Dear Editor,
Urinary infections are common during pregnancy, affecting 10-15% of women. In 1-2.5% of pregnancies there are complications due to acute pyelonephritis1 and the infection is recurrent in up to 10% of women. The development of a kidney abscess secondary to acute pyelonephritis is uncommon during pregnancy. This can affect patients with urinary tract alterations and diagnosis of the condition requires a high index of suspicion and confirmation using ultrasound.2-5 The most common causal agents are enterobacteria. The infection most commonly affects the right kidney (90%), it is usually unilateral and associated with high morbidity, which is why early diagnosis and treatment are necessary.1,2-4
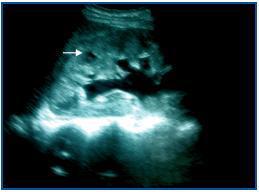
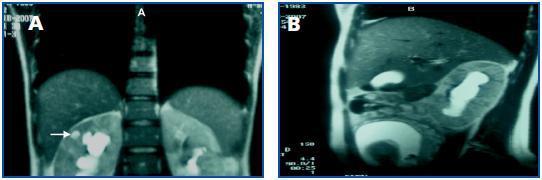
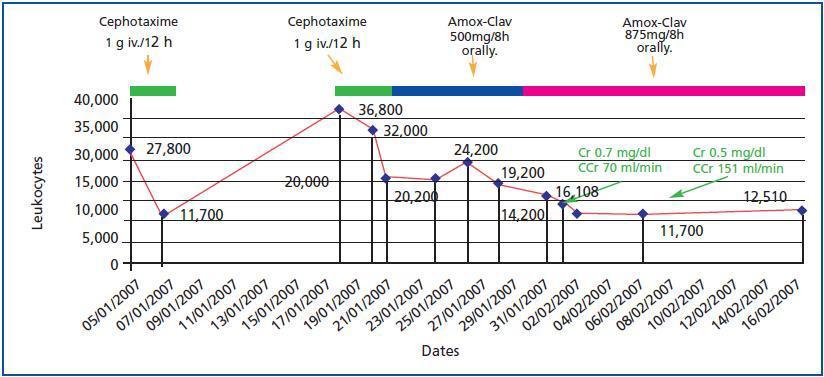
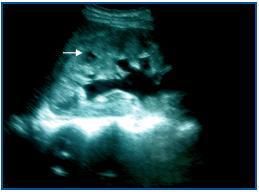
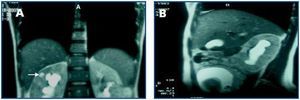
This is the case of a 23-year-old woman with a history of repeated urinary tract infections since the age of 16. In 2005 she miscarried at 12 weeks and this coincided with a urinary infection caused by Escherichia coli. In November 2006 when she was 12 weeks pregnant, the following results were obtained from a urine test: pH 7.5, nitrites (+), leukocytes (++). Sediment: leukocytes 20-40 per field and abundant bacteria. No treatment was prescribed. On 4 January 2007 when she was 20 weeks pregnant, she had a fever of 39º C and pain in the right renal fossa. The biochemistry showed: leukocytes 27,800/mm3 (85% neutrophils), Hb 8.7g/dl, platelets 288,000/mm3 and GSV 16-39mm/h. Other data: Na 138mmol/l, K 4.8mmol/l, Cl 96mmol/l, glucose 66mg/dl, urea 48mg/dl, creatinine 0.7mg/dl, uric acid 3.4mg/dl and CRP 31mg/dl. Urine: blood 25/ml, nitrites (+), leukocytes 100/ml. Sediment: leukocytes 31-50 per field, isolated red blood cells and abundant bacteria. Urine culture: Escherichia coli. She received 1g/12 hours of intravenous cefotaxim treatment for four days. The fever disappeared after 48 hours and there were improvements in her clinical condition and test results. On 18 January 2007, in the 22nd week of pregnancy, she was admitted into hospital again with the same symptoms. The biochemistry showed: leukocytes 36,800/mm3 (91% neutrophils), Hb 8.4g/dl, platelets 357,000/mm3. Urine: leukocytes (+++), proteinuria (++), urea 55mg/dl, creatinine 1.2mg/dl, total proteins 5.1g/dl and CRP 69mg/dl. The ultrasound showed: the right kidney increased in size (14cm larger in diameter), with a reduction in the corticomedullary differentiation and a hypoecogenic image of 8mm at cortical level in the upper pole, with echogenic content that was suggestive of a corticomedullary abscess, moderate dilatation of the calyx, pelvis and proximal ureter (figure 1). The major axis of the left kidney measured 12.7cm, echogenicity was normal and there was mild pyelocalceal dilatation. The patient was first administered treatment with amoxicillin clavulanate 500mg/8 hours, and then 850/125mg/8 hours; after 48 hours her fever subsided and her symptoms improved. Nine days after the first ultrasound, a second one was carried out which continued to show the image of the abscess in the right kidney. On 8 February 2007, when she was 24 weeks pregnant a MRI scan showed bilateral pyeloureteral dilatation that was greater on the right side, with blunting of the calyceal fornices and a renal pelvis measuring 2.8cm. The right kidney was enlarged with deteriorated corticomedullary differentiation. There was a hyperintense image 8-10mm in diameter in the upper pole around the corticomedullary area, which seemed to be a parenchymatous abscess (figure 2). Treatment using amoxillin clavulanate 875/125mg/8 hours was administered for three weeks. The clinical progress made by the patient was favourable and leukocyte levels were normalised (figure 3). After two weeks, a new MRI scan showed a microabscess which was 15mm in diameter and a renal pelvis of 3cm. In a new ultrasound scan carried out three weeks later, the lesion had decreased in size. Antibiotic therapy continued (oral amoxicillin clavulanate) for two more weeks until the five week course of treatment was completed. Regular ultrasound scans detected the ongoing presence of the abscess which is why patient treatment was switched to phosphomycin 500mg/8 hours for three weeks (from 7 to 28 March). The patient continued to go for check ups at the GP¿s and a new MRI scan showed the presence of lesions. The patient was then admitted into hospital once again. On admission the following results were obtained: leukocytes 15,700 (neutrophils 74.5%) and urine sediment with 20-30 leukocytes per field. She was then administered cefotaxim 2g/8 hours for five weeks. On 4 May when she was 38 weeks pregnant, labour was induced, resulting in a live birth (weight 2.94kg) without complications. A new control MRI scan was carried out a week after delivery which showed the renal abscess in the right kidney and its content. The patient was referred to the Urology Department so vesicoureteral reflux tests could be carried out and in order to check that the patient had recovered. The tests indicated that the abscess had disappeared.
Pregnant women have a higher risk of suffering from urinary infections,1 however, the development of acute pyelonephritis with a renal abscess is an extremely rare complication2-4 that is challenging in terms of treatment.
The diagnosis of a kidney infection is fundamentally based on symptoms like fever, shivering and side pain,6,7 by means of imaging techniques. The technique of choice during pregnancy is the ultrasound. Segmentary pyelonephritis (lobar nephronia) appears in the ultrasound as a solid oval-shaped mass with edges that are not clearly defined, whereas an abscess appears as clearly identifiable mass that is similar to a cyst. The presence of internal echoes or layers of cellular debris within a well defined mass with an irregular internal wall suggests an abscess.6,7 For patients who are not pregnant a CT scan is the method of choice for detecting acute pyelonephritis and/or a renal abscess.8-10A renal abscess appears in a CT scan as a mass that does not contrast, with a swollen, irregular wall, which could present liquid and cellular detritus inside, as well as internal septa. Since the MRI scan avoids the use of ionising radiation, it is an imaging technique which is used extensively in obstetrics.11-13 Until now only one case involving a pregnant patient with a renal cortical abscess detected using MRI had been published.2 In MRI scans the renal abscess has the appearance of a rounded lesion with a swollen wall, which has a low signal intensity that is not homogeneous on the T1 weighted image and increasing signal intensity on the T2 weighted image. We were also able to observe the presence of liquid with detritus. Furthermore, the MRI can accurately show the level of obstruction in the urinary tract or any other anomalies like vesicoureteral reflux that may be present during the pregnancy. Although gadolinium is contraindicated during the first trimester of pregnancy, it can be used during the second and third trimesters in order to investigate foetal and placental anomalies that are not clearly defined in an ultrasound scan.11,14 Acortical renal abscess is associated with a mortality rate of 1.5-15%. Therefore, treatment should be aggressive and based on combining intensive antibiotic therapy with percutaneous drainage or surgery.3 With ultrasound and MRI scans being used more frequently, the availability of more powerful antibiotics and better support measures are in place, in many cases medical treatment is a viable alternative to surgery.3,7,9 Prolonged antibiotic treatment has a more beneficial effect on reducing morbidity and preserving renal mass and function.7,9 Our patient presented the three key symptoms: fever, side pain and pyuria, which is characteristic of an upper urinary tract infection. In this case, apart from urinary stasis and hydronephrosis caused by the pregnancy,5 there were other factors that favoured the condition like previous urinary tract infections and vesicoureteral reflux. The ultrasound and MRI scan made an early diagnosis possible, showing the presence of a renal corticomedullary abscess and dilatation of the upper urinary tract. Close monitoring of lesions using regular ultrasound and MRI scans and ongoing, rotated antibiotic treatment made it possible to successfully bring the pregnancy to term without having to resort to surgical drainage.
In summary, we have described an exceptional case of a women who was 24 weeks pregnant who presented acute pyelonephritis caused by Escherichia coli, which was further complicated by a corticomedullary renal abscess. The diagnosis was confirmed using ultrasound and MRI scans. The ongoing antibiotic treatment made it possible to keep the pregnancy and bring it to term in the 38th week, resulting in a normal live birth. The patient also made a full recovery without having to resort to percutaneous drainage. This case highlights that MRI scans can be useful for detecting specific urological problems like a complicated case of pyelonephritis with a renal abscess, hydronephrosis and vesicoureteral reflux. Given the favourable prognosis for mother and foetus, this case also shows that conservative medical treatment is a viable alternative to surgery.
Figure 1.
Figure 2.
Figure 3.