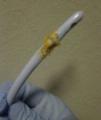
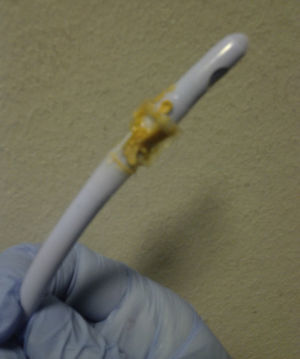
Struvite urolithiasis is an uncommon clinical scenario, usually associated with urinary infections caused by urease-positive organisms and with renal transplant,1 which requires a high degree of clinical suspicion and microbiological collaboration for its diagnosis. We describe the case of a 76-year-old man with a past medical history of COPD, cor pulmonale, previous ischaemic stroke, and multiple admissions for respiratory infections, requiring prolonged antibiotic therapy. He had an indwelling urinary catheter for prostatic obstructive uropathy, and regular medications were acenocoumarol, inhaled beta-agonists, furosemide, and dutasteride-tamsulosin. In the previous 3 months he had had recurrent urinary infections caused by various bacteria, with an acidic urinary pH, and had been treated with quinolones and beta-lactams. He began attending the emergency room repeatedly with catheter obstruction. Urine was turbid, thick, and milky, with an ammoniacal odour. Standard urine culture and urine mycobacteria and fungus culture were repeatedly negative. Despite changing the catheter, several oral antibiotic regimens and nightly antibiotic prophylaxis, the problem persisted, with progressively alkalotic urine and a sediment with magnesium ammonium phosphate crystals. During one of these episodes, on removing the catheter, we observed a petrous material in the form of orange-brown hexagonal crystals (Figs. 1 and 2) that was subsequently identified as struvite. Urine culture was repeated, and grew a Corynebacterium urealyticum (CU) sensitive to glycopeptides. It was treated with teicoplanin for 15 days with good clinical resolution.
CU is a strictly aerobic diphtheriform Gram-positive coccobacillus, and was characterised between 1985 and 1992.2 Initially, it was called coryneform D2. It is a common inhabitant of skin and mucous membranes, mainly in the perigenital region of women. It can be isolated from fomites and in the air of rooms of colonised individuals. It acts as an opportunistic organism in the urinary tract and infects from a heavy inoculum and by antibiotic selection, facilitated by interventions that allow it to penetrate (such as urinary catheterisation, cystoscopy, surgery, or renal transplant). It is characterised by having a urease gene with no repressor, the ability to synthesise proteinaceous pili and biofilms, and to acquire resistance to multiple antibiotics genetically (macrolides, lincosamides, ketolides, chloramphenicol, tetracycline, streptomycin and other AMGs), and by DNA gyrase mutations (to beta-lactams and quinolones). It causes cystitis, pyelonephritis, and encrusted cystitis that in transplants can result in encrusted pyelitis and graft loss. Less often, it can lead to endocarditis, soft tissue infections, and osteomyelitis. It does not grow in normal media, therefore a prolonged incubation time and use of enriched media are recommended (Blood agar at 35°C, chocolate agar, CLED, MacClonkey agar). It should be suspected when faced with the clinical picture of urinary infection with alkaline pH urine, magnesium ammonium phosphate crystals (struvite) in the sediment, and recurrent urinary retention. It is usually resistant to beta-lactams, aminoglycosides and quinolones, and sensitive to vancomycin and teicoplanin (sensitive in vitro to Synercid®, linezolid, and glycylcyclines). Treatment requires removal and de-encrustation of foreign bodies (such as catheters or cystocopes) and urine should be acidified, for which acetohydroxamic acid (Uronefrex®), vitamin C, fucidic acid, citric acid, and bladder irrigation using citric acid with glucono-delta-lactone and magnesium carbonate (Renacidin®) are all useful.
In the literature we find mainly isolated cases3–6 and a review of 163 transplant patients1 in which 9.8% of positive cultures were attributed to CU. The pathogenesis is explained,7 beginning with a prolonged inflammation that induces stimulation of cytokines and growth factors in the bladder, with the consequent activation of smooth muscle cells, endothelial cells, and pericytes that differentiate into osteoblasts capable of generating bone (calcium, hydroxyapatite, and collagen) on stimulation of calcification regulatory proteins. The apoptotic remains of the damaged cells act as crystallisation nuclei and the alkaline pH allows precipitation of crystals. The mechanism can be blocked with appropriate antibiotic treatment and accelerated with vitamin K inhibitors, as osteocalcin, essential for the calcification process, is vitamin K-dependent. Therefore, acenocoumarol would induce osteocalcin overexpression, representing an added risk factor.
Our case was contracted due to the presence of a petrous material, made of hexagonal crystals that repeatedly obstructed the urinary catheter as can be seen in the figures.
Please cite this article as: Martín-Navarro JA, Petkov-Stoyanov V, Gutiérrez-Sánchez MJ, Gordo-Flores ME. Urolitiasis por estruvita en infección por Corynebacterium urealyticum. A propósito de un caso. Nefrologia. 2015;35:410–411.