En este trabajo revisamos los casos que hemos observado en los últimos diez años de enfermos tratados con hemodiálisis periódica que han recuperado la función renal en cuantía suficiente para poder interrumpir dicho tratamiento. Durante el período de estudio, 218 enfermos comenzaron tratamiento con hemodiálisis periódica en nuestro hospital y precisaron diálisis durante más de 90 días. En 17 de ellos (8%), se pudo interrumpir la diálisis, tras haber permanecido en ella un tiempo que osciló entre 95 y 529 días. La probabilidad de recuperación de la función renal fue mayor en los enfermos con nefropatía intersticial crónica (p = 0,04) o con enfermedades autoinmunes (p = 0,07), y en los que comenzaron tratamiento renal sustitutivo con dos sesiones de hemodiálisis a la semana (p = 0,02). No hemos observado diferencias significativas en edad, género, filtrado glomerular al inicio del tratamiento con hemodiálisis o índice de comorbilidad. Siete enfermos volvieron a precisar tratamiento con hemodiálisis tras un período de tiempo sin ella de 11 ± 7 meses. Dos enfermos fallecieron por motivos no atribuibles al tratamiento de la insuficiencia renal y otro salió del estudio por traslado a otro hospital tras haber permanecido 35 meses sin diálisis. Los 14 enfermos restantes están vivos y 8 permanecen libres de diálisis, con un tiempo de evolución que oscila entre 13 y 106 meses. Concluimos que la función renal residual no tiene por qué deteriorarse de forma inexorable tras el inicio de tratamiento con hemodiálisis, y que la posibilidad de recuperación funcional es factible en algunos enfermos.
The aim of this study was to review all cases of recovery of renal function in chronic haemodialysis patients, observed in the last ten years. During the study period, 218 chronic renal failure patients were managed on haemodialysis for a minimum of 90 days. In 17 cases (8%), it was possible to interrupt dialysis after 95 to 529 days. The probability of renal function recovery was higher in patients with chronic interstitial nephritis (P=.04) or autoimmune diseases (P=.07), as well as in those starting haemodialysis treatment at a frequency of two sessions per week (P=.02). No significant differences in age, gender, glomerular filtration rate at the beginning of haemodialysis treatment, or comorbidity rate were observed. Seven patients returned to haemodialysis treatment after a dialysis-free period of 11±7 months. Two patients died for reasons unrelated to renal failure treatment, and another patient was moved to another hospital following 35 months without dialysis. The other 14 patients are alive and 8 are dialysis-free, with a monitoring period of 13 to 106 months. The conclusion reached is that there is no reason why residual kidney function should inexorably worsen after the start of haemodialysis treatment, and that functional recovery is possible in some patients.
INTRODUCTION
Patients with chronic kidney disease that have required dialysis for over 90 days have little chance of recovering enough renal function to warrant removal from renal replacement therapy. In studies based on the data from large-scale registries, only 0.8%-2.5% of patients experienced such a recovery.1-5
Three months is considered to be a sufficient time period for correcting the possible concurrent aggravating factors, and for kidney regeneration mechanisms to have yielded the maximum possible level of renal recovery. On the other hand, the start of renal replacement therapy is accompanied by a rapid reduction in residual renal function, above all when using haemodialysis. The inflammatory response associated with bio-incompatibility and decreased renal perfusion secondary to ultrafiltration and hypotension are dialysis-related factors that contribute to a progressive deterioration in renal function.6,7 As a result, once dialysis treatment reaches a chronic phase, recovery of renal function is a rarity. Additionally, some authors advise against interrupting chronic dialysis even when recovery does occur, stating that the period off dialysis tends to be short and is associated with increased mortality.4
In this study, we review the cases of recovered residual renal function that we observed within the last 10 years. The objective is to evaluate the incidence of this phenomenon and to study the evolution of these patients in order to determine whether this possibility deserves consideration once periodic dialysis treatment has commenced.
MATERIAL AND METHOD
In accordance with the Spanish Society of Nephrology guidelines, our criteria for starting haemodialysis in patients with stage 5 chronic kidney disease was a glomerular filtration rate less than 6ml/min in patients with no other symptoms, or moderately higher GFR levels in patients with uraemic symptoms or heart failure that could not be controlled with conservative treatment.8
We applied our clinical protocol to all patients in the haemodialysis unit, including an analysis of glomerular filtration rate using the mean clearance rates of urea and creatinine. Clearance was calculated using urea and creatinine concentrations measured in 24-hour urine samples prior to the first dialysis session of each week and blood concentrations obtained immediately before starting dialysis. The first measurement, which was usually taken during the first week of treatment, was considered as the baseline glomerular filtration rate. Once treatment with periodic haemodialysis was started, residual renal function was measured every two months.9
Time on dialysis was initially set at 3.5 hours or 4 hours per session, depending on whether dry weight was less than or greater than 60kg, and treatment was started with two weekly sessions (Monday and Friday or Tuesday and Saturday) whenever deemed possible by the attending physician. This regimen of two weekly sessions was maintained as long as residual urea clearance was greater than 2.5ml/min.10 The standard protocol used in our haemodialysis unit for patients receiving dialysis twice per week involved administration of 80mg furosemide on days when not receiving dialysis.
Dry weight is defined primarily based on clinical criteria. For the past five years, we have used bioelectrical impedance vector analysis during the first months of treatment for assistance in avoiding excessive volume depletion. To this end, we have sought to maintain the post-dialysis impedance vector within a 75% tolerance ellipse of the zone corresponding to dehydration (upper pole of the ellipse).11
There have been no standard criteria for indicating an interruption of dialysis treatment in light of recovered residual renal function. As a general rule, this possibility has been considered when residual glomerular filtration rate consistently surpasses 6ml/min and the patient is in a stable clinical condition.
Between January 1 2001 and December 31 2010, 224 patients started treatment with periodical haemodialysis at the haemodialysis unit of the Ramón y Cajal Hospital. Of these, 6 remained on dialysis for less than 90 days (4 due to death and 2 due to recovery of renal function) and were excluded from the analysis. The remaining 218 patients constituted the population examined in our study. Haemodialysis was started using an arteriovenous fistula (planned start) in 50% of these patients (110 cases), and the remaining 108 started haemodialysis with a venous catheter (unplanned start). Two weekly sessions were administered to 73 patients, and three weekly sessions were administered to the other 145 patients. In all cases, we used the same haemodialysis technique with a high-permeability, synthetic, bio-compatible filter membrane (ultrafiltration coefficient >20ml/h/mmHg) and ultrapure dialysate fluid.
The distribution of values for glomerular filtration rate was normal (Kolmogorov-Smirnov test), and we used paired and unpaired Student’s t-tests for comparing means. Qualitative variables were compared using chi-square tests with Yates corrections. We expressed all data as mean and standard deviation. P-values <.05 were considered to be statistically significant.
RESULTS
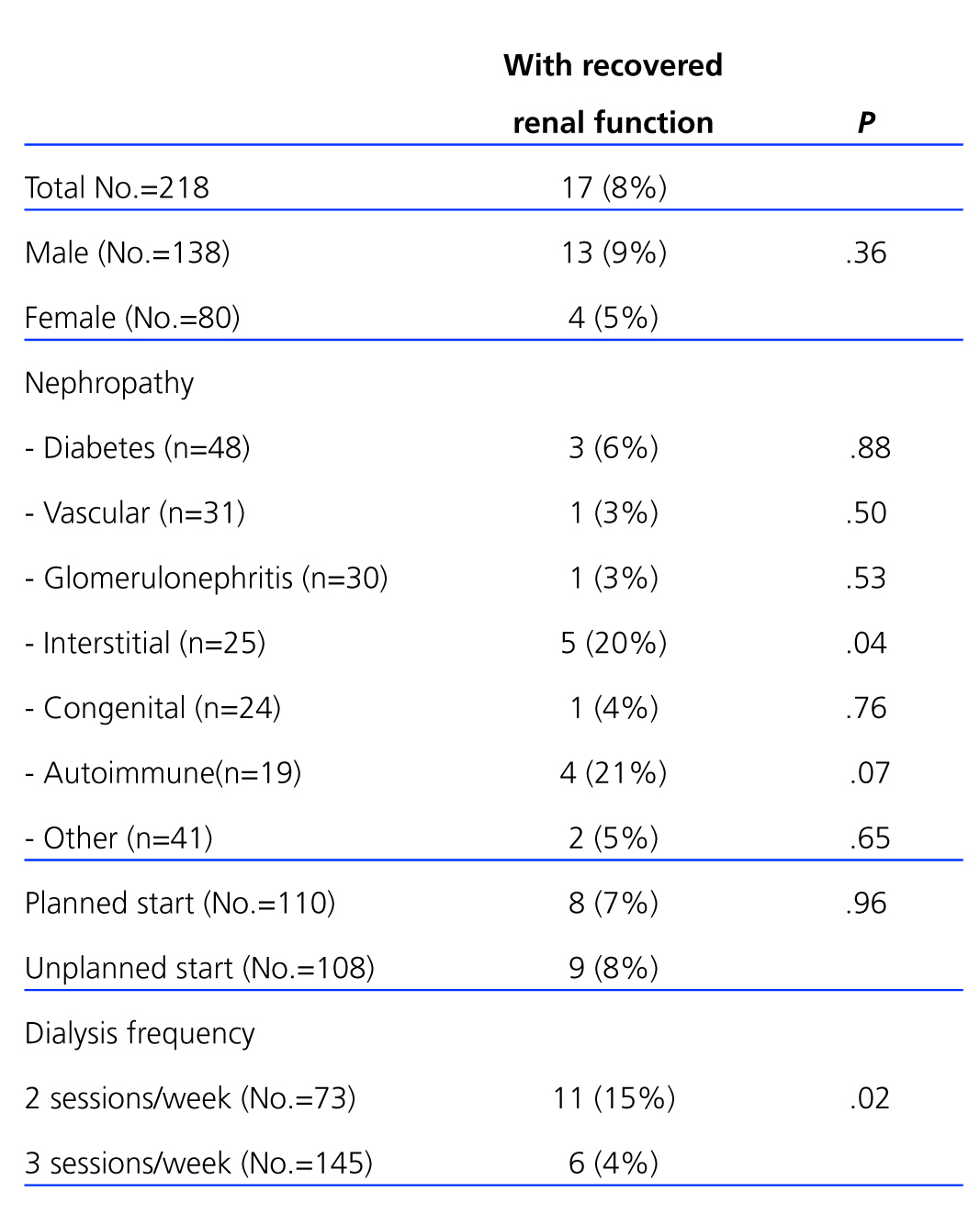
Of the 218 incident patients that received periodical haemodialysis treatment for over 90 days, 17 (8%) recovered enough renal function to warrant suspension of dialysis treatment. In Table 1, we compare data from the start of haemodialysis treatment for the 17 patients that did recover renal function with the remaining 201 patients that did not. The prevalence of chronic interstitial nephropathy and autoimmune disease was higher in patients that recovered renal function, although in the latter this difference was not statistically significant. The start of treatment with a vascular catheter did not affect the evolution of glomerular filtration rate. However, the probability of recovering renal function was greater in the patients that started renal replacement therapy with two weekly sessions. There were no differences between the patients that recovered renal function and those that did not in terms of age (58±15 years vs 62±16 years; P=.32), Charlson comorbidity index (5.9±2.9 vs 6.4±2.7; P=.46), or baseline glomerular filtration rate (6.6±1.8ml/min vs 5.8±2.3ml/min; P=.16).
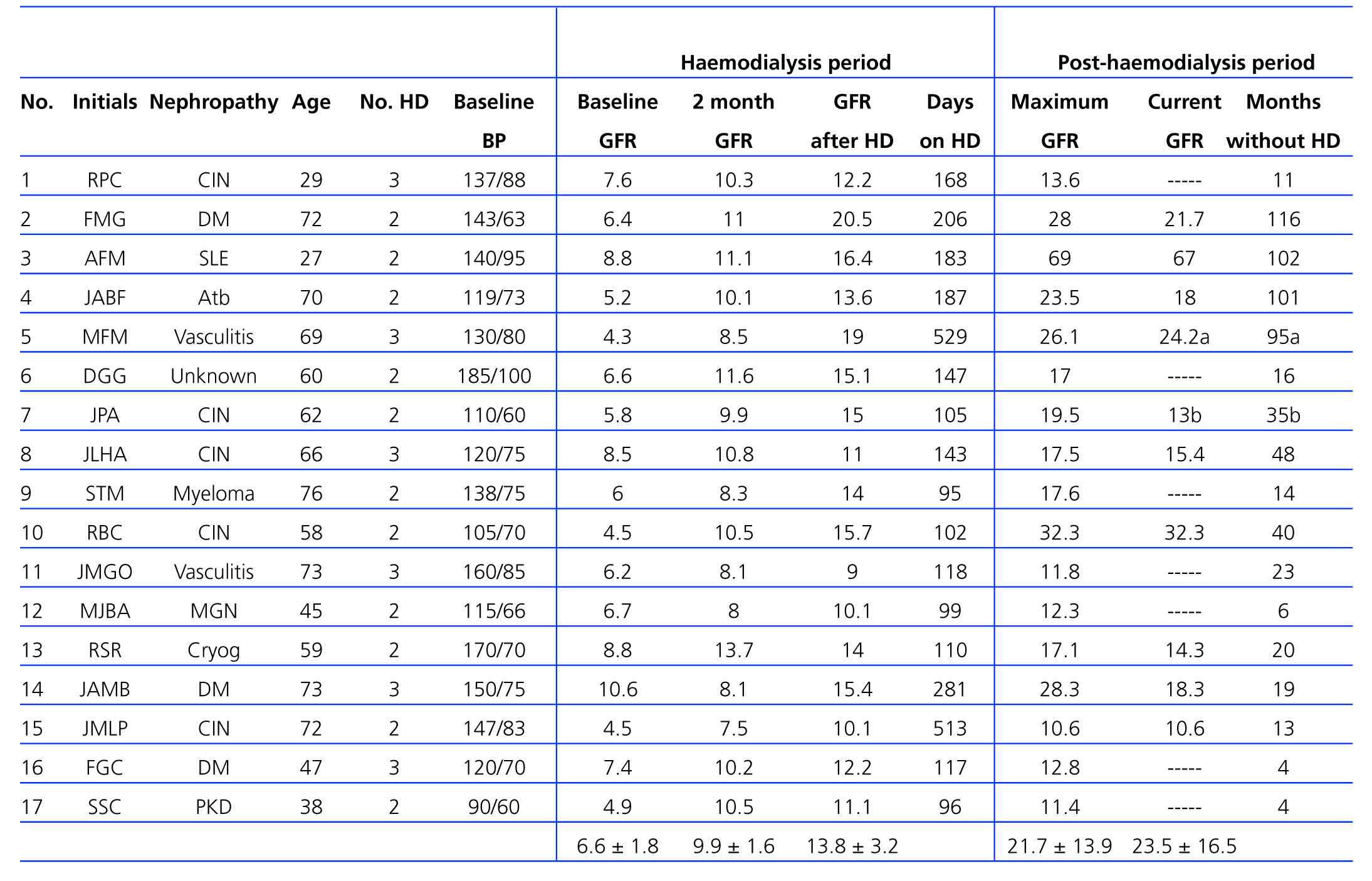
Table 2 shows the clinical characteristics for our patients at the moment of starting renal replacement therapy, the number of sessions per week administered, mean pre-dialysis blood pressure during the first week of treatment, glomerular filtration rate in each patient at the start of haemodialysis (baseline), after two months, and at the moment that HD treatment was suspended, as well as evolution following this point (maximum glomerular filtration rate reached during the dialysis-free period and the value corresponding to the termination of the study in July 2011) for the 17 patients that recovered renal function. The need for dialysis treatment was triggered by hydrosaline retention with dyspnoea in cases 3, 8, and 13, pericarditis in case 14, heart failure with acute myocardial infarction in case 16, and difficulties in controlling arterial hypertension in case 6. In the remaining 11 cases, the start of haemodialysis was indicated based on the criteria of their attending physicians, who evaluated renal function and the appearance of other signs and symptoms attributable to uraemia. Upon starting dialysis, the two patients with vasculitis and the patient with systemic lupus erythematosus received low doses of corticosteroids as an immunosuppressant treatment. In all periods studied, glomerular filtration rate surpassed the baseline value (P<.01 for current glomerular filtration rate and P<.001 for all other values). The mean time on haemodialysis was 188±131 days, and surpassed one year in two patients. Seven patients required haemodialysis treatment once again following a dialysis-free period of 11±7 months. One of these (case 9) died due to the underlying condition (myeloma) 7 months after restarting haemodialysis; the other 6 are still alive, and 3 have received kidney transplants (cases 1, 6, and 11). Of the remaining 10 patients, one (case 5) died due to vascular dementia after 95 months of evolution off dialysis; another patient (case 7) changed locations and hospitals and we were unable to follow his evolution after 35 months post-dialysis follow-up; the remaining 8 patients are still alive and did not require renal replacement therapy when this study came to an end.
We should point out the evolution of case 3: a 27-year old male with systemic lupus erythematosus and diffuse proliferative glomerulonephritis, with major histological and immunological activity, and who evolved towards terminal renal failure within 3 months despite receiving high doses of prednisone and boluses of cyclophosphamide. Upon starting haemodialysis, the treatment with cyclophosphamide was suspended, and the prednisone treatment was rapidly reduced until reaching a maintenance dose of 10mg/day. The gradual improvement in residual renal function allowed for an interruption of dialysis treatment after 6 months; 9 years later, the chronic kidney disease is in stage 2, with normal urinary sediments and proteinuria <500mg/day, with no signs of immunological activity.
DISCUSSION
Although the recovery of residual renal function following treatment with dialysis is a rare occurrence, it should not be considered exceptional. We observed this phenomenon in 8% of our patients that started haemodialysis treatment at our unit over the last 10 years.
A greater probability of functional recovery has been correlated with certain aetiologies of chronic kidney disease, such as auto-immune diseases and interstitial and vascular nephropathies.1-5,12-15 In our study, only interstitial nephropathy had a higher prevalence with statistical significance.
The influence of the type of dialysis on the possibility of recovering renal function remains a controversial subject. Peritoneal dialysis is considered to preserve residual renal function better than haemodialysis, and some series have shown that the recovery of renal function is greater in patients treated with this method.3,16-18 However, other publications that have analysed this topic have concluded that the possibilities of recovering renal function are equally scarce for both techniques.1,5,19
In our study of patients treated with haemodialysis, we observed a higher recovery rate of residual renal function than those published in large patient registries. According to some studies the probability of recovering renal function is greater if patients have a higher glomerular filtration rate when starting renal replacement therapy.5,18 The level of renal failure suffered by the patients that started renal replacement therapy in our study was similar to those reported in other publications,3,5 and we observed no significant differences in terms of baseline glomerular filtration rates between patients that recovered renal function and those that did not. Except for a higher probability of recovering renal function in patients with chronic interstitial nephropathy or autoimmune disease, we were unable to identify other factors that would allow for identifying patients at the start of haemodialysis treatment that have a greater chance of functional recovery. Controlling arterial hypertension may have been the cause for the improvement observed in residual renal function in one of our patients (case 6), although this factor does not appear to have played a relevant role in the rest of the cases we have analysed.
It is possible that the use of post-dialysis bioelectrical impedance vector analysis to establish dry weight and thus avoid states of excessive dehydration, dialysis techniques involving ultrapure water and high-permeability biocompatible membranes, and the start of renal replacement therapy with two weekly sessions all may have been factors that contributed to the maintenance and recovery of renal function in our patients. Sharp drops in volume have been attributed with a rapid loss of renal function in haemodialysis patients.20 During the first few weeks of dialysis treatment, we use a standard post-dialysis bioelectrical impedance vector analysis to determine dry weight, and we attempt to maintain the impedance vector value below the 75% tolerance ellipse, in order to avoid excessive volume depletion. It has been described that glomerular filtration rate is maintained at a better rate with the use of ultrapure water21 and biocompatible membranes,22 although the true benefit of these membranes is still a subject of some controversy.23 In our haemodialysis unit, we place special emphasis on commencing haemodialysis treatment in a progressive manner, attempting to start with two weekly sessions whenever possible. This practice may also have contributed to maintaining residual renal function, since such a correlation has been observed in the past.24,25 Ours being a retrospective study, it is impossible to determine which of the aforementioned factors were the most influential in producing our results.
Angiotensin-converting enzyme inhibitors26 and angiotensin receptor antagonists27 have been used in patients on peritoneal dialysis with the effect of slowing the deterioration of glomerular filtration rate. These drugs are not commonly used in our haemodialysis unit, neither as anti-hypertensive drugs nor to preserve residual renal function. We do administer 80mg per day of furosemide to our patients that undergo two dialysis sessions per week in order to avoid excessive weight gain and to facilitate a more natural water intake. Although furosemide can aid in maintaining diuresis, it has not been shown that this drug has any effect upon the evolution of residual renal function in patients on dialysis.20
Interrupting dialysis treatment due to improvements in residual renal function is a major source of controversy. The authors responsible for the registries of renal patients in Australia and New Zealand advise against this practice, since the dialysis-free period following recovery of renal function is generally short and associated with an increase in mortality rates.4 However, our own experience has been different. Only two of our patients died due to causes not attributable to kidney disease treatment, and the dialysis-free period was longer than 1 year in 13 of our patients.
Periodical measurements of residual renal function are taken on a routine basis for all patients treated with peritoneal dialysis, but this is not a universal practice in all haemodialysis units. Residual renal function has an intrinsic prognostic value, and its measurement is important for quantifying dialysis dosage, understanding the factors that may influence its evolution, and to identify those patients that might benefit from a temporary suspension in dialysis treatment.
We conclude that residual renal function does not necessarily suffer an inexorable deterioration following the start of haemodialysis treatment, and that functional recovery is possible in some patients. A periodical check-up of residual renal function and the adoption of measures to preserve it could contribute to maintaining values at a constant level or even producing a recovery.
Conflicts of Interest
The authors have no conflicts of interest to declare.
Table 1. Baseline values for the study population
Table 2. Clinical results and evolution of glomerular filtration rate in patients that recovered renal function