of evidence-based clinical data so far in this population. Treatment with OACs can be challenging, especially in ESRD, where the net clinical benefit is still unclear and there is a greater need than ever to explore new therapeutic strategies.1
Therefore, there is a need for more training and involvement of the nephrologist in this pathology due to its prevalence and the differential characteristics of these patients with respect to the general population. This is a clear opportunity for improvement in the immediate future.
Although our sample included a significant percentage of patients and PD centers in Spain, the study has several limitations. The main limitation is the validity of the results of a questionnaire, the fact that there is a bias in the participating centers, as well as the global analysis of the patients in a unit instead of individualized analysis, with the consequent lack of variables specific to each individual. However, the lack of updated studies on AF in PD in Europe and, more specifically, in our country, supports the interest of our results, especially since it is a multicenter study that included more than a thousand patients on PD. The surveys were carried out by nephrologists from all the autonomous regions of Spain, and although there was no random sampling for the selection of centers, the number of participants included to achieve the objective of the article is high (n = 1,403) and represents 43% of the subjects on PD in Spain (according to data from the Spanish Registry of Renal Patients [REER] in 2020, there were 3,248 prevalent patients on PD in Spain26). Thus, we have obtained a first picture of the AF patient on PD, which serves as a starting point for the study and approach to a pathology with significant associated morbidity and mortality.
In conclusion, subjects on PD in our country present a notable prevalence of NVAF. Given that this is a pathology whose treatment can have costs for the patient, nephrologists should become involved in its diagnosis, evaluation, and management. The lack of prospective studies and controlled clinical trials in patients on PD should not lead us to therapeutic nihilism. Studies such as the current one allow us to know how the situation is in our units and what are the aspects to be improved in order to offer optimal care to our patients.
FinancingThis work has not received any funding.
Conflict of interestJ.L. Górriz has participated in advisory boards for Boehringer Ingelheim, AstraZeneca, Bayer and Novo Nordisk; he has lectured for AstraZeneca, Boehringer Ingelheim, Esteve, Bayer, Eli Lilly and Company, Astellas and Novo Nordisk and has received research grants from AstraZeneca.
M. Montomoli has participated in Bayer advisory boards; he has given lectures and received research grants from AstraZeneca.
A. Cases reports receiving a grant, consulting and speaking fees from CSL Vifor, speaking and consulting fees from Astellas, Astra Zeneca, Bayer, GSK and Novo Nordisk; consulting fees from Boehringer Ingelheim, Lilly and Otsuka; speaking fees from Amgen, BMS and Sanofi (Mexico) and others from Arbor Research, Astellas, Bayer, Diaverum, Esteve, GSK, Lilly, Novo Nordisk and Sociedad Española de Nefrología, but did not receive funding in connection with the writing of this article.
The rest of the authors declare that they have no conflicts of interest.
The authors would like to thank the Levante Peritoneal Dialysis Registry and the Valencian Society of Nephrology for their financial support for the maintenance of the Levante Peritoneal Dialysis Registry, which has facilitated the extraction of data for this study. We would like to thank all those who collaborated in the completion of the survey.
List of participating researchers: Miguel González Rico, Marco Montomoli, Emilio Sánchez Álvarez, Juan Carlos Quevedo Reina, Isabel García Méndez, Adoración Martínez Losa, Manel Vera Rivera, Inés Rama Arias, María Maldonado Martín, María Antonia Munar Vila, Agustín Ortega Cerrato, Gloria Del Peso Gilsanz, Nuria Aresté Fosalba, Olga González Peña, Sandra Beltrán Catalá, Claudia Yuste Lozano, Diana Manzano Sánchez, Margarita Giménez Edo, José María Portolés Pérez, Merche Prats Valencia, Verónica Duarte Gallego, Francesc Barbosa Puig, José Graña Fandós, Juan Carlos Alonso Gómez, Beatriz Diez Ojea, Almudena Vega Martínez, Eduardo Torregrosa de Juan, Ana Sánchez Escudero, Celia Climent Codina.