We present the case of a 40-year-old woman, with symptomatic hypokalemia.
She had been previously healthy up to 2016 when an axillary lymph node revealed the diagnosis of metastatic melanoma (of unknown primary). She maintains active surveillance at oncology consult. Aside from axillary-drainage she had no other directed treatment. Since the oncologic diagnosis she adhered to a strict diet (Table 1) and physical-workout regimen.
Diet and nutritional assessment.
| Diet | |
| Breakfast | Juice containing:Maca fruit (Lepidium meyenii, sometimes referred to as peruvian ginseng), guarana (Paullinia cupana), beetroot, roseseed, baobab (Adansonia), açai, lemon |
| Midmorning | Whey protein pudin, banana, juice of ginger |
| Late morning | Two eggs, two pieces of fruit, matcha tea |
| Lunch | One of the following:Pie of broccoli, mushroom, tuna fish and eggGrilled fish with vegetables and potatoEggs (3) and cooked broccoliGrilled chicken with salted vegetables and integral riceTuna with couscous and salad |
| Afternoon | Coffee with cardamom and two pieces of fruit |
| Dinner | Two slices of melon or watermelon, hemp seeds |
| Supper | Yoghurt (skyr or kefir) with two scoops of casein, cinnamon, avocado and hemp seeds; cooked fish with vegetables |
| Supplements | Vitamin D, omega 3/6/9, vitamin E supplements |
| Nutritional assessment | |
| Calories | 2153kcal/d (39.9kcal/kg/d) |
| Protein | 190g/d (3.5g/kg/d) |
| Sodium | 1076mg/d (46.8mEq Na or 2.5g of salt) |
| Potassium | K 5390mg/d or 138mEq/d, not accounting for K supplementation (pills) |
| Acid load | Potential renal acid load: −6.69mEq/dOrganic acids: 40.17mEq/dNet acid excretion: 33.48mEq/d |
Family history is significant for kidney stone disease, and cancer (mother had gallbladder adenoma, grandfather had lung and prostate cancers).
Three-years later she starts feeling tired, sad, and with discrete memory-impairment which was associated with increased workload and reactive-depression.
A routine bloodwork revealed serum hypokalemia (K 2.6mmol/L) and metabolic alkalosis with alkalemia (pH 7.56, HCO3 35mmol/L). She was referred to the emergency-department for initial study and treatment. She was normotensive and physical-examination was unimpressive aside from discrete proximal-muscle weakness. Kidney function and remaining electrolyte-panel were normal. EKG showed no alterations.
She was discharged on oral potassium supplements and referred to nephrology consult. At first-consult she was normokalemic on 3 potassium pills a day (8-mEq each). She denied vomiting or diuretic use. Her blood-pressure was normal. There were no relevant physical-examination alterations including neurologic exam, skin-changes, dental erosion, enlarged parotid-glands, calluses, or scars on the knuckles. Menstrual history was unremarkable.
Nutritional-assessment revealed appropriate caloric and protein intake, with a potassium rich, alkaline, low-sodium diet (Table 1). She was underweight (BMI 17.6kg/m2).
Her physical activity's program included weightlifting 1h 15 daily, fast-walk 10-km daily and Pilates twice weekly.
She was instructed to stop potassium-supplementation for 48h for a repeat blood and urine work-up. Her symptoms restarted with accompanying hypokalemia and metabolic alkalosis. Her renal function, sodium and magnesium levels were normal. There was an increased urine potassium-to-creatinine ratio, low-chloride concentration, low calcium-to-creatinine ratio, and high sodium-to-chloride ratio. 24h-urine collection showed low-sodium excretion (Table 2).
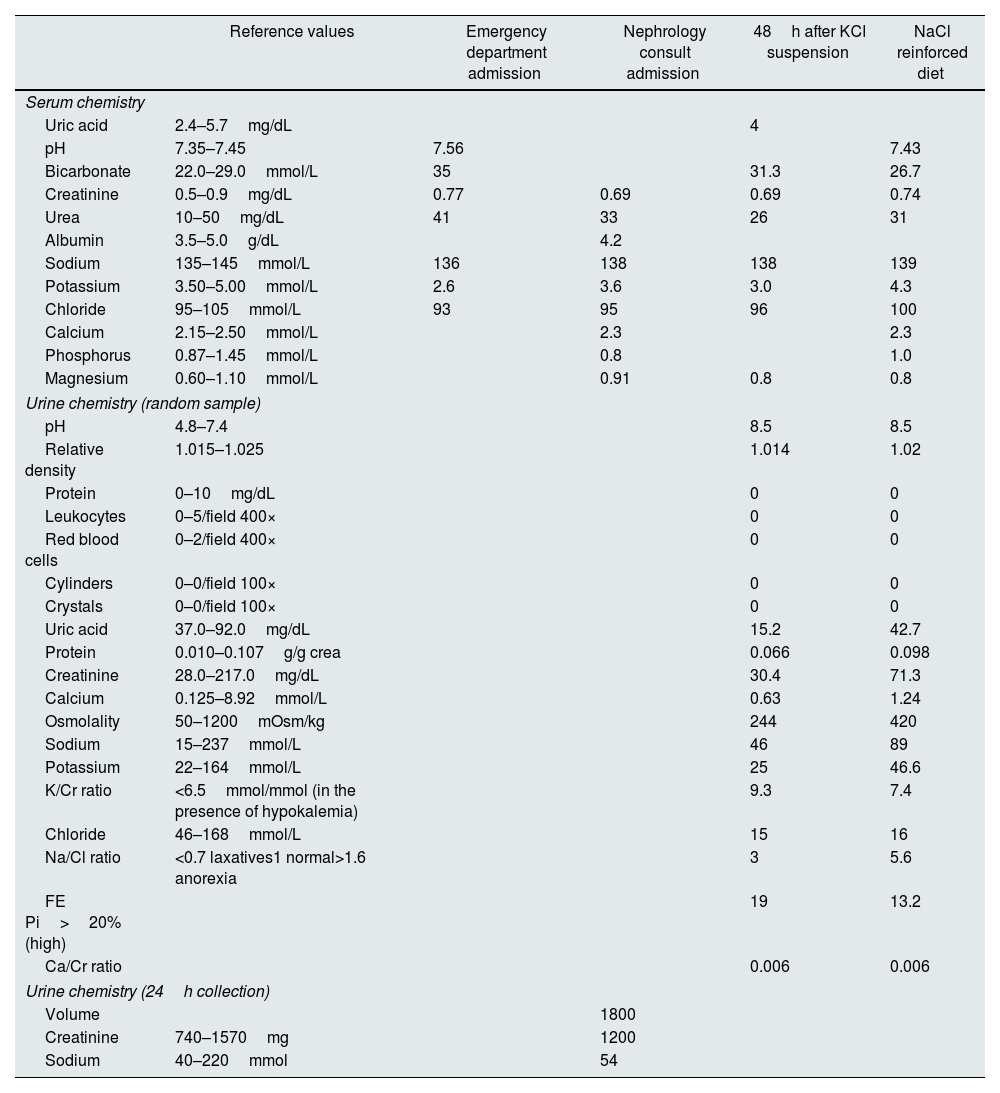
Laboratory results at emergency department, first consult (on KCl supplementation), 48h after KCl suspension, and on NaCl reinforced diet.
| Reference values | Emergency department admission | Nephrology consult admission | 48h after KCl suspension | NaCl reinforced diet | |
|---|---|---|---|---|---|
| Serum chemistry | |||||
| Uric acid | 2.4–5.7mg/dL | 4 | |||
| pH | 7.35–7.45 | 7.56 | 7.43 | ||
| Bicarbonate | 22.0–29.0mmol/L | 35 | 31.3 | 26.7 | |
| Creatinine | 0.5–0.9mg/dL | 0.77 | 0.69 | 0.69 | 0.74 |
| Urea | 10–50mg/dL | 41 | 33 | 26 | 31 |
| Albumin | 3.5–5.0g/dL | 4.2 | |||
| Sodium | 135–145mmol/L | 136 | 138 | 138 | 139 |
| Potassium | 3.50–5.00mmol/L | 2.6 | 3.6 | 3.0 | 4.3 |
| Chloride | 95–105mmol/L | 93 | 95 | 96 | 100 |
| Calcium | 2.15–2.50mmol/L | 2.3 | 2.3 | ||
| Phosphorus | 0.87–1.45mmol/L | 0.8 | 1.0 | ||
| Magnesium | 0.60–1.10mmol/L | 0.91 | 0.8 | 0.8 | |
| Urine chemistry (random sample) | |||||
| pH | 4.8–7.4 | 8.5 | 8.5 | ||
| Relative density | 1.015–1.025 | 1.014 | 1.02 | ||
| Protein | 0–10mg/dL | 0 | 0 | ||
| Leukocytes | 0–5/field 400× | 0 | 0 | ||
| Red blood cells | 0–2/field 400× | 0 | 0 | ||
| Cylinders | 0–0/field 100× | 0 | 0 | ||
| Crystals | 0–0/field 100× | 0 | 0 | ||
| Uric acid | 37.0–92.0mg/dL | 15.2 | 42.7 | ||
| Protein | 0.010–0.107g/g crea | 0.066 | 0.098 | ||
| Creatinine | 28.0–217.0mg/dL | 30.4 | 71.3 | ||
| Calcium | 0.125–8.92mmol/L | 0.63 | 1.24 | ||
| Osmolality | 50–1200mOsm/kg | 244 | 420 | ||
| Sodium | 15–237mmol/L | 46 | 89 | ||
| Potassium | 22–164mmol/L | 25 | 46.6 | ||
| K/Cr ratio | <6.5mmol/mmol (in the presence of hypokalemia) | 9.3 | 7.4 | ||
| Chloride | 46–168mmol/L | 15 | 16 | ||
| Na/Cl ratio | <0.7 laxatives1 normal>1.6 anorexia | 3 | 5.6 | ||
| FE Pi>20% (high) | 19 | 13.2 | |||
| Ca/Cr ratio | 0.006 | 0.006 | |||
| Urine chemistry (24h collection) | |||||
| Volume | 1800 | ||||
| Creatinine | 740–1570mg | 1200 | |||
| Sodium | 40–220mmol | 54 | |||
At the emergency department the patient presents with symptomatic hypokalemia and metabolic alkalosis; she is discharged after electrolyte correction and referred to nephrology consult. At first consult the patient is normokalemic and presents a low 24h urinary Na content. 48h after KCl supplementation suspension, symptoms and electrolyte abnormalities return: the patient presents with metabolic alkalosis, hypokalemia and urinary abnormalities compatible with a vomiting induced picture (high K/Cr ratio, low chloride concentration, high Na/Cl ratio). The electrolyte and acid–base disturbances were corrected after reinforcement of salt in diet (NaCl reinforced diet).
We hypothesized that the primary disturbance maintaining metabolic-alkalosis and hypokalemia was chloride-depletion. The patient was instructed to replace potassium-supplements (KCl) for table salt (NaCl) and was reassessed 48h later. She responded favorably, with clinical and analytical resolution.
Normal blood pressure, hypokalemia with increased urinary excretion, and metabolic alkalosis in a young adult woman with dietary and physical priorities is concerning for vomits or diuretic abuse which can be surreptitious. The critical interpretation of the concentrations of sodium, potassium, and chloride in the plasma and urine can help establish the correct diagnosis. In diuretic abuse the pattern is of increased urinary sodium and chloride while the diuretic is acting. When the effect abates, the concentration falls, reflective of extracellular volume contraction. Distinguishing between loop and thiazide diuretics can be accomplished by calcium excretion determination (high in loop diuretics); direct measure of diuretics in the urine can also be performed. Our patient's urinary chemical profile is not suggestive of active diuretic activity. Remote diuretic use could potentially be the cause of this clinical picture. Some ingredients in her diet have been associated with diuretic-like properties namely lemon, ginger, and guarana. Her urine electrolyte panel is most characteristic for vomiting, which the patient persistently denied. Although neither of this hypothesis can be excluded, her clinical history raises an alternative diagnosis.
Since the oncologic diagnosis our patient was attentive to what she ate and how she lived, embarking on a significant lifestyle change. The net effect of vomiting is the loss of chloride and the gain of bicarbonate in the plasma. The ensuing bicarbonaturia obligates the excretion of sodium and potassium and, hence, a decline in the effective intravascular volume and hypokalemia.
In this case, a conjugation of factors are working together to produce an acid–base and electrolyte disturbance similar to vomiting: (1) intense physical-activity induces chloride and potassium loss through sweat, extracellular volume contraction with a salt-avid reabsortive state; (2) alkaline-diet induces high rate excretion of organic-anions and bicarbonate that obligates sodium and potassium loss (mainly potassium due to the low-sodium content in diet); (3) low-sodium diet (and low-chloride diet) limits chloride delivery to the distal-tubule, interfering with the activity of beta-intercalated cells (through pendrin channels) to promote HCO3− excretion.
Pendrin is an important regulatory transporter in the cortical collecting ducts, whose main stimuli are distal chloride delivery and intracellular pH. Reduced chloride delivery to the cortical collecting ducts impedes bicarbonate excretion and causes sodium conservation to be more dependent on ENaC which may explain the high doses of urinary potassium excretion. Also, pendrin is reduced in potassium depletion.1–4 This alternative explanation is physiologically feasible, and a similar explanation has been proposed in previous case reports.2,5–8 Chloride depletion alkalosis can be corrected by selective chloride repletion despite sodium or potassium negative balance.2 The maintenance of normokalemia after transition from KCl to NaCl supports this hypothesis.
In conclusion, not all normotensive hypokalemic metabolic alkalosis with increased urinary K/Cr ratio and low chloride excretion are due to vomiting. A vegetable-based, low-sodium diet associated with intense physical-activity may simulate electrolyte and acid–base disturbances similar to vomiting induced hypokalemic metabolic alkalosis.
FundingNone.
Authors’ contributionsJoão Oliveira, M.D., Joana Freitas, M.D., Inês Sala, M.D. were involved in the care and treatment of the patient. João Oliveira, M.D. was responsible for writing and submitting the manuscript. Sofia Santos, M.D., António Cabrita, M.D., supervision of care and submission of manuscript.
Availability of data and material (data transparency)Yes.
Conflicts of interestOn behalf of all authors, the corresponding author states that there is no conflict of interest.