Obesity is a risk factor for incident chronic kidney disease (CKD). C1q/TNF related protein 3 (CTRP3) is an adipokine with multiple effects and may modulate the association between obesity and vascular diseases. The aim of the study is to explore potential links between obesity, CTRP3 levels and CKD progression.
MethodsPatients with stage 3 and 4 CKD without previous cardiovascular events were enrolled and divided into groups according to body mass index (BMI) and sex. Demographic, clinical, analytical data and CTRP3 levels were collected at baseline. During follow-up, renal events (defined as dialysis initiation, serum creatinine doubling or a 50% decrease in estimated glomerular filtration rate were registered).
Results81 patients were enrolled. 27 were obese and 54 non-obese. Baseline CTRP3 was similar between both groups (90.1±23.8 vs 84.5±6.2; p=0.28). Of the sum, 54 were men and 27 women, with higher CTRP3 in women (81.4±24.7 vs 106±24.7;p<0.01). During a mean follow-up of 68 months, 15 patients had a renal event. Patients in the higher CTRP3 tertile had less events but without statistical significance (p=0.07). Obese patients in the higher CTRP3 tertile significantly had less renal events (p=0.049). By multiple regression analysis CTRP3 levels could not predict renal events (HR 0.98; CI95% 0.96–1.06).
ConclusionsCTRP3 levels are higher in woman than men in patients with CKD, with similar levels between obese and non obese. Higher CTRP3 levels at baseline were associated with better renal outcomes in obese patients.
La obesidad es un factor de riesgo de la enfermedad renal crónica (ERC) incidente. La proteína 3 relacionada con C1q/TNF (CTRP3) es una adipoquina que puede modular la asociación entre obesidad y enfermedades vasculares. El objetivo del estudio es explorar los posibles vínculos entre obesidad, CTRP3 y progresión de ERC.
MétodosPacientes con ERC estadio 3 y 4 sin eventos cardiovasculares previos fueron reclutados y divididos según el índice de masa corporal y sexo. Los datos demográficos, clínicos, analíticos y los niveles de CTRP3 se recopilaron basalmente. Durante el seguimiento se registraron eventos renales (inicio de diálisis, duplicación de la creatinina o una disminución del 50% en la filtración glomerular estimada).
ResultadosSe reclutaron 81 pacientes, 27 obesos y 54 no obesos. LA CTRP3 inicial fue similar en ambos grupos (90,1±23,8 vs. 84,5±6,2; p=0,28). Del total, 54 eran varones y 27 mujeres, con mayor CTRP3 en mujeres (81,4±24,7 vs. 106±24,7; p<0,01). Durante un seguimiento medio de 68 meses, 15 pacientes sufrieron un evento renal. Los pacientes en el tercil superior de CTRP3 tuvieron menos eventos, pero sin significación estadística (p=0,07). Los pacientes obesos en el tercil superior de CTRP3 tuvieron significativamente menos eventos renales (p=0,049). Por análisis de regresión múltiple, los niveles de CTRP3 no pudieron predecir eventos renales (HR: 0,98; IC 95%: 0,96-1,06).
ConclusionesLos niveles de CTRP3 son más altos en mujeres que en varones en pacientes con ERC, con niveles similares entre obesos y no obesos. Valores iniciales mayores de CTRP3 se asociaron con mejores resultados renales en pacientes obesos.
Obesity is a disease whose prevalence has been constantly increasing in recent decades1 and which represents an enormous healthcare and economic burden for the health systems due to its association with cardiovascular,2 endocrine,3 psychological,4 renal diseases,5–7 etc.
The association between obesity and kidney disease is complex, multifactorial, and not fully understood. There is a clear indirect damage of obesity on the kidney through the development of known nephropathy risk factors such as hypertension (HTN) and diabetes mellitus (DM).7 Obesity also impacts directly the kidney through hemodynamic changes (such as hyperfiltration and hyperactivation of the renin–angiotensin–aldosterone system) and by a specific obesity inflammatory/hormonal state, defining a specific renal pathology named as “obesity-related glomerulopathy”.8–10
The aforementioned inflammatory/hormonal state is due to the secretion of adipokines, like adiponectin, resistin or leptin,11 converting the adipose tissue into an endocrine organ rather than a mere “energy storage”. A new family of adipokines structurally similar to adiponectin has recently been discovered, the C1q/TNF related proteins (CTRPs).12,13 Among them, CTRP3 is an adipokine with multiple metabolic and anti-inflammatory effects.13–15 Lower levels of CTRP3 have been described in patients with DM and in obese patients, as well as higher levels in women,14,16–18 although some results are contradictory.
Studies of CTRP3 in kidney diseases are scarce. There are in vitro studies with positive results on the anti-inflammatory effect of CTRP3 in diabetic nephropathy19 and IgA nephropathy,20 as well as studies of CTRP3 levels in patients with diabetic nephropathy21 and according to the degree of chronic kidney disease (CKD).22 There are currently no studies of CTRP3 and its impact on renal prognosis.
We present an observational study in patients with CKD on the association of CTRP3 levels with anthropometric values and with the risk of developing long-term renal events.
MethodsThis is an observational study enrolling patients without previous cardiovascular disease (CVD) who had Stage 3 or 4 CKD [estimated glomerular filtration rate (eGFR) between 60 and 15mL/min/1.73m2 of body surface area], according to the four-variable Modification of Diet in Renal Disease (MDRD4) equation, who participated in the Effect of Aspirin in Primary Prevention of Cardiovascular Risk in Patients With Chronic Kidney Disease (AASER)23 study [clinical trial (ClinicalTrials.gov Identifier: NCT01709994)]. Inclusion and exclusion criteria are listed below:
Inclusion criteria- •
Signed informed consent.
- •
Age: Males 45–79 years or females 55–79 years.
- •
CKD stage 3 or 4.
- •
A previous cardiovascular event: cardiac arrhythmias, cardiac arrest, angina or acute myocardial infarction, stroke, carotid stenosis of more than 50%, documented peripheral vascular arteriopathy.
- •
Hospitalization for any cause in the three months prior to inclusion in the study.
- •
Allergy to acetyl-salicylic acid.
- •
Coagulopathy from any cause.
- •
Thrombocytopenia<150,000 platelets.
- •
Liver disease from any cause.
- •
Infection by hepatitis B virus, hepatitis C or HIV.
- •
Immunosuppressive treatment within 12 weeks before inclusion in the study.
A total of 81 patients were included in the study: 22 stage 3a (eGFR 45–59mL/min/1.73m2), 39 stage 3b (eGFR 30–44mL/min/1.73m2) and 20 Stage 4 (15–29mL/min/1.73m2).
Visits were performed every 6 months, and the following data were recorded in all participants (at every visit):
- -
Medical history including data on cardiovascular risk factors.
- -
Concomitant medication: renin–angiotensin system blockers, antidiabetics, statins and allopurinol. The dosage these drugs were adjusted following the Kidney Disease: Improving Global Outcomes guidelines. Changes in the dosage or choice of drug were not recorded during the follow-up.
- -
Laboratory data: serum creatinine, eGFR, lipid profile, uric acid, glycated haemoglobin, erythrocyte sedimentation rate (ESR), high sensitivity C-reactive protein (hsCRP), urine albumin-to-creatinine ratio (uACR).
The following laboratory data were only measured at baseline:
- -
Anthropometric/clinical data: age, gender, height, weight, body mass index (BMI), systolic and diastolic blood pressure, and heart rate;
- -
CTRP3
CTRP3 concentrations were measured in plasma samples using a commercially available ELISA kit (R&D Systems) according to manufacturer's protocol and are expressed in ng/ml. Plasma hsCRP was measured using a latex-based turbidimetric immunoassay on a Hitachi analyser. For the rest of laboratory parameters standard laboratory assays were used.
Renal event was defined as doubling of serum creatinine, an eGFR decrease 50% or initiation of renal replacement therapy. The researchers adjudicated renal events according to clinical documentation.
The study was approved by the local Ethics Committees in accordance with the Declaration of Helsinki and all patients provided written informed consent.
Statistical analysisAll statistical analyses were performed using IBM SPSS, version 21.0 (IBM Corp., Armonk, NY, USA) for Windows. Values are expressed as mean (± standard deviation). Participants were categorized by baseline BMI as non-obese (<30kg/m2) and obese patients (≥30kg/m2) and by sex (men/women). Differences between groups were analysed using the Mann–Whitney test.
Subcategorization according to baseline BMI was performed and definend as normal-weight (BMI<25kg/m2), overweight (BMI 25–29.99kg/m2) and obese (BMI≥30kg/m2). Differences between these groups were analysed using the Kruskal–Wallis test. Kaplan–Meier curves and the log-rank test were used to analyse renal survival. For the exploratory survival analysis, the patients were divided into two groups based on the tertiles of CTRP3 levels: the highest tertile (T3) was compared with the other tertiles (T1&T2). Cox proportional hazard models were used to evaluate the risk of renal events, and the results were adjusted for age, eGFR, uACR. Statistical significance is defined as a two-tailed P<0.05
ResultsA total of 81 patients from the AASER23 study were included in the analysis of CTRP3 and its correlation with CKD progression. The first analysis was performed by categorizing according to baseline BMI in obese (BMI≥30kg/m2) (n=38) and non-obese (BMI<30kg/m2) (n=53). Obese patients presented higher SBP (p=0.01), uric acid (p=0.003) and CRP (0.02). The CTRP3 levels were similar between both groups (90.1±23.8 vs 84.5±6.2; p=0.28). Both groups presented similar baseline levels of creatinine, eGFR, lipid profile, albuminuria, and ESR (p>0.05).
Since the mean BMI in the non-obese groups tended to be >26kg/m2 a new subcaterogization was performed in three groups: normal weight (NW) (BMI<26kg/m2; n=16), overweight (OW) (BMI 26–29.99kg/m2; n=37) and obese (OB) (BMI≥30kg/m2; n=28). CTRP3 levels in these subgroups were comparable (NW 87.8±31.5 vs OW 88.1v25.8 vs OB 94.3±26.5; p=0.13).
Categorization according to BMI was carried out in the men subgroup (n=54; 14 obese and 40 non-obese) and in the women subgroup (n=27; 14 obese and 13 non-obese). CTRP3 levels were similar between obese and non-obese in both subgroups (p>0.05) as well as creatinine, eGFR, lipid profile, albuminuria and ESR (p>0.05).
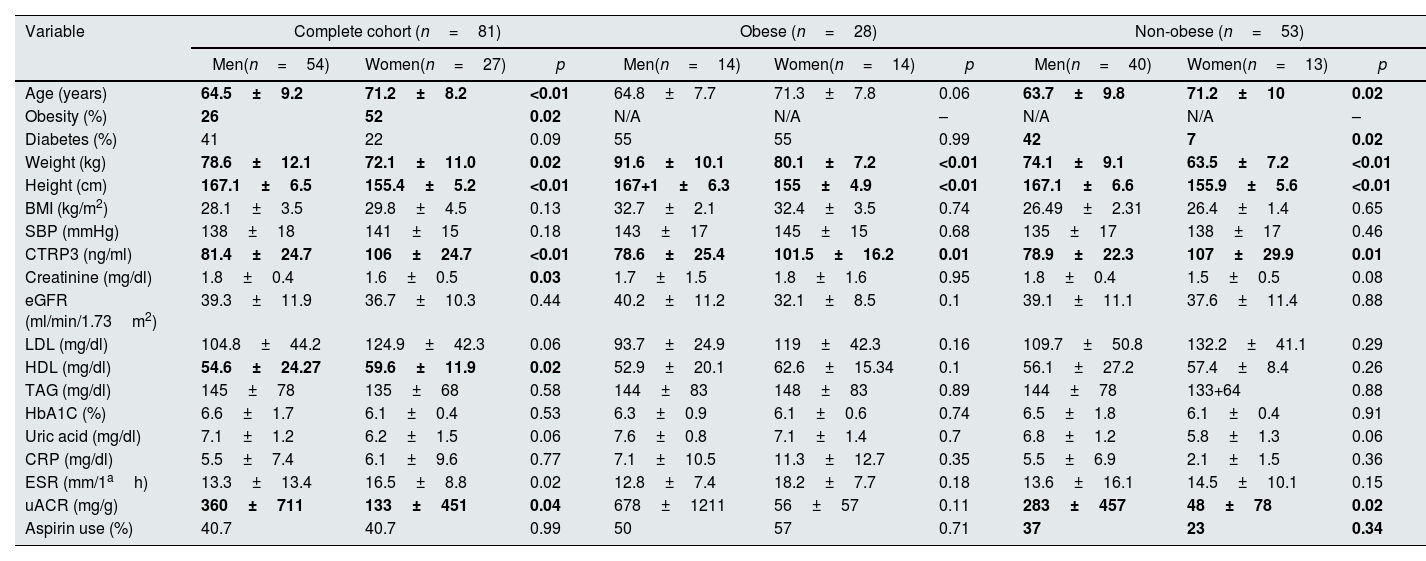
Next, the process was carried out reversely, categorizing firstly according to sex (men, women) and secondly according to BMI status. Women resulted to be older (p<0.01), have lower weight (p=0.02) without differences in BMI (p=0.29), had lower levels of albuminuria (p=0.04) and higher HDL (p=0.02). CTRP3 levels were higher in women compared to men (106±24.7 vs 81.4±24.7; p<0.01) (Table 1).
Baseline characteristics categorized according to sex (in complete cohort, obese and non-obese).
| Variable | Complete cohort (n=81) | Obese (n=28) | Non-obese (n=53) | ||||||
|---|---|---|---|---|---|---|---|---|---|
| Men(n=54) | Women(n=27) | p | Men(n=14) | Women(n=14) | p | Men(n=40) | Women(n=13) | p | |
| Age (years) | 64.5±9.2 | 71.2±8.2 | <0.01 | 64.8±7.7 | 71.3±7.8 | 0.06 | 63.7±9.8 | 71.2±10 | 0.02 |
| Obesity (%) | 26 | 52 | 0.02 | N/A | N/A | – | N/A | N/A | – |
| Diabetes (%) | 41 | 22 | 0.09 | 55 | 55 | 0.99 | 42 | 7 | 0.02 |
| Weight (kg) | 78.6±12.1 | 72.1±11.0 | 0.02 | 91.6±10.1 | 80.1±7.2 | <0.01 | 74.1±9.1 | 63.5±7.2 | <0.01 |
| Height (cm) | 167.1±6.5 | 155.4±5.2 | <0.01 | 167+1±6.3 | 155±4.9 | <0.01 | 167.1±6.6 | 155.9±5.6 | <0.01 |
| BMI (kg/m2) | 28.1±3.5 | 29.8±4.5 | 0.13 | 32.7±2.1 | 32.4±3.5 | 0.74 | 26.49±2.31 | 26.4±1.4 | 0.65 |
| SBP (mmHg) | 138±18 | 141±15 | 0.18 | 143±17 | 145±15 | 0.68 | 135±17 | 138±17 | 0.46 |
| CTRP3 (ng/ml) | 81.4±24.7 | 106±24.7 | <0.01 | 78.6±25.4 | 101.5±16.2 | 0.01 | 78.9±22.3 | 107±29.9 | 0.01 |
| Creatinine (mg/dl) | 1.8±0.4 | 1.6±0.5 | 0.03 | 1.7±1.5 | 1.8±1.6 | 0.95 | 1.8±0.4 | 1.5±0.5 | 0.08 |
| eGFR (ml/min/1.73m2) | 39.3±11.9 | 36.7±10.3 | 0.44 | 40.2±11.2 | 32.1±8.5 | 0.1 | 39.1±11.1 | 37.6±11.4 | 0.88 |
| LDL (mg/dl) | 104.8±44.2 | 124.9±42.3 | 0.06 | 93.7±24.9 | 119±42.3 | 0.16 | 109.7±50.8 | 132.2±41.1 | 0.29 |
| HDL (mg/dl) | 54.6±24.27 | 59.6±11.9 | 0.02 | 52.9±20.1 | 62.6±15.34 | 0.1 | 56.1±27.2 | 57.4±8.4 | 0.26 |
| TAG (mg/dl) | 145±78 | 135±68 | 0.58 | 144±83 | 148±83 | 0.89 | 144±78 | 133+64 | 0.88 |
| HbA1C (%) | 6.6±1.7 | 6.1±0.4 | 0.53 | 6.3±0.9 | 6.1±0.6 | 0.74 | 6.5±1.8 | 6.1±0.4 | 0.91 |
| Uric acid (mg/dl) | 7.1±1.2 | 6.2±1.5 | 0.06 | 7.6±0.8 | 7.1±1.4 | 0.7 | 6.8±1.2 | 5.8±1.3 | 0.06 |
| CRP (mg/dl) | 5.5±7.4 | 6.1±9.6 | 0.77 | 7.1±10.5 | 11.3±12.7 | 0.35 | 5.5±6.9 | 2.1±1.5 | 0.36 |
| ESR (mm/1ah) | 13.3±13.4 | 16.5±8.8 | 0.02 | 12.8±7.4 | 18.2±7.7 | 0.18 | 13.6±16.1 | 14.5±10.1 | 0.15 |
| uACR (mg/g) | 360±711 | 133±451 | 0.04 | 678±1211 | 56±57 | 0.11 | 283±457 | 48±78 | 0.02 |
| Aspirin use (%) | 40.7 | 40.7 | 0.99 | 50 | 57 | 0.71 | 37 | 23 | 0.34 |
Abbreviations (in alphabetical order): BMI=body mass index; CRp=C-reactive protein; CTRP3=C1q/TNFalpha Related Protein 3; eGFR=estimated glomerular filtration rate; ESR=erythrocyte sedimentation rate; HbA1C=glycohemoglobin; HDL=high density lipoprotein; LDL=low density lipoprotein; N/A=non applicable; SBp=systolic blood pressure; TAG=triacylglycerides; uACR=urine albumin creatinine ratio.
In both the obese and non-obese subgroups, CTRP3 was higher in women compared to men (Table 1).
Baseline CTRP3 levels were comparable between diabetics and non-diabetics (92±26 vs 88±27; p=0.46).
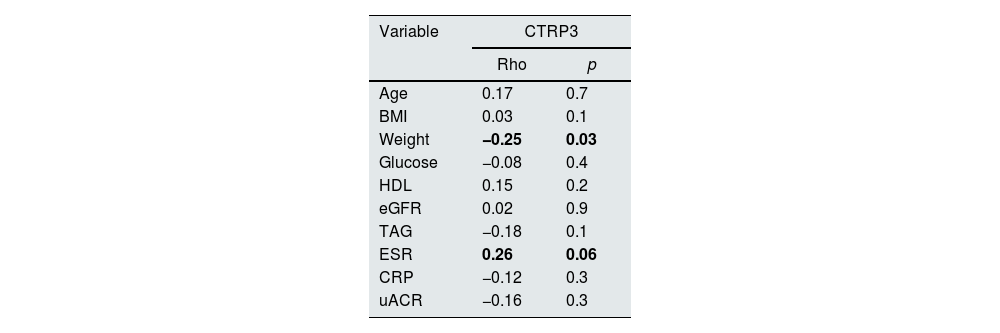
The correlation analysis by non-parametric methods detected that, in the complete cohort, CTRP3 levels are inversely related to weight (Rho −0.25; p=0.03) and positively with ESR (Rho 0.26; p=0.06) although the latter does not reach statistical significance. The other variables, shown in Table 2, showed no statistically significant association.
Correlation between CTRP3 and other variables.
| Variable | CTRP3 | |
|---|---|---|
| Rho | p | |
| Age | 0.17 | 0.7 |
| BMI | 0.03 | 0.1 |
| Weight | −0.25 | 0.03 |
| Glucose | −0.08 | 0.4 |
| HDL | 0.15 | 0.2 |
| eGFR | 0.02 | 0.9 |
| TAG | −0.18 | 0.1 |
| ESR | 0.26 | 0.06 |
| CRP | −0.12 | 0.3 |
| uACR | −0.16 | 0.3 |
Abbreviations (in alphabetical order): BMI=body mass index; CRp=C-reactive protein; CTRP3=C1q/TNFalpha Related Protein 3; eGFR=estimated glomerular filtration rate; ESR=erythrocyte sedimentation rate; HDL=high density lipoprotein; TAG=triacylglycerides; uACR=urine albumin creatinine ratio.
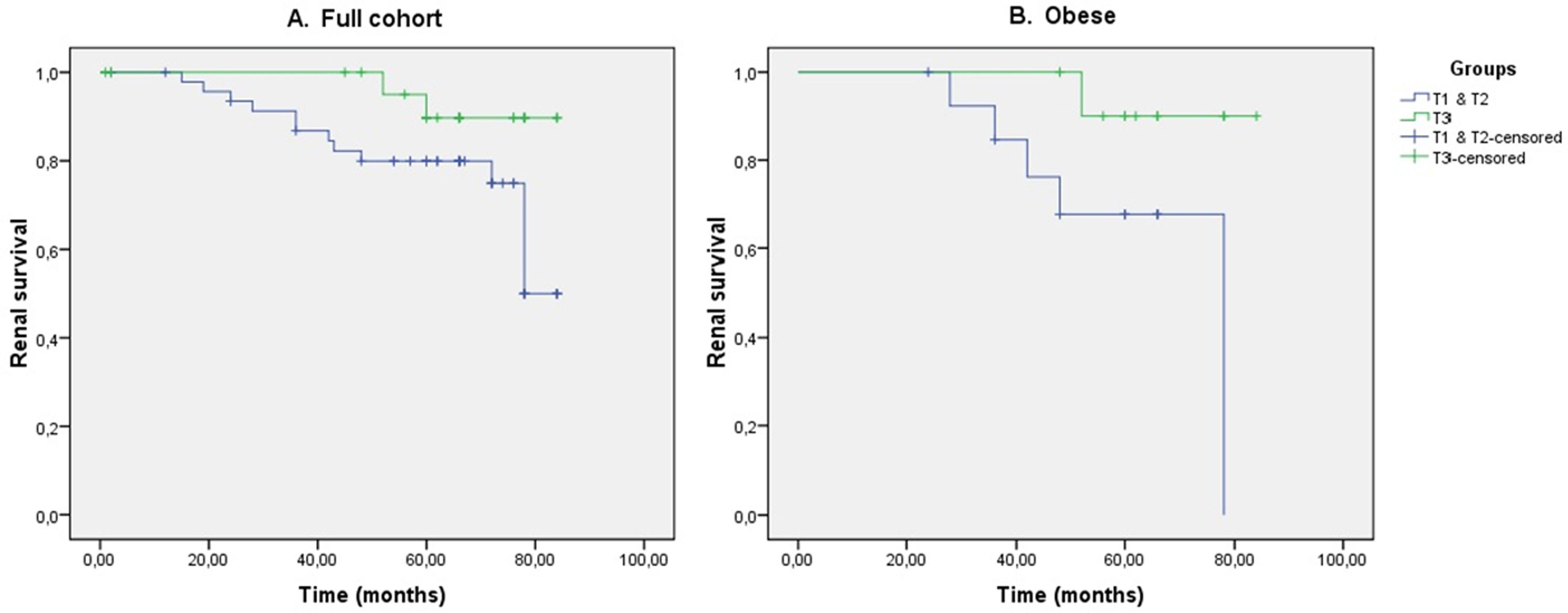
Participants were followed for a mean (±SD) of 64.09±17.88 months. For the renal survival analysis, the patients were categorized according to the CTRP3 levels into two groups, those belonging to the first and second tertile (T1&T2) (n=53) and those belonging to the upper tertile (T3) (n=28). Tertile limits were 74.42 and 105.68 respectively. In the entire cohort, a total of 15 renal events occurred (13 events in T1&T2 and 2 events in T3). Aspirin use in T3 was 48% and in T1&T2 was 37% (p=0.35). Renal survival tended to be better in T3, although the differences did not reach statistical significance (LogRank=3.2; p=0.07) (Fig. 1).
In non-obese patients, 8 renal events were detected in T1&T2 (n=34) and 1 event in T3 (n=13). These differences were not statistically significant (p>0.05). In obese patients, 5 renal events were detected in T1&T2 (n=14) and 1 renal event in T3 (n=11), being this difference statistically significant (LogRank=3.8; p=0.049) (Fig. 1). Finally, it was stratified according to sex and CTRP3 tertiles, without finding statistically significant differences in any subgroup (LogRank=1.6; p=0.2).
The multiple Cox regression analysis confers no predicting power for renal events to CTRP3 levels (HR 0.98; CI95% 0.96–1.06) when adjusted for age, eGFR and uACR.
DiscussionWe present the results of an observational exploratory analysis of the role of CTRP3 in renal disease, showing a potential beneficial impact of higher levels of this new adipokine in kidney disease progression.
CTRP3 is part of a recently described family of adipokines, the C1q/TNF related proteins, is structurally similar to adiponectin and predominantly expressed in adipose tissue.14 Previous studies show that CTRP3 has beneficial endocrine and cardiovascular effects increasing insulin sensitivity,17,22 enhancing triglycerid metabolism and inhibiting gluconeogenesis.13,14 In animal models, recombinant CTRP3 is protective following myocardial infarction or stroke.15 CTRP3 also has anti-inflammatory effects. It has been inversely correlated with TGFbeta, TNFalpha and interleukin-6.14,24
Observational studies in humans show lower levels of CTRP3 in patients with DM or obesity, as well as higher levels in women.14,16–18 This has arisen the hypothesis that CTRP3 may be implicated in the pathogenesis of DM and obesity, being the downregulation of this adipokine an early step in the metabolic disturbances of these diseases.
In our cohort women had higher CTRP3 levels compared to men (106±24.7 vs 81.4±24.7; p<0.01) in both obese and non-obese subgroups (Table 1), consistent with previous reports.14 CTRP3 levels were comparable between obese and non obese patients (90.1±23.8 vs 84.5±6.2; p=0.28) and between diabetic and non diabetic patients (92±26 vs 88±27; p=0.46).
Some of our results contrast to previous reports,14,16–18 specially the absence of differences in CTRP3 levels between obese and non-obese groups. The previous reports compared groups with great BMI differences. In our cohort the non-obese group had BMI>25kg/m2 and the BMI difference with the obese group was modest. A more detailed categorization according to BMI was performed in three groups: NW, OW and OB as detailed in the methods section. CTRP3 levels in these groups were comparable (p=0.13).
Thus, the contrast between our results and previous reports may be due to undetected bias. For example, the mentioned literature is based on patients without CKD, which may impact CTRP3 expression, for example, due to its inherent proinflammatory state. This is an hypothesis that merits further investigation in future studies.
Few studies are published about CTRP3 in patients with CKD and show contradictory results. Moradi et al.21 studied CTRP3 levels in diabetics with and without diabetic nephropathy and in controls and Yavuz et al.22 studied CTRP3 in dialysis, predialysis and control patients. Moradi et al reported in patients with diabetic nephropathy a much higher CTRP3 levels than ours (222.03±51.99ng/ml) and a clear negative correlation between CTRP3 and creatinine (r=−0.389; p<0.01) and TGFbeta and IL-6.21 On the contrary, Yavuz et al.22 reported lower CTRP3 levels than ours (37.2±17.8ng/ml in dialysis patients and 24.6±14.9ng/ml in predialysis patients) and a positive correlation between CTRP3 and creatinine (r=0.31; p<0.001).
Our results are inbetween these two studies. We found no significant correlation between CTRP3 and serum creatinine, eGFR and inflammatory markers (Table 2) although our study is limited to hsCRP and ESR, not including TNFalfa or IL-6, which may be a limitation of our study.
Groups of different studies may not be directly compared because of undetected bias (e.g. selection bias, differences in BMI, in body composition, in the number of diabetics or the absence of control group in our study) but we believe that the contrast between the mentioned studies and ours is worthmentioning and merits further investigation in future studies to explain these differences.
CTRP3 has proved beneficial in vitro kidney effects, such us attenuation of glucose-induced human glomerular mesangial cell dysfunction19 and of inflammatory response stimulated by secretory IgA or regression of renal fibrosis via inhibiting notch signaling pathways.25 Given all this and the fact that other CTRP family members have been associated with better kidney outcomes,26 we explored the impact of baseline CTRP3 in the incidents of renal events. For that purpose patients were followed for 64.09±17.88 months. Renal survival tended to be better in the higher CTRP3 tertile although it did not reach statistical significance (LogRank=3.2; p=0.07). When we compared tertile groups according to baseline BMI or sex, the obese subgroup with higher CTRP3 levels showed better and significant renal prognosis (LogRank=3.8; p=0.049) (Fig. 1). However, CTPR3 failed to predict renal events (HR 0.98; CI95% 0.96–1.06) when adjusted to major risk factors for kidney disease progression.
Some limitations of our study are worthmentioning. The simple size is small. Most of the definitions used are transversal and no longitudinal parameters were recorded (e.g. BMI, diabetes control, etc), which may impact renal prognosis. BMI itself reflects badly the proportion of lean and fat mass, which directly impacts CTRP3 expression. The number of renal events and simple size, specially in subgroups analysis, is too small to reach solid conclusions. Finally, our study has been done in a cohort belonging to the AASER trial. Although aspirin use was comparable in the various subgroups, it would be interesting to confirm our data in a cohort not belonging to a randomized controlled trial.
However, our study also has strengths. To our knowledge, it is the first study to assess the impact of CTRP3 in kidney disease progression and it has a long follow-up period.
ConclusionsIn a cohort of patients with stage 3–4 CKD, CTRP3 levels were similar in patients with and without diabetes or obesity and higher in women. CTRP3 had no correlation with eGFR. Higher CTRP3 levels at baseline were associated with better renal outcomes in obese patients. Further studies are needed in this field to corroborate our data.
Availability of data and materialData and materials support the claims and comply with field standards.
Ethics approvalAll procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. The study was approved by the Bioethics Committee of the Hospital Gregorio Marañón.
Consent to participateInformed consent was obtained from all individual participants included in the study.
FundingThe authors’ research was funded by the Spanish Ministry of Economy and Competitiveness through Fondo de Investigación en Salud grants PI16/02057, PI15/000298 and RED de INvestigación RENal RD016/0019 Fondo Europeo de DEsarrollo Regional funds. Salary support: FIS Miguel Servet (MS14/00133) to M.D.S.-N.
Conflict of interestThe authors declare that there is no conflict of interest regarding the publication of this article.